Ventricular Rhythms and Asystole
Ventricular rhythms and asystole are ECG findings that range from common ectopic beats to life threatening arrest rhythms. This guide explains what ventricular rhythms are, how to recognize PVCs, ventricular tachycardia, ventricular fibrillation, idioventricular escape rhythms, and how to confirm true asystole. You will also learn key ECG criteria, high risk patterns like R on T and multifocal PVCs, and when a rhythm is shockable versus nonshockable.
ACLS Certification Association videos have been peer-reviewed for medical accuracy by the ACA medical review board.
Table of Contents
- What Are Ventricular Rhythms?
- Premature Ventricular Complexes
- Unifocal and Multifocal PVCs
- R-on-T Phenomenon
- Runs and Couplets
- Grouped Beating
- Ventricular Tachycardia
- Ventricular Fibrillation
- Ventricular Escape Rhythm (Idioventricular Rhythm)
- Asystole
- Summary
- Frequently Asked Questions About Ventricular Rhythms
Article at a Glance
- Ventricular arrhythmias arise from the ventricles and have a unique and sometimes bizarre appearance.
- Premature ventricular complexes occur singly or as part of a pattern.
- Ventricular tachycardia is a potentially lethal rhythm with a unique appearance
- In ventricular fibrillation, the heart quivers or “fibrillates,” rendering the ventricles unable to fill with blood.
- Asystole is often referred to as “flat line” and indicates there is no longer any electrical activity in the heart. This differs from conduction delays such as first degree heart block, where electrical activity is present but slowed.
Ventricular rhythms are rhythms that originate from an ectopic focus within the ventricles rather than the atria or AV junction. In contrast, supraventricular irregularities such as a premature atrial contraction arise from atrial ectopic activity. Because the impulse starts outside the normal conduction pathway, ventricular depolarization often spreads cell to cell, which commonly produces a wide QRS complex greater than 0.12 seconds. Ventricular rhythms include premature ventricular complexes (PVCs), ventricular tachycardia (VT), ventricular fibrillation (VF), and ventricular escape rhythms such as idioventricular rhythm or junctional escape rhythm. Some supraventricular rhythms can also appear wide if there is aberrant conduction, so interpretation depends on the clinical context and the overall ECG pattern. In general, the more unstable the patient and the wider and faster the rhythm, the more urgent it is to treat as a potentially dangerous ventricular rhythm.What Are Ventricular Rhythms?
The QRS complex represents ventricular depolarization. When impulses are generated from the ventricles, the QRS complexes widen and are greater than 0.12 seconds. Other supraventricular rhythms may also present with prolonged QRS complexes if there is an impulse conduction disturbance from a supraventricular focus into the ventricles.
Normally, the atria contract first, followed by the ventricles, allowing blood to fill the ventricles. When the ventricles contract, a sufficient amount of blood is ejected into the systemic circulation. If the ventricles contract before the atria, the heart’s efficiency is significantly reduced because only a small amount of blood is available to supply the entire body.1
Ventricular arrhythmias include premature ventricular complexes, ventricular tachycardia, ventricular fibrillation, and idioventricular rhythms. The ventricular escape rhythm is the last line of defense in a heart with a severely compromised conduction system.
Ventricular Rhythms and Asystole
This video reviews the key ventricular rhythms covered on this page and explains why ventricular rhythms often look wide on ECG. It also reinforces the difference between shockable heart rhythms like VF and some forms of VT, versus nonshockable rhythms like asystole. Watch the video to connect ECG recognition with ACLS priorities.
Premature Ventricular Complexes
Premature ventricular complexes (PVCs) are early ventricular beats that interrupt an underlying rhythm. They are common and can be benign, but frequent PVCs or specific patterns can indicate increased myocardial irritability. A PVC typically appears as an early wide QRS complex without a preceding P wave, often followed by a compensatory pause. Recognition matters because PVC patterns can precede more dangerous ventricular rhythms in high-risk settings.
What are PVCs (Premature Ventricular Contractions)?
This short video explains what PVCs are, why they occur, and what makes them easy to recognize on ECG. It also clarifies how PVCs differ from supraventricular beats and why a wide early beat without a preceding P wave is a common clue. Watch the video explaining what PVCs are before reviewing detailed ECG criteria.
ECG Rhythm Review: PVCs
This video focuses on how PVCs look on rhythm strips, including the wide QRS, lack of a preceding P wave, and the compensatory pause. It is helpful for pattern recognition and for spotting PVCs within a baseline rhythm. Watch the video showing the ECG rhythm of PVCs for visual examples.
