What is Synchronized Cardioversion?
This guide is designed for healthcare professionals, ACLS providers, and medical students seeking a clear understanding of electrical therapy in tachyarrhythmias. By the end of this article, you will be able to confidently set up a cardiac monitor for synchronized cardioversion, administer the shock safely, and understand when to cardiovert versus when to defibrillate.
ACLS Certification Association videos have been peer-reviewed for medical accuracy by the ACA medical review board.
Article at a Glance
- Workflow: Secure the airway, apply pads, enable the SYNC feature, select the appropriate energy level, clear the patient, and administer the shock.
- Monitor Cues: Always verify that the SYNC indicator is illuminated and that R-wave markers (hash marks) are correctly tracking each QRS complex.
- Risk Mitigation: Synchronization delays energy delivery to align with the R wave, preventing an accidental “R-on-T” shock during the vulnerable portion of the T wave, which could precipitate ventricular fibrillation.
Synchronized Cardioversion
Synchronized cardioversion is a specialized electrical therapy where a shock is timed (synchronized) to align exactly with the peak of the QRS complex (the R wave) on the patient’s ECG. We use synchronized cardioversion for hemodynamically unstable tachycardias with a pulse still present. Common indications include unstable Atrial Fibrillation (AF), Atrial Flutter, Supraventricular Tachycardia (SVT), and Ventricular Tachycardia (VT) with a pulse.
Pulse vs. Pulseless Clarification: It is crucial to distinguish between a patient who needs synchronized cardioversion and one who needs CPR and defibrillation. For example: If SVT is present with a pulse but poor perfusion, do I cardiovert or start CPR? Because the patient still has a pulse (even if perfusion is poor), you should perform immediate synchronized cardioversion. CPR and defibrillation are reserved exclusively for cardiac arrest (pulseless) scenarios.
To better understand the decision-making process, watch our video on assessing the clinical condition in tachycardia. Furthermore, for a deep dive into recognizing instability, review the concepts in our lesson covering the unstable patient. As providers, it’s our responsibility to know the equipment, so make sure you review your monitor and know how to perform these procedures safely.
Monitor Setup
Most monitors generally operate the same. Follow these standard steps to prepare the monitor:
- Turn on the Monitor/Defibrillator: Attach the pads securely to the patient’s chest.
- Select the SYNC Feature: Press the “sync” button. This puts the monitor into a synchronized state.
- Verify R-Wave Markers: Look for hash marks or dots appearing exactly above each QRS complex, confirming the machine is tracking the rhythm accurately.
- Select Energy Level: Follow specific device manufacturer guidelines and local protocols. Energy levels depend on the rhythm (e.g., narrow regular rhythms often require 50–100 Joules, while wide or irregular rhythms may require higher energy). Be prepared to escalate the energy level in a stepwise fashion if the initial shock is unsuccessful.

Pressing the SYNC button ensures the device tracks the R waves before delivering energy.
Troubleshooting the SYNC Feature: If the monitor is not sensing the QRS complexes or the markers are inconsistent, adjust the ECG size (gain) or select a different lead until the markers clearly align with every R wave.
The fundamental goal of synchronization is to avoid delivering an electrical shock during the vulnerable portion of the T wave (the relative refractory period). If a shock lands on this vulnerable phase, it can trigger an “R-on-T” phenomenon, which carries a high risk of precipitating lethal ventricular fibrillation (VF). For a quick refresher on these phases, watch this breakdown of ECG and the Cardiac Cycle Basics.
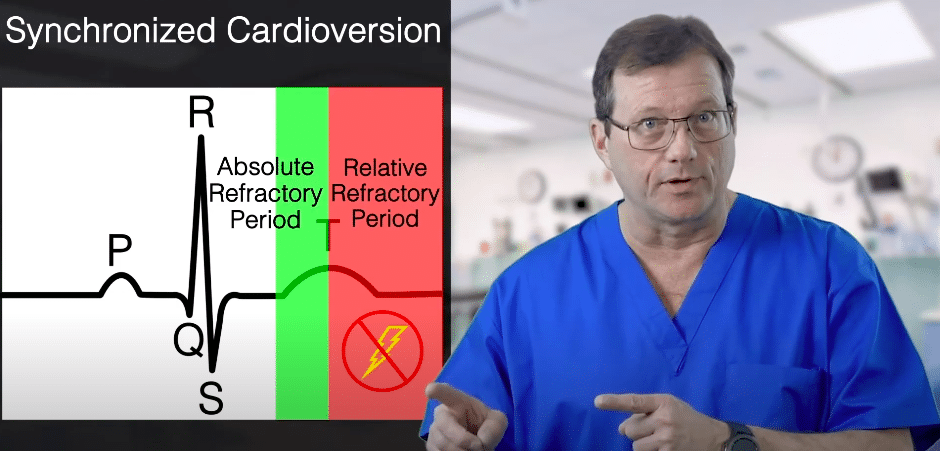
Synchronization avoids the vulnerable portion of the T wave to prevent an R-on-T phenomenon.

