How to Do A Neurological Assessment: A 5-Step Neuro Exam (LOC, GCS, Pupils, EOMs, Strength)
This guide walks you through how to properly perform and document a rapid, focused bedside neurological assessment. Designed for nurses, ACLS providers, and medical students, this article will teach you the exact 5-step sequence required to establish a patient’s baseline and rapidly identify acute neurological changes.
ACLS Certification Association videos have been peer-reviewed for medical accuracy by the ACA medical review board.
Article at a Glance
The 5-Step Neuro Check Order: A standard focused bedside neurological assessment evaluates five core areas:
- Level of Consciousness (LOC): How awake and arousable is the patient?
- Glasgow Coma Scale (GCS): Quantifying eye, verbal, and motor responses out of 15.
- Pupils (PERRLA): Evaluating cranial nerves II and III for size and reactivity.
- Extraocular Movements (EOMs): Checking the six cardinal fields of gaze for tracking and nystagmus.
- Grips and Strength: Checking bilateral extremities for equal motor function.
What is a neurological assessment and why is it done?
A neurological assessment is a clinical evaluation of the nervous system. It is important to distinguish between a comprehensive neurological exam (a lengthy, specialized workup done by a neurologist) and a focused bedside neurological assessment (a rapid “neuro check” performed frequently by nurses and emergency providers).
Providers perform these rapid, focused checks to establish a baseline, screen for sudden changes, monitor the progression of a known injury, or rapidly evaluate a patient post-trauma or during a suspected stroke.
What does the assessment entail?
When performing a routine neuro check, five topics must be addressed and documented sequentially:
- Level of consciousness (LOC)
- Glasgow Coma Scale (GCS)
- Pupils (Cranial nerves II and III)
- Extraocular movement (Cranial nerves III, IV, and VI)
- Grips and leg strength (Spinal motor pathways)
“Patient is awake, alert, and oriented x4. GCS 15. Pupils are 3mm, round, equal, and reactive to light and accommodation (PERRLA). EOMs intact without nystagmus. Hand grips and plantar/dorsiflexion are 5/5 and bilaterally equal.”
How is a neurological assessment performed?
To ensure nothing is missed and that subsequent providers can accurately compare your findings, always perform the assessment in a systematic, top-to-bottom order.
1. Level of Consciousness (LOC)
The level of consciousness is the most sensitive and basic indicator of how the patient is doing neurologically. It evaluates how awake and arousable the patient is. Implementation Guidance: Always start by observing the patient before touching them. If their eyes are closed, speak their name. If they do not respond to voice, gently shake their shoulder or apply a standard painful stimulus (like a sternal rub or pinching the nail bed). Document exactly what level of stimulus was required to arouse them.
At the very top of the scale, a patient is awake and alert.
The next level down is a lethargic patient. This patient falls asleep easily, perhaps even when the rescuer is talking to them. But they’re still easily aroused by voice.
The next level of consciousness is obtunded. These patients fall asleep very easily and are difficult to arouse. Unlike a lethargic patient, a rescuer may have to shake them lightly to wake them. When woken they will talk in sentences. They are easily understood but difficult to keep awake.
Following obtunded is stuporous. Patients are classified as this level when they are barely above comatose. A stuporous patient is very difficult to arouse and requires painful stimuli. If a clinician does arouse them, they may express themselves in grunts and groans. They will be nonsensical, won’t form words, and will not be able to answer questions.
The very last level of consciousness is comatose. These patients do not wake up, even with painful stimuli.
Keep in mind that level of consciousness should not be confused with mental status. Mental status measures something else entirely (orientation). In trauma cases, clinicians must also differentiate conditions such as spinal shock vs neurogenic shock, which can complicate neurological findings.
| Level of Consciousness | Patient Description |
|---|---|
| Awake and alert | Awake, alert. Speaks appropriately |
| Lethargic | Falls asleep easily. Easily aroused. Speaks appropriately |
| Obtunded | Falls asleep easily. Difficult to arouse. Speaks appropriately |
| Stuporous | Very difficult to arouse. Unable to form words |
| Comatose | Not able to be aroused. Unconscious |
Stuporous refers to a patient who is difficult to arouse and unable to form words.
2. Glasgow Coma Scale (GCS)
The Glasgow coma scale (GCS) is a neurological scale for objectively evaluating a person’s level of consciousness and mental status. This scale is commonly used following a possible traumatic brain injury or stroke.

The Glasgow Coma Scale assesses a person’s level of consciousness.
The Glasgow coma scale ranges from 3 to 15. The lowest possible score is a 3, which indicates deep coma. The highest score is a 15, indicating a fully awake and oriented patient. The GCS evaluates three specific areas:
When documenting, note if factors like an endotracheal tube (which prevents speech, charted as 1T) or heavy sedation are confounding the score, as these prevent an accurate baseline neurological assessment.
Eye Opening Response (Max 4 Points)
If the clinician enters the room and the patient’s eyes open spontaneously, they get full points (4). If they must speak to the patient to wake them up, they get 3. If the clinician needs to inflict noxious stimuli (pain) to encourage them to open their eyes, they get a 2. If they don’t open their eyes at all, only 1 point is awarded.
Verbal Response (Max 5 Points)
Verbal response determines the patient’s orientation (mental status). Note: A patient can be entirely awake (LOC) but still confused (Mental Status). If they are oriented to person, place, time, and situation, they receive 5 points. If they’re awake but confused, they get 4 points. If they speak in sentences but the words don’t make sense contextually, they receive 3 points. If the only sounds they emit are incomprehensible moans, they receive 2 points. If there is no verbal response, they get 1 point.
Motor Response (Max 6 Points)
The motor score decreases as the patient’s responses become less purposeful. A patient who successfully obeys a command (e.g., “squeeze my hands” and “let go”) receives full points (6). If they do not obey commands, the clinician applies a pain stimulus:
- Localizing Pain (5 points): The patient purposefully reaches over to brush the clinician’s hand away from the pain source.
- Withdrawal From Pain (4 points): The patient pulls away or turns in the bed, but cannot purposefully locate the source.
- Decorticate Posturing (3 points): Abnormal flexion. The patient draws their arms stiffly into their core.
- Decerebrate Posturing (2 points): Abnormal extension. The patient hyperextends their arms out and hyperpronates their wrists outward. This indicates severe brainstem injury and is neurologically more worrisome than decorticate posturing.
- No Response (1 point): No movement to noxious stimuli.
