Treatment of Bradyarrhythmias
This guide provides a comprehensive breakdown of the ACLS Adult Bradycardia With a Pulse Algorithm. Designed for healthcare providers and ACLS learners, this article will teach you how to evaluate symptomatic bradycardia, determine when to intervene, and confidently navigate the stepwise escalation from Atropine to Transcutaneous Pacing and alternative infusions.
ACLS Certification Association videos have been peer-reviewed for medical accuracy by the ACA medical review board.
Article at a Glance
- Atropine is the first-line drug of choice for the treatment of symptomatic bradycardia unless contraindicated.
- Alternative drugs are dopamine and epinephrine. They’re administered via intravenous infusion and are titrated to patient response.
- Transcutaneous pacing is an alternative to drug therapy, though it is a stopgap measure.
- Clinicians should consult a cardiologist when treating patients with bradyarrhythmias.
Adult Bradycardia With a Pulse Algorithm
Read: Bradyarrhythmias
What’s the most appropriate treatment for Bradyarrhythmia?
Interpreting the algorithm in a high-stress scenario requires a clear, step-by-step approach. You must decide if the slow heart rate is actually causing the patient harm, and if so, rapidly escalate therapies until perfusion is restored.
- Assess Clinical Instability: Determine if the bradycardia (typically <50 bpm) is causing symptoms. Look for hypotension, acutely altered mental status, signs of shock, ischemic chest discomfort, or acute heart failure. If the patient is stable, simply monitor and observe.
- First-Line Intervention (Atropine): If the patient is unstable, administer an initial IV push of Atropine.
- Reassess Response: Did the Atropine increase the heart rate and resolve the symptoms? If yes, continue to monitor. If no, or if Atropine is contraindicated, you must escalate immediately.
- Escalate Therapy: Move directly to Transcutaneous Pacing (TCP) or begin a continuous IV infusion of Dopamine or Epinephrine.
Targeting the Underlying Drivers of Bradycardia
While ACLS interventions stabilize the patient, providers must simultaneously evaluate and address reversible contributing causes. If you only treat the rate without treating the cause, the patient will inevitably deteriorate again.
Common Reversible Causes Checklist:
- Hypoxia: Ensure airway patency and administer oxygen.
- Toxins/Medications: Screen for overdoses of beta-blockers, calcium channel blockers, or digoxin.
- Electrolytes: Check a rapid panel for severe hyperkalemia.
- Ischemia: Obtain a 12-lead ECG to rule out an acute myocardial infarction (particularly inferior MI).
Atropine
When intervention is required, Atropine is the first-line pharmacologic therapy.1 It is an anticholinergic drug that antagonizes the muscarinic actions of acetylcholine by blocking parasympathetic influences, thereby increasing heart rate and AV conduction.
It is used to temporarily improve bradyarrhythmias until a more permanent solution, such as a transvenous pacemaker, can be applied. The current ACLS dose to correct bradycardia is an IV bolus of 1 mg administered every 3–5 minutes as needed, up to a maximum total dose of 3 mg.2
For a deep dive into the precise mechanism of action and proper push techniques, watch our clinical review on Atropine in ACLS.

Atropine is an anticholinergic drug which increases the heart rate and atrioventricular conduction.
Precautions and When Atropine Will Fail:
- High-Grade Blocks: Atropine is generally ineffective for Mobitz Type II second-degree blocks and Third-Degree AV blocks with wide QRS complexes. Do not delay transcutaneous pacing for these patients.
- Acute MI: Clinicians must use caution in patients with an acute myocardial infarction; increasing the heart rate increases myocardial oxygen demand, potentially worsening ischemia.
- Heart Transplants: Atropine is ineffective for post-heart transplant patients because they lack the vagal innervation essential for the drug’s antimuscarinic effects.3
If the bradycardia is caused by toxicologic factors (e.g., a massive beta-blocker or calcium-channel blocker overdose), Atropine will likely not be enough to overcome the receptor blockade. In these instances, you must move quickly to the Alternative Infusions (Dopamine/Epinephrine) or specialized antidotes (like Glucagon).