Verify that the SYNC markers (hash marks) align perfectly with the peak of the QRS complexes.
Read: Assessing Appropriateness for Clinical Condition
Shock Administration
Before delivering the shock, consider patient comfort. Because synchronized cardioversion is painful and the patient is awake, provide conscious sedation and analgesia whenever feasible, ensuring your airway equipment is ready at the bedside.
Follow this checklist for safe shock administration:
- Charge the Monitor: Press the charge button once the energy is selected.
- Clear the Patient: Visually confirm that oxygen is moved away and no team members are touching the patient or the bed. State “Clear!” loudly.
- Press and Hold the Shock Button: Because the machine must wait for the exact moment of the next R wave, there will be a slight delay. Caution: Behavior varies by manufacturer—some modern units auto-fire quickly, while others require you to press and firmly hold the button until the shock is delivered.
- Reassess the Rhythm: Immediately look at the monitor to determine if the rhythm has converted and check for a pulse.
Common Pitfall: Most monitors automatically default back to unsynchronized mode (defibrillation) immediately after a shock is delivered. If the first shock fails and you need to deliver a second cardioversion, you must press the SYNC button again.

Always visually confirm the patient is clear before pressing the shock button.
What is the difference between cardioversion and defibrillation?
While both procedures deliver electrical energy to the heart to terminate an arrhythmia, their timing and indications are fundamentally different.
| Feature | Synchronized Cardioversion | Defibrillation |
|---|---|---|
| Timing | Synced exactly to the R-wave | Delivered immediately (unsynced) |
| Typical Indication | Unstable tachycardia with a pulse | Cardiac arrest (Pulseless VT or VF) |
| Energy Level | Lower initial energy (e.g., 50–100J) | Higher initial energy (e.g., 120–200J) |
Synchronized vs Unsynchronized Cardioversion
“Unsynchronized cardioversion” is practically synonymous with defibrillation—it means delivering the shock without waiting for the SYNC markers. Decision Note: If a patient is unstable but the monitor cannot reliably synchronize to the R waves (for example, in polymorphic VT), do not delay therapy. Treat the rhythm as ventricular fibrillation and perform high-energy, unsynchronized cardioversion (defibrillation).
Summary
Synchronized cardioversion is the definitive treatment for hemodynamically unstable tachyarrhythmias in patients with a pulse. Remember these core steps:
- Prepare: Consider sedation, attach pads, and press the SYNC button.
- Verify: Ensure R-wave markers are tracking correctly to avoid an R-on-T event.
- Deliver: Select the protocol-driven energy dose, clear the patient, and press (and hold if necessary) the shock button.
- Reassess: Check the rhythm and remember to re-enable SYNC if a subsequent shock is required.
More Free Resources to Keep You at Your Best
Editorial Note
ACLS Certification Association (ACA) uses only high-quality medical resources and peer-reviewed studies to support the facts within our articles. Explore our editorial process to learn how our content reflects clinical accuracy and the latest best practices in medicine. As an ACA Authorized Training Center, all content is reviewed for medical accuracy by the ACA Medical Review Board.