Junctional Rhythms
This guide explains junctional rhythms in a clear, practical way. You will learn where these rhythms originate, how to recognize them on an ECG, the main types from slower to faster rates, and what common causes and treatments look like in real clinical settings.
What are Junctional Rhythms?
Junctional rhythms occur when the heart’s electrical activity originates from the atrioventricular (AV) junction rather than the sinoatrial (SA) node. This typically happens when the SA node slows or conduction from the atria is disrupted, allowing the AV junction to take over pacing of the heart.
ACLS Certification Association videos have been peer-reviewed for medical accuracy by the ACA medical review board.
Article at a Glance
- If the junctional pacemaker assumes impulse production control, the atria and ventricles concurrently depolarize.
- P waves may occur before, after, or be buried within the QRS complex.
- When the P wave occurs before the QRS complex, the PR interval is less than 0.12 seconds.
- The junctional escape rhythm is a failsafe mechanism.
- An accelerated junctional rhythm occurs when the rate exceeds 60 beats per minute (bpm).
- Junctional tachycardia is a junctional rhythm exceeding 100 bpm.
Types of Junctional Rhythms
Junctional rhythms are classified based on heart rate, ranging from slower escape rhythms to faster tachycardias. Understanding the rate helps determine whether the rhythm is acting as a protective backup or represents abnormal automaticity.
In the lower region of the atrioventricular (AV) junction, where the AV node meets the Bundle of His, a group of pacemaker cells is responsible for junctional rhythm generation, or atrioventricular junctional rhythms.
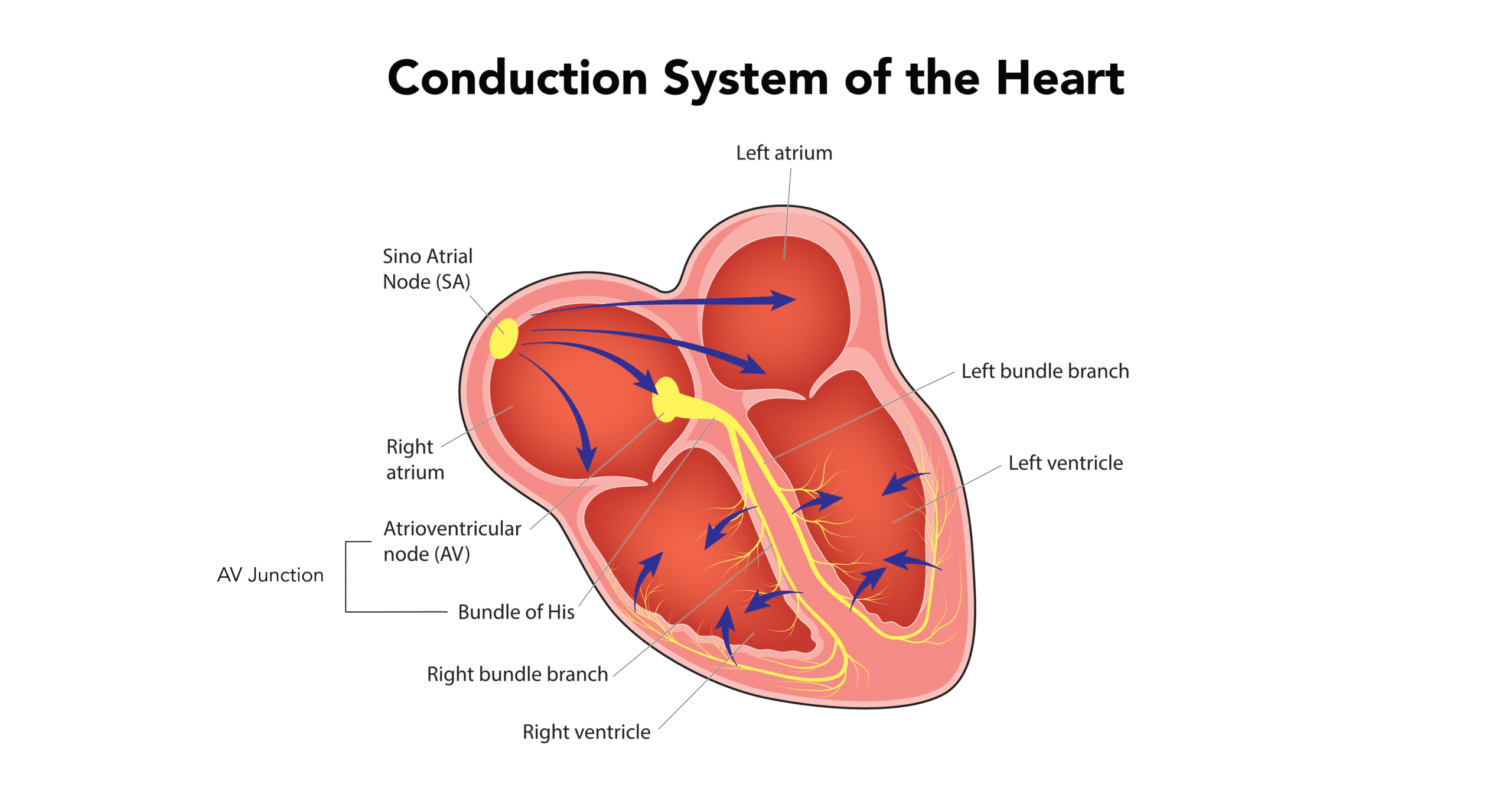
During a junctional rhythm, the heartbeat originates from the AV junction, including the AV node and Bundle of His, rather than the sinoatrial (SA) node.