The premature ventricular complex (PVC) is a single ectopic beat coming from an irritable focus that supersedes the sinoatrial (SA) impulse. It is not a rhythm but rather a single entity disrupting the core rhythm. It occurs earlier than expected in the cardiac cycle.
PVCs have no P wave because the impulse originates in the ventricles, so there’s no atrial depolarization from the sinoatrial node. The QRS complex is wide and more than 0.12 seconds.
A striking feature of PVCs, making them easy to spot, is the T wave morphology opposite the deflection of normal QRS complexes.
Pathologic Signs: Multifocal PVCs and R on T Phenomenon
Most isolated PVCs can be incidental, but certain PVC patterns suggest increased risk and may signal myocardial irritability. Multifocal PVCs and the R on T phenomenon are especially important because they can precede ventricular tachycardia or ventricular fibrillation in vulnerable patients. The following patterns should be documented clearly and interpreted in clinical context.
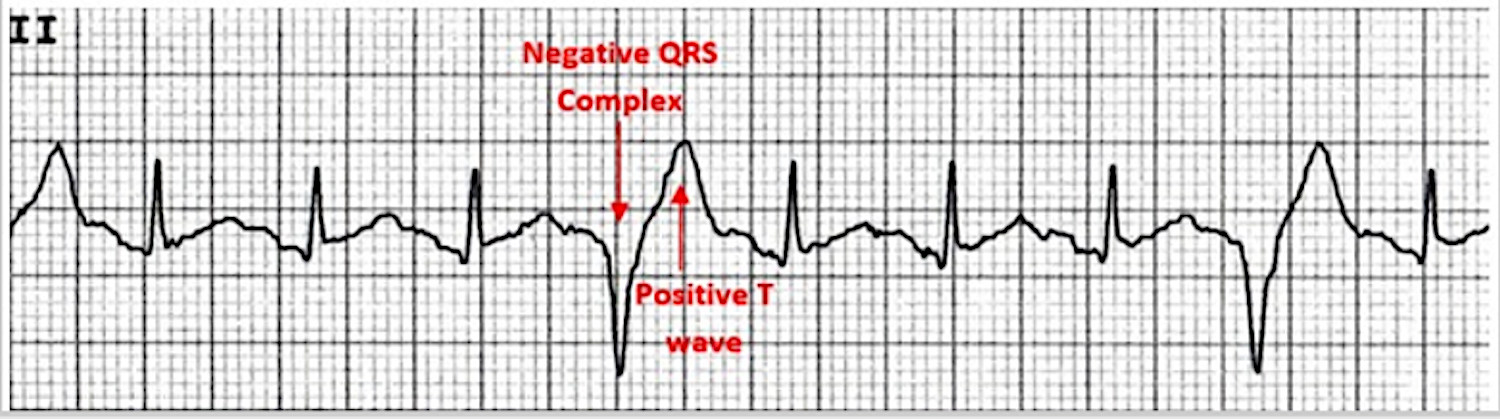
An ECG displays a QRS complex with a negative deflection followed by a T wave with a positive deflection.
During a PVC, a compensatory pause follows the ectopic beat. The underlying rhythm remains unchanged because the impulse generated from the ventricles does not affect the impulses from the sinoatrial node, enabling the SA node to discharge at the expected time.
In the figure below, the arrows indicate PVCs. A dropped R wave follows the PVC. That compensatory pause does not affect the core rhythm because the SA node discharges at its own pace.
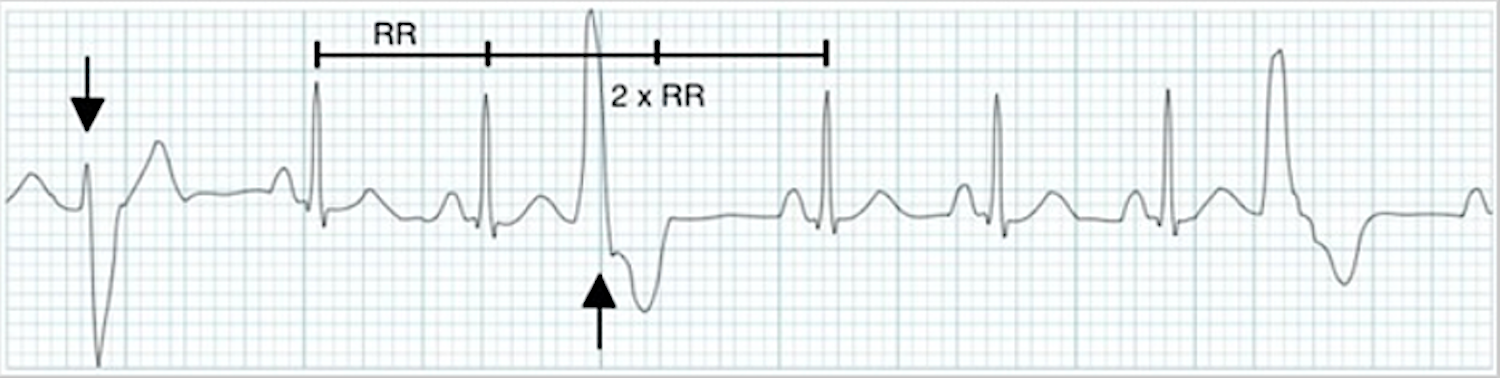
ECG tracing displays PVCs with a dropped R wave.