Transcutaneous/Transvenous Pacing
Transcutaneous pacing is a painful but life-saving temporary intervention used to treat symptomatic bradycardia until expert consultation is available and a permanent transvenous pacemaker can be placed.
When to pace early (Bypassing Atropine):
Do not wait to see if Atropine works; prepare and apply pacing pads immediately if the patient presents with:
- A Second-Degree AV block (Mobitz type 2).
- A Third-Degree AV block with a wide QRS complex (indicating a non-nodal block).
- A history of a heart transplant (where vagal innervation is absent).
Reassess and Monitor: Continuous ECG and hemodynamic blood pressure monitoring are vital during pacing. You must confirm mechanical capture (a palpable pulse matching the pacer spikes) rather than just electrical capture on the monitor. If transcutaneous pacing fails to capture or stabilize the patient, expert consultation for immediate transvenous pacing is required.
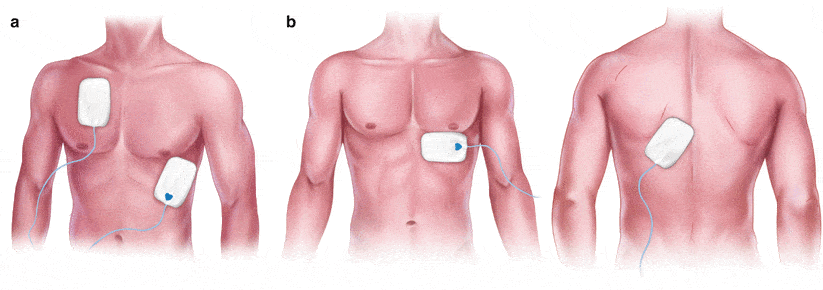
Transcutaneous Pacing
Alternative Infusions: Epinephrine and Dopamine
If Atropine fails to achieve its therapeutic effect and transcutaneous pacing isn’t immediately available (or is ineffective), providers must initiate an IV infusion of either Dopamine or Epinephrine. These are also the treatments of choice if the bradycardia is driven by a toxicological overdose (beta-blocker/calcium channel blocker).
Dopamine Infusion
Dopamine is a catecholamine with alpha- and beta-adrenergic effects that increase both heart rate and blood pressure. Review the precise mixing and titration guidelines in our Dopamine ACLS drug review.
- Dose: 5–20 mcg/kg/minute.
- Titration: Titrate slowly to the patient’s response and taper off slowly when discontinuing.
- Caution: At higher doses, it causes severe vasoconstriction. Use extreme caution if the patient is at risk for acute myocardial infarction.
Epinephrine Infusion
Epinephrine has similar chronotropic and inotropic effects to dopamine but relies on a standard fixed infusion rate rather than weight-based dosing. Refresh your knowledge on these specific receptor actions by watching our Epinephrine ACLS drug review.
- Dose: 2–10 mcg/minute.
- Titration: Titrate precisely to the patient’s blood pressure and heart rate response.
Summary
Per the most current AHA ACLS guidelines, treatment for bradycardia is strictly driven by the presence of unstable symptoms. If the patient is unstable, the initial pharmacological treatment is a 1 mg IV push of Atropine. If Atropine is ineffective or if the patient presents with a high-grade block, providers must rapidly escalate the pathway to Transcutaneous Pacing or initiate a continuous infusion of Dopamine or Epinephrine.
Providers must continually reassess the patient’s vital signs and monitor their ECG while actively searching for and treating underlying, reversible causes. As temporary interventions take effect, prepare to consult a cardiology specialist regarding the need for a permanent pacemaker.
More Free Resources to Keep You at Your Best
Editorial Sources
ACLS Certification Association (ACA) uses only high-quality medical resources and peer-reviewed studies to support the facts within our articles. Explore our editorial process to learn how our content reflects clinical accuracy and the latest best practices in medicine. As an ACA Authorized Training Center, all content is reviewed for medical accuracy by the ACA Medical Review Board.