Respiratory Assessment Guide: Techniques and Findings
Mastering the respiratory assessment is vital for identifying life-threatening conditions early. This guide covers the four pillars of assessment, such as Inspection, Palpation, Percussion, and Auscultation. We will explore how to interpret breath sounds, identify abnormal findings like crackles and wheezes, and use patient history to uncover hidden respiratory clues.
ACLS Certification Association videos have been peer-reviewed for medical accuracy by the ACA medical review board.
Article at a Glance
- The four respiratory assessment techniques are inspection, palpation, percussion, and auscultation.
- Providers should be able to distinguish between normal findings and abnormal findings.
- Clinicians will learn various respiratory assessment techniques in detail.
The Respiratory Assessment: Four Fundamental Techniques
The respiratory assessment is an important topic in critical care, and the assessment for critically ill patients greatly differs from non-critically ill patients. The four assessment techniques are: inspection, palpation, percussion, and auscultation.

A patient on a ventilator in the intensive care unit.
Patient History: Uncovering Respiratory Clues
A thorough patient history often reveals the diagnosis before you even touch the patient. Key areas to explore include:
- Smoking History: Calculate pack-years to assess risk for COPD and malignancy.
- Occupational Exposure: Ask about exposure to asbestos, silica, or chemical fumes.
- Dyspnea Triggers: Determine if shortness of breath occurs at rest, with exertion, or while lying flat (orthopnea).
Inspection
Clinicians gather a lot of data as soon as they enter the patient’s room. Their initial inspection may reveal a patient’s struggle to breathe. Clinicians must pay attention to several factors:
- Mental Status: Poor cerebral oxygenation often manifests as restlessness or agitation, whereas hypercarbia (high CO2) typically causes confusion, lethargy, or disorientation.
- Cough & Sputum: Evaluate the cough type (dry, productive, nocturnal). Assess sputum characteristics:
- Yellow/Green: Bacterial infection.
- Rust-colored: Pneumococcal pneumonia or tuberculosis.
- Pink/Frothy: Pulmonary edema, which is commonly associated with heart failure.
- Respiratory Rate & Quality: Count the rate and note the depth. Rapid, shallow breathing may indicate distress.

An inspection of the patient can alert you to their respiratory status.
- First, the provider should pay attention to the patient’s supplemental oxygen, noting the type and amount. In general, the more oxygen the patient is on, the sicker they are. Patients’ breathing may range from unassisted to requiring a ventilator.
- Providers should also count the respiratory rate and note the quality of respirations. They may be solid and full respirations, or they may be shallow and fast. Providers don’t want patients breathing too fast or too slow.
- Next, clinicians pay attention to accessory muscles to determine if the patient is using these muscle groups or intercostal muscles to encourage breathing.
- Next is anteroposterior (AP) to lateral diameter. AP is anterior to posterior while lateral is side to side. Normally, the AP to lateral diameter is 1:2. However, in certain patients, the AP to lateral diameter is 1:1. Patients with emphysema or barrel chests have an AP to lateral diameter of 1:1. Some providers call the AP to lateral diameter the chest diameter.
- Clinicians should next check the patient’s color. Check their nail beds, paying attention for any bluish hues suggesting respiratory distress or hypoxemia.
- A patient’s positioning details potential health problems. Patients may sit upright to breathe or assume a tripod position when they’re struggling to breathe. For example, a tripod position may be a sign of COPD exacerbation.
- Providers should begin talking to the patient. If they converse without running out of breath, they’re probably stable.
- Sometimes, providers may hear audible noises such as wheezing when entering the patient’s
room. That is cause for concern and should be addressed.
If inspection reveals signs of severe distress or cessation of breathing, immediate intervention is required. These steps are part of structured respiratory arrest management, which ensures timely recognition and treatment. Watch this overview of what constitutes respiratory arrest and how to identify it quickly.