It’s possible a PVC occurs between regular complexes without disturbing the regular pattern of the sinoatrial node. That phenomenon is known as an interpolated premature ventricular complex.2
PVCs are caused by myocardial irritability. When multiple PVCs occur within one minute, it is pathologic. Chest pain associated with PVCs can be life-threatening, sometimes requiring antiarrhythmic intervention such as lidocaine in ACLS. Clinicians must report PVCs in ECG documentation.
Unifocal PVCs originate from one irritable focus and have the same morphology throughout. Multifocal PVCs occur when multiple PVC morphologies are present. Multifocal PVCs are more serious than unifocal PVCs.Unifocal and Multifocal PVCs
When the R wave of a PVC overlaps the T wave of the core rhythm, it’s known as an R-on-T phenomenon. It’s the result of a relative refractory state of the T wave. Some of the charges are still polarized secondary to a strong ventricular depolarization, precipitating more dangerous rhythms, such as ventricular tachycardia or ventricular fibrillation.R-on-T Phenomenon
Clinicians must suspect increased myocardial irritability when PVCs occur in succession without a normal beat intervening. A couplet is two successive PVCs. Three or more PVCs in a row is known as a run. Clinicians should document the number of PVCs. When several PVCs occur in a row, the normal pacemaker can’t resume, causing significant irritability.Runs and Couplets
Grouped Beating
When a pattern forms between PVCs and normal beats, it’s known as grouped beating. When a PVC occurs between every other normal complex, it’s known as bigeminy. One PVC followed by two sinus complexes is known as trigeminy. If a PVC is followed by three sinus complexes, it’s a quadrigeminy.
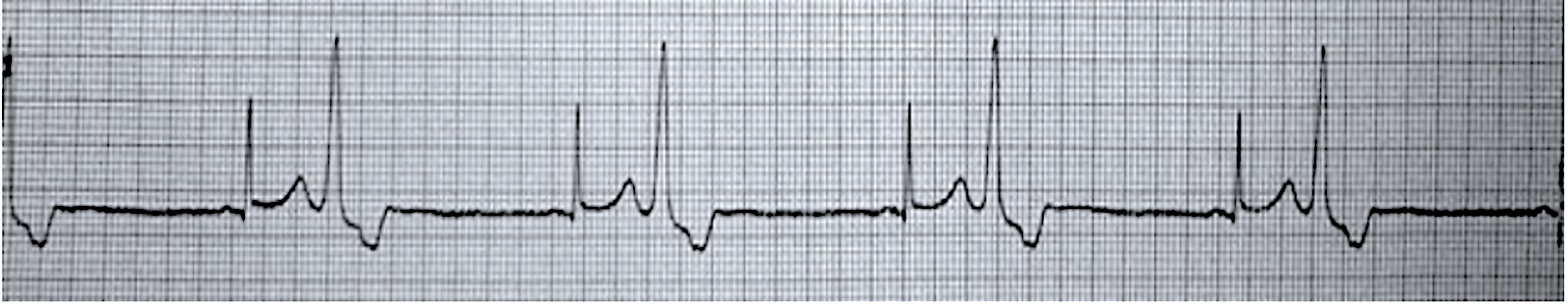
An ECG tracing displays bigeminy, where every second beat is a PVC. The underlying rhythm is sinus rhythm.