In a junctional pacemaker, the impulse originates in the middle of the heart and travels in both directions.1 The atria and ventricles depolarize simultaneously, causing an unusual pattern of conduction in the ECG.
LEAD II has a positive QRS complex deflection because the impulse is directed towards the positive electrode, while the P wave shows a negative deflection as the other impulse travels away from the positive electrode.
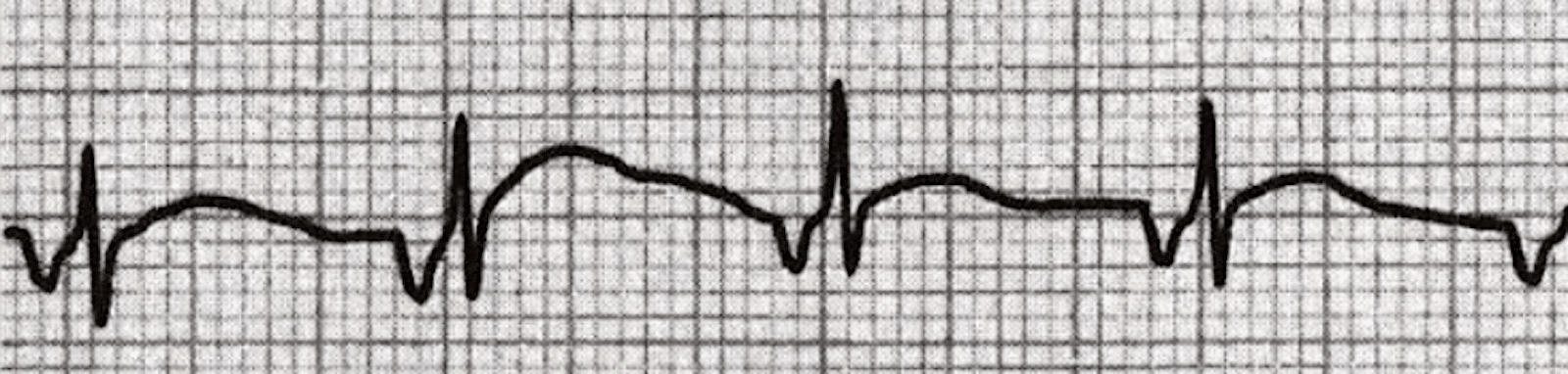
Junctional Rhythm ECG
However, the relationship of the P wave and QRS complex in junctional rhythms may not be consistent. The video below provides a visual explanation of how junctional rhythms appear on ECG and how they differ from normal sinus rhythms. The impulse force traveling towards the ventricles may be different from the force travelling towards the atria.
- RATE: 40–60 bpm; atrial and ventricular rhythms are independent
- RHYTHM: regular
- P WAVES: inverted if visible; may precede, follow, or be within the QRS complex
- PR INTERVAL: less than 0.12 seconds if preceding the QRS; may be immeasurable depending on P wave location
- QRS COMPLEX: less than 0.12 seconds; widened if BBB present
Identifying Junctional Rhythms: P Waves
Junctional arrhythmia P waves may manifest before the QRS complex, be hidden within the QRS complex, or fall after the QRS complex. The ventricles may depolarize before or after the atria.
If the ventricles depolarize before the atria, the QRS complex comes first followed by the P wave. If the ventricles and atria depolarize at the same time, the P wave is hidden within the QRS complex. If the ventricles depolarize after atrial depolarization, the P wave manifests before the QRS complex.
If an impulse results in a normal P wave and PR interval, clinicians assume the rhythm is atrial in nature, meaning the impulse originated at the sinoatrial node or elsewhere in the atria. However, if an atrial impulse occurs near the AV junction, the P waves may be inverted. An inverted P wave and a normal PR interval (0.12 to 0.20 seconds) indicate an atrial arrhythmia rather than a junctional rhythm. The PR interval in that case is normal because as the impulse traverses a normal conduction route from the atria to the ventricles.
Since the junctional pacemaker is closer to the ventricles, PR intervals of junctional rhythms are less than 0.12 seconds because the impulse travel time towards the ventricles is shorter.
The junctional pacemaker may produce a wide variety of arrhythmias, namely: premature junctional complexes, junctional escape rhythm, accelerated junctional rhythm, and junctional tachycardia.2
Common Causes of Junctional Rhythms
Junctional rhythms commonly occur when the sinoatrial node slows or fails to generate impulses, allowing the AV junction to act as a backup pacemaker. This mechanism helps maintain cardiac output but may signal an underlying issue.