Palpation is essential in critically ill patients. Providers will perform a chest excursion, placing their hands on the patient’s back with thumbs touching. Next, they’ll ask the patient to inhale deeply while looking to see if their hands expand symmetrically. If the provider’s hands don’t expand symmetrically, there’s air, fluid, or something else trapped in the patient’s lungs or pleural spaces causing asymmetrical expansion. The cause could be a pleural effusion or pneumothorax. Crepitus, also called subcutaneous emphysema, is especially important with patients who have chest tubes. For respiratory patients, the tubes drain air from a pneumothorax or drain fluid from a pleural effusion. Crepitus exhibits a “Rice Krispies” type feeling around the chest tube insertion site created by air leakage into the subcutaneous tissue. All patients with chest tubes exhibit a little crepitus around the insertion site — a byproduct of the tube’s insertion. The clinician will mark the crepitus. If it begins expanding beyond their markings, the clinician must report it. Subcutaneous emphysema may expand to a patient’s neck and face. Tactile fremitus is the vibratory sensation or feeling of chest vibrations exhibited when the patient speaks. Providers place the palms of their hands on the patient’s back, working them from top to bottom. They’ll have the patient say a phrase, feeling for a tactile fremitus as the patient speaks. The provider repeats this pattern up and down the patient’s back and front. Disorders such as pneumonia and pleural effusion will affect vibratory sensation. Pneumonia causes increased vibrations due to fluid consolidation. In pleural effusion, the fluid build-up will increase vibrations during a tactile fremitus assessment. The vibrations decrease as air enters the pleural space, occurring in injuries such as a pneumothorax. Air decreases vibrations because it isn’t a good transmitter.Palpation
Percussion, the least used assessment technique, is a method of tapping on a surface to determine the underlying structures. Clinicians put one hand on the patient’s back, using the other to tap and assess. They start between the scapula and vertebral column on both sides, tapping from the top down. Clinicians will also assess percussion from the front. Providers may find resonance and hyperresonance from a percussion assessment. Resonance is a normal finding. Providers will hear a resonant sound when tapping their fingers on a healthy lung. Hyperresonance indicates there is far too much air, a sign of a pneumothorax or air escaping the pleural space. Clinicians may also hear a tympany, a hollow, drum-like sound. It’s normal over the belly because it’s full of air, but a very tympanic sound over the lungs indicates too much air. Resonance is a normal sound, while hyperresonance and tympany are signs of air. If a provider hears dullness or flatness, fluid is present because it doesn’t produce sound during percussion. The 5-7-9 Rule: When percussing the liver borders to assess lung hyperinflation, remember the upper border of liver dullness usually falls at the: Downward displacement of these borders suggests air trapping, as seen in COPD/Emphysema. Read: Insulin Onset, Peak, and DurationPercussion