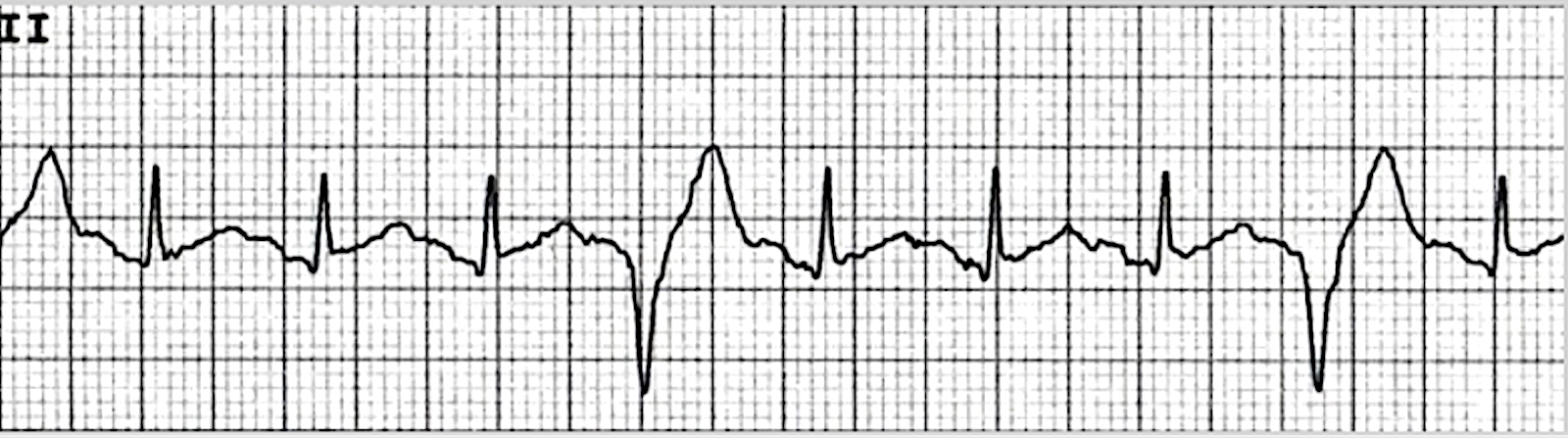
An ECG tracing displays quadrigeminy, where every fourth beat is a PVC.
How Can I Remember the PVCs?
This short memory-focused video gives simple cues to help you spot PVCs quickly, including wide early beats, absent preceding P waves, and the compensatory pause. It is useful for students and clinicians to build pattern recognition. Watch the remember the PVCs lesson for quick reinforcement.
ECG Criteria for Premature Ventricular Complexes (PVCs)
- RATE: depends on the core rhythm.
- RHYTHM: depends on the core rhythm.
- P WAVES: will not be preceded by a P wave; dissociated P waves may be seen near the PVC.
- PR INTERVAL: no PR interval because the focus comes from the ventricles.
- QRS COMPLEX: wide and bizarre QRS complex, 0.12 seconds or greater; T wave is usually the opposite direction from the P wave.
Read: Introduction to ECG Interpretation
Ventricular Tachycardia
Ventricular tachycardia (VT) originates from an extremely irritable focus that overrides the higher pacemaker sites, causing a sustained PVC run. VT is classified as an arrhythmia and has a rate of 150 to 250 beats per minute (bpm).3
The R-R interval may have a slightly irregular appearance, but the complexes are generally uniform in morphology. Like PVCs, VT will have bizarre-looking QRS complexes 120 milliseconds (0.12 seconds) or longer and a T wave deflection opposite the R waves. P waves will not be seen before the QRS complexes.