Common causes include increased vagal tone, medication effects such as beta blockers, calcium channel blockers, or digoxin, myocardial ischemia, electrolyte disturbances, and post–cardiac surgery irritation. Identifying the cause is essential for determining whether the rhythm is protective or pathological.
Treatment and Management
Treatment depends on the patient’s symptoms and hemodynamic stability. Many junctional rhythms do not require direct intervention if the patient is stable and the rhythm is functioning as an appropriate backup.
Management focuses on correcting underlying causes, such as adjusting medications, treating ischemia, or correcting electrolyte imbalances. In symptomatic cases or sustained tachycardia, further evaluation and escalation of care may be necessary.
Read: Atrioventricular Blocks
Premature Junctional Complex
The premature junctional complex (PJC) is an ectopic beat, not a rhythm. An irritable focus in the AV junction stimulates a premature cardiac impulse, interrupting the core rhythm. The core rhythm is dominant, but a premature beat turns the underlying rhythmic pattern irregular.
The rhythm’s rate is determined by the core rhythm. P wave morphology is inverted secondary to the retrograde impulse coming from the junctional pacemakers. The P wave may manifest within, before, or after the QRS complex. Whenever the P wave manifests before the QRS complex, the PR-interval is less than 0.12 seconds.
The QRS complex is normal.
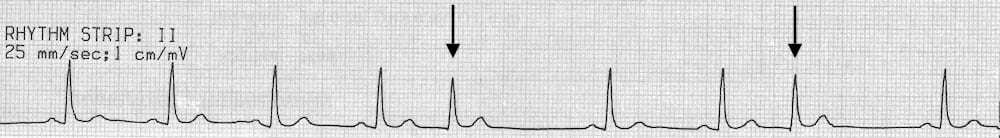
Premature junctional complexes contain P waves embedded within the QRS complex (see arrows).
Related Video – One Quick Question: What are PJCs (Premature Junctional Contractions)?
- RATE: depends on the core rhythm
- RHYTHM: depends on the core rhythm, but irregular when PJCs occur
- P WAVE: inverted P wave seen before, after, or within the QRS complex
- PR INTERVAL: measured if it is visible and seen before the QRS complex and will be less than 0.12 seconds
- QRS COMPLEX: less than 0.12 seconds
Junctional Escape Rhythm
The junctional escape rhythm is a failsafe mechanism and not truly an arrhythmia.3 If the sinoatrial node and atrial foci are irritable or unable to function, the junctional escape rhythm takes control of cardiac rate and rhythm.
It is also known as a junctional rhythm. The inherent rate at the atrioventricular junction is 40–60 bpm, so the junctional escape rhythm exhibits a rate of 40–60 bpm.
The junctional escape rhythm features regular R-R intervals. The P wave morphology is inverted, and P waves may occur within, before, or after the QRS complex. The PR interval (when the P wave occurs before the QRS complex) and the QRS complex are less than 0.12 seconds.
Related Video – One Quick Question: What are the Junctional Escape Rhythm Criteria?
- RATE: 40–60 bpm
- RHYTHM: regular
- P WAVE: inverted and may occur before, after, or be buried within the QRS complex
- PR INTERVAL: less than 0.12 seconds; only measured if the P wave occurs before the QRS complex
- QRS COMPLEX: less than 0.12 seconds
Accelerated Junctional Rhythm
Accelerated junctional rhythm occurs when the AV junction paces the heart faster than its intrinsic rate, typically between 60 and 100 bpm. It often results from increased automaticity or suppression of the sinoatrial node.
Junctional Tachycardia
When the atrioventricular junction is irritable, it overrides the sinoatrial node and other higher pacemaker sites. The inherent AV junction rate is 40–60 bpm. A rate of 60–100 bpm is an accelerated junctional rhythm. If it exceeds 100 bpm, it’s a junctional tachycardia.
- RATE: 60–100 bpm for accelerated junctional rhythm; greater than 100 bpm for junctional tachycardia
- RHYTHM: regular
- P WAVE: inverted and can manifest before, after, or be buried within the QRS complex
- PR INTERVAL: less than 0.12 seconds if it occurs before the QRS complex
- QRS COMPLEX: less than 0.12 seconds
Related Video -ECG Rhythm Review – Accelerated Junctional
Summary
Different junctional rhythms present with different metrics. Clinicians must monitor a patient’s ECG, including recognition of ectopic beats such as the premature junctional contraction, checking for heart rate, rhythm, P wave placement, PR interval occurrence, and QRS complex occurrence.
More Free Resources to Keep You at Your Best
Editorial Sources
ACLS Certification Association (ACA) uses only high-quality medical resources and peer-reviewed studies to support the facts within our articles. Explore our editorial process to learn how our content reflects clinical accuracy and the latest best practices in medicine. As an ACA Authorized Training Center, all content is reviewed for medical accuracy by the ACA Medical Review Board.
1. Yamama Hafeez; Shamai A. Grossman. Junctional Rhythm. National Library of Medicine. 2022.
2. Kenneth M. Rosen, MD. Junctional Tachycardia. American Heart Association.
3. Cleveland Clinic. Junctional Escape Rhythm. 2022.