Auscultation is when providers listen to sounds, typically with a stethoscope. A clinician auscultates eight areas on the patient’s front and eight areas on the back as well as the lateral lobes. There are three auscultation zones on the right lobe and two on the left. Providers start auscultating above the clavicle, working their way down. It’s important to listen side to side to compare. A useful pattern is right, left, down, right, down, left. Clinicians listen all the way down until auscultating all areas on the front, back, and lateral lobes. Next, providers listen for normal and abnormal breath sounds. While auscultation provides immediate data, assessing gas exchange is equally critical. Review the basics of ACLS Arterial Blood Gases to understand the metabolic side of respiratory failure, and consider systemic factors such as the regular insulin peak when evaluating patients with comorbid conditions. A health care provider listens to the lungs. In cases where assessment reveals a complete lack of air movement, you must act fast. This video demonstrates how to manage respiratory arrest on an adult effectively. One abnormal breath sound is crackling, heard especially in critically ill patients. Crackles are a soft, rustling sound akin to Rice Krispies and do not clear with coughing. They suggest something is happening in the lower airway alveoli and may indicate atelectasis. Crackles may be heard in a patient with pneumonia due to infections in the lower airways. Crackles indicate problems in the alveoli. Wheezes are another abnormal breath sound, indicating airway narrowing or bronchoconstriction. Wheezing is most often associated with asthma or an asthmatic attack. Rhonchi is associated with excess phlegm buildup and cough. It’s very common. Everyone who’s ever had bronchitis has exhibited rhonchi. Stridor is an abnormal breath sound characterized by a high-pitched whistling due to disrupted airflow. Stridor is a warning sign of imminent airway closure. Stridor may present in an extubated patient taken off a ventilator. If heard, the provider should immediately re-intubate. Providers may also hear stridor in children with croup as they breathe in. While not as severe as other cases, clinicians should administer the child steroids or anti-inflammatories to open their airways. A rub (also known as a pleural friction rub) is an abnormal lung sound caused by an inflammation of the pleural layers “grating” against each other. An infection is usually to blame, and a pleural friction rub is a likely indicator of pleurisy, especially when accompanied by other signs of infection. Providers should practice the four respiratory assessment techniques, inspection, palpation, percussion, and auscultation. Patients will exhibit a variety of normal and abnormal breathing sounds, and providers should diagnose and provide treatment accordingly. Documenting Abnormal Sounds: When an adventitious sound is heard, documentation must be specific. Note the:Auscultation
Normal Breath Sounds

Abnormal Breath Sounds
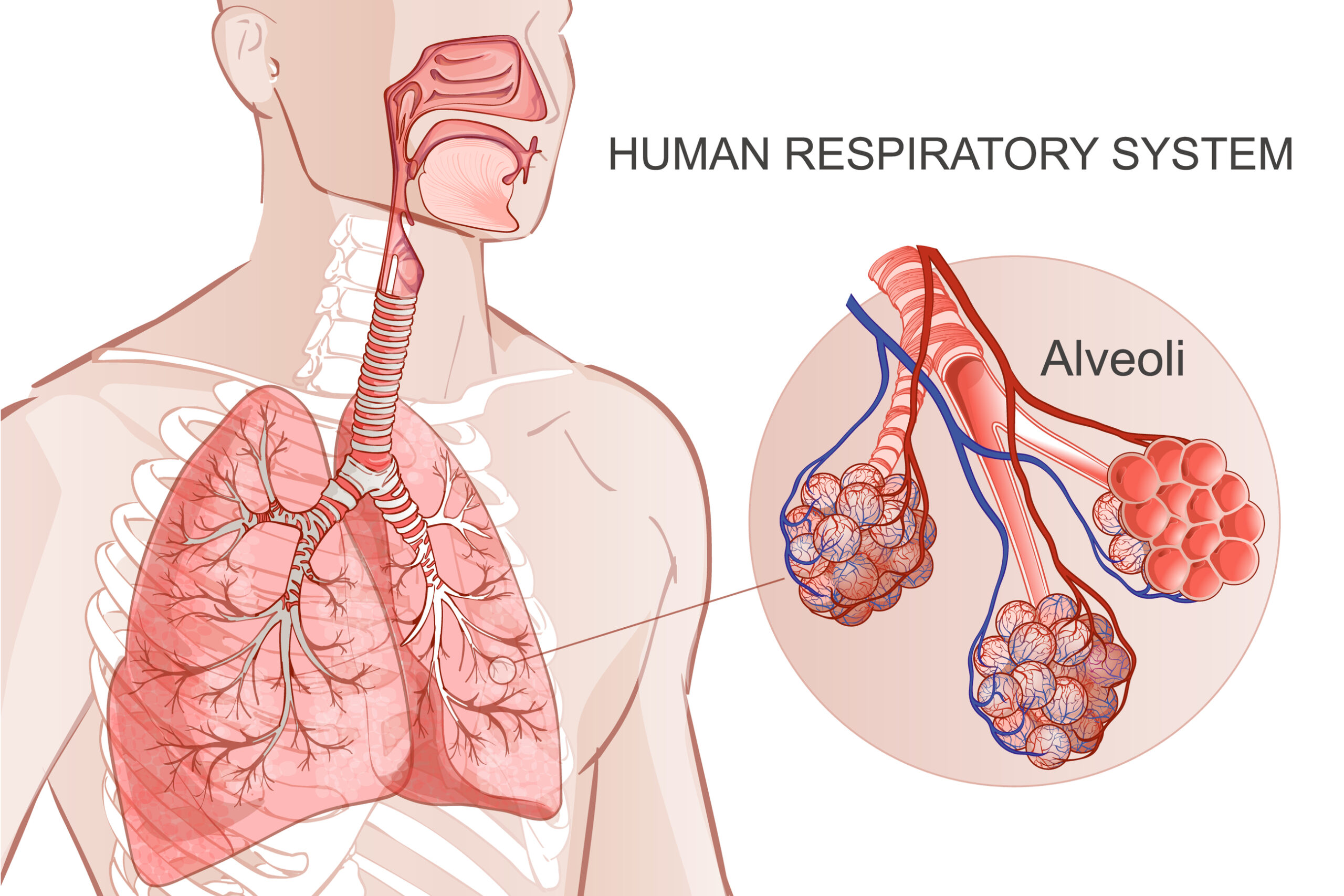
A comprehensive respiratory assessment relies on the synergy of history taking, inspection, palpation, percussion, and auscultation. By systematically evaluating breath sounds, sputum characteristics, and physical signs of distress, clinicians can accurately diagnose various respiratory conditions ranging from pneumonia to pneumothorax. Mastery of these techniques ensures timely intervention and better patient outcomes.Summary
More Free Resources to Keep You at Your Best
Editorial Note
ACLS Certification Association (ACA) uses only high-quality medical resources and peer-reviewed studies to support the facts within our articles. Explore our editorial process to learn how our content reflects clinical accuracy and the latest best practices in medicine. As an ACA Authorized Training Center, all content is reviewed for medical accuracy by the ACA Medical Review Board.