VT patients will have serious signs and symptoms due to the insufficient blood flow to the body as the ventricles are beating too quickly to fill with blood. Most patients will be unconscious, and a pulse may or may not be felt. Patients in slow VT may be conscious.4
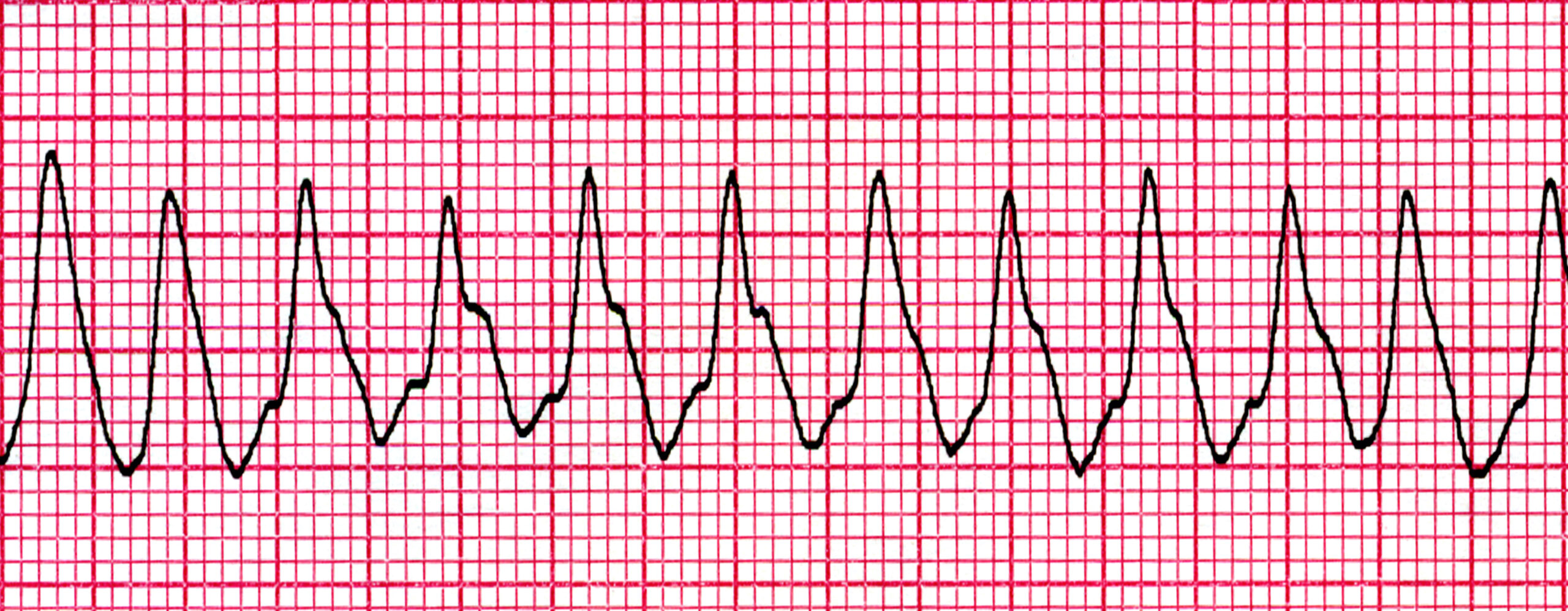
An ECG strip showing ventricular tachycardia.
Non-sustained versus sustained VT: Ventricular tachycardia is often divided into non-sustained VT and sustained VT. Non-sustained VT refers to a VT run that terminates spontaneously, while sustained VT persists and may require intervention. This threshold is clinically important because sustained VT is more likely to produce hemodynamic instability and may progress to ventricular fibrillation.
Fusion and capture beats: In some VT rhythms, occasional beats can look narrower or have a hybrid appearance. A capture beat occurs when a sinus impulse briefly conducts through and produces a normal-looking QRS during VT. A fusion beat occurs when a sinus impulse and a ventricular impulse occur together, producing a QRS that looks like a blend of normal and ventricular morphology. These findings support the diagnosis of VT when wide complex tachycardia is being evaluated.
ECG Rhythm Review: Ventricular Tachycardia
This video reviews the classic ECG features of VT, including wide complex tachycardia patterns and how to recognize VT quickly in clinical settings. It reinforces why VT is potentially lethal and how rhythm recognition influences immediate management. Watch the video showing the ECG rhythm of VT for examples and visual cues.
ECG Criteria for Ventricular Tachycardia (VT)
- RATE: 150–250 bpm; can exceed 250 bpm when VT progresses to ventricular flutter; slow VT is characterized by a rate of less than 150 bpm.
- RHYTHM: usually regular; can be slightly irregular.
- P WAVES: complexes will not be preceded by P waves; dissociated P waves may be seen.
- PR INTERVAL: no PR interval because the focus is in the ventricles.
- QRS COMPLEX: wide and bizarre; 0.12 seconds or greater; T wave is usually in the opposite direction of the R wave.
How is Ventricular Tachycardia (VT) Treated?
VT treatment depends on whether the patient has a pulse and whether they are stable. If the patient is pulseless, treat as cardiac arrest and follow ACLS shockable rhythm priorities. If the patient has a pulse, assess for instability such as hypotension, altered mental status, shock, ischemic chest discomfort, or acute heart failure. Unstable VT generally requires immediate synchronized cardioversion. Stable wide complex tachycardia may be treated with antiarrhythmic therapy based on clinician judgment and protocol, while preparing for escalation if the patient deteriorates.
In ventricular fibrillation (VF), an extremely irritable ventricular focus causes impulses to fire in such a chaotic manner that the ventricles begin fibrillating. In essence, the heart merely quivers rather than beating forcefully. Ventricular fibrillation is a lethal arrhythmia because the fibrillating heart does not send blood to the rest of the body.5 VF has a distinct pattern and is one of the easiest arrhythmias to identify. There are no waves or complexes. It is a simple, grossly chaotic fibrillatory pattern. Patients in VF will be unconscious, apneic, and lack any palpable pulses. VF is often preceded by ventricular tachycardia. The “cure” for both VT and VF is electricity. Defibrillation “shocks” the heart out of its chaotic rhythm, allowing the heart’s normal pacemaker to take over again. Fine VF: Ventricular fibrillation can appear coarse or fine. Fine VF has very low amplitude fibrillatory activity and can sometimes be mistaken for asystole on a quick look. If a patient appears to be in asystole but the clinical picture suggests a shockable rhythm, clinicians should confirm the rhythm in multiple leads and adjust gain before concluding it is true asystole. This helps reduce the risk of missing fine VF.Ventricular Fibrillation
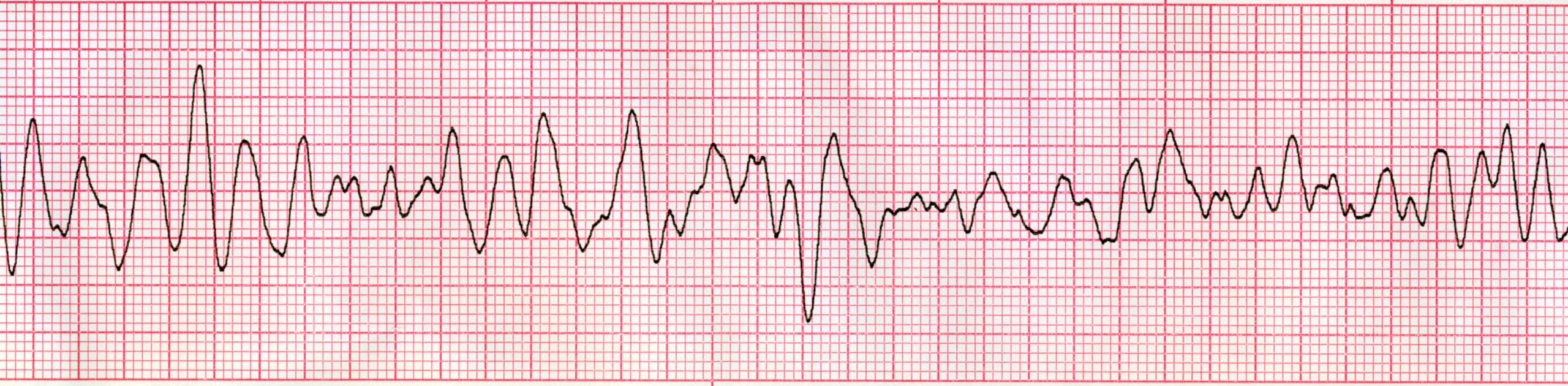
Ventricular fibrillation is treated with defibrillation with the goal of restoring a normal rhythm.
ECG Rhythm Review: Ventricular Fibrillation
This video shows what VF looks like on ECG and reinforces why VF is immediately shockable. It helps differentiate VF from artifact and highlights the urgency of defibrillation and CPR. Watch the video showing the ECG rhythm of VF for visual examples.
An idioventricular rhythm is produced by an escape beat. When higher pacemaker sites fail to produce an impulse, a ventricular escape rhythm takes place in the form of an idioventricular rhythm. Idioventricular rhythms have a rate of 20–40 bpm. If the rate is slower than 20 bpm, it is an agonal rhythm because the heart is on the brink of ceasing all activity. An accelerated idioventricular rhythm is possible when the rate is above 40 bpm. An idioventricular rhythm is produced by an escape beat. Because the impulse is generated from the ventricles, there are no P waves. The escape mechanism has taken over the failed atrial pacemaker sites. Clinicians will observe very slow ventricular complexes with a regular rhythm which may occasionally be irregular. The ventricular complexes are 120 milliseconds (0.20 seconds) or longer. Accelerated idioventricular rhythm (AIVR) is a ventricular rhythm that resembles an idioventricular escape rhythm but occurs at a faster rate, typically above 40 bpm. It can be seen when ventricular automaticity increases, sometimes in reperfusion settings. The rhythm is usually regular, the QRS is wide, and P waves are absent or dissociated. AIVR is often transient, but interpretation should always consider symptoms, blood pressure, and the broader clinical situation. Management depends on patient stability and the cause. A ventricular escape rhythm is often a sign of a failing conduction system or severe physiologic compromise. If the patient is unstable, treat the underlying cause and support perfusion and oxygenation. If the rhythm reflects a bradycardic state with poor perfusion, escalation may be needed per bradycardia management principles. If the patient is stable and the rhythm is transient, clinicians may monitor closely while evaluating reversible contributors such as hypoxia, ischemia, electrolyte abnormalities, or medication effects.Ventricular Escape Rhythm (Idioventricular Rhythm)
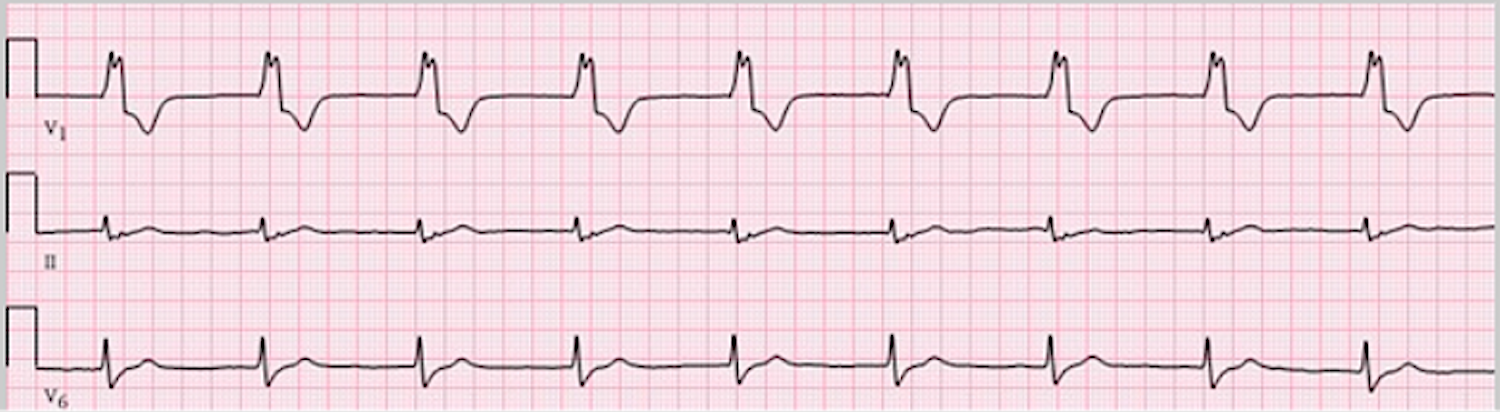
Identifying Accelerated Idioventricular Rhythm (AIVR)
How is Idioventricular Rhythm Managed?
ECG Rhythm Review: Idioventricular Rhythm
This video shows how ventricular escape rhythms appear on ECG, including the slow rate, wide complexes, and absent P waves. It also helps distinguish idioventricular escape rhythms from other wide complex rhythms. Watch the video showing the ECG of idioventricular escape rhythm for visual confirmation.
ECG Criteria for Ventricular Escape Rhythm
- RATE: 20–40 bpm; can be slower (agonal) or faster (accelerated).
- RHYTHM: regular.
- P WAVES: none.
- PR INTERVAL: none.
- QRS COMPLEX: wide and bizarre; 0.12 seconds or longer.
Asystole
Asystole is when all the electrical activity in the heart stops, resulting in a straight or “flat line” pattern.6 It is a lethal arrhythmia and almost always is resistant to resuscitation efforts. The patient in asystole is, for all intents and purposes, deceased.
Hs and Ts: Treating Asystole
This video focuses on cause-driven management for asystole using the Hs and Ts checklist. It reinforces the importance of confirming true asystole, continuing high-quality CPR, and rapidly searching for reversible causes during rhythm checks. Watch the video about the Hs and Ts for treating Asystole for a structured approach.
Clinicians must ensure patients with a flat isoelectric line are truly in asystole and not another rhythm such as a fine VF. They should also rule out machine or operator error by checking the rhythm in several leads other than Lead ll.
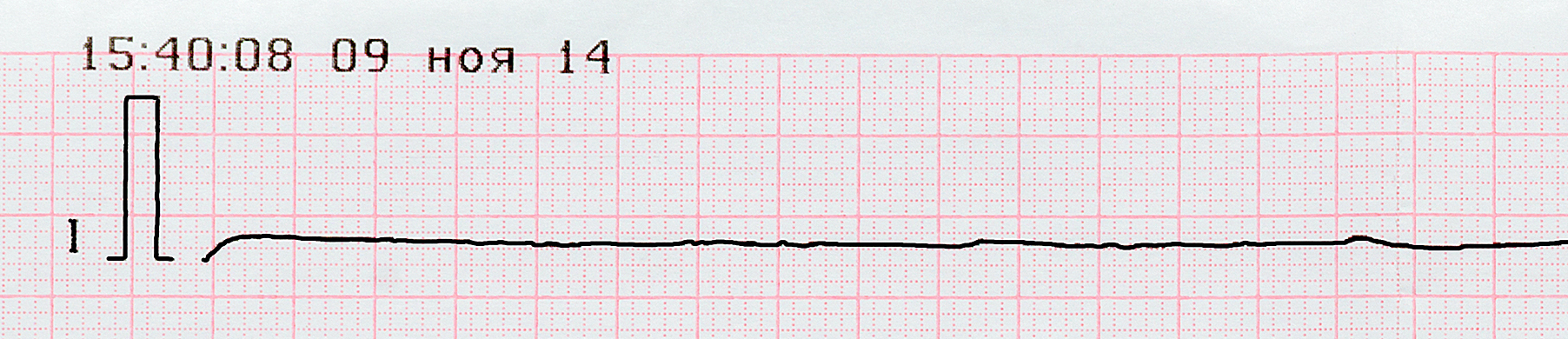
Asystole is represented by a “flat line,” which is a cessation of electrical activity.
VT vs VF vs Asystole Comparison
| Rhythm | Rate | Rhythm Pattern | Shockable |
|---|---|---|---|
| Ventricular Tachycardia (VT) | Typically 150 to 250 bpm | Wide complex tachycardia, often regular | Shockable if pulseless |
| Ventricular Fibrillation (VF) | No measurable rate | Chaotic fibrillatory waveform, coarse or fine | Shockable |
| Asystole | No rate | Flat line, no organized ventricular activity | Not shockable |
Ventricular arrhythmias come from the ventricles. They have fairly unique and bizarre ECG appearances. Premature ventricular complexes either occur solely or with others. VT is potentially lethal while in VF the heart’s ventricles can’t fill with blood. Asystole occurs when the heart lacks electrical activity. Each ventricular arrhythmia has its own heart rate, rhythm, P wave placement, PR interval, and QRS complex.Summary
Frequently Asked Questions About Ventricular Rhythms
Can ventricular arrhythmias be prevented?
Some risk can be reduced by treating underlying causes such as ischemia, electrolyte abnormalities, medication effects, and uncontrolled heart disease. Prevention depends on the specific diagnosis and a clinician-guided plan.
Does heart failure cause VT?
Heart failure can increase the risk of VT because structural heart changes and myocardial scarring can create reentry pathways and increase electrical instability.
Who is at risk for VT?
Higher risk groups include patients with prior myocardial infarction, cardiomyopathy, structural heart disease, significant electrolyte abnormalities, or a history of ventricular arrhythmias.
How common are ventricular arrhythmias?
Isolated PVCs are common in many populations. Sustained VT and VF are less common but carry a higher risk and often occur in patients with underlying heart disease.
Is accelerated idioventricular rhythm (AIVR) ever exercise-induced?
AIVR can occur in situations where ventricular automaticity increases. If it occurs with symptoms or hemodynamic changes, it should be assessed in a clinical context.
More Free Resources to Keep You at Your Best
Editorial Sources
ACLS Certification Association (ACA) uses only high-quality medical resources and peer-reviewed studies to support the facts within our articles. Explore our editorial process to learn how our content reflects clinical accuracy and the latest best practices in medicine. As an ACA Authorized Training Center, all content is reviewed for medical accuracy by the ACA Medical Review Board.
1. Jordan King; David R. Lowery. Cardiac Output. National Library of Medicine. 2021.
2. Yasar Sattar; Muhammad F. Hashmi. Ventricular Premature Complexes. National Library of Medicine. 2022.
3. Khashayar Farzam; John R. Richards. Premature Ventricular Contraction. National Library of Medicine. 2022.
4. Mayo Clinic. Ventricular Tachycardia. 2022.
5. Mayo Clinic. Ventricular Fibrillation. 2021.
6. Cleveland Clinic. Asystole. 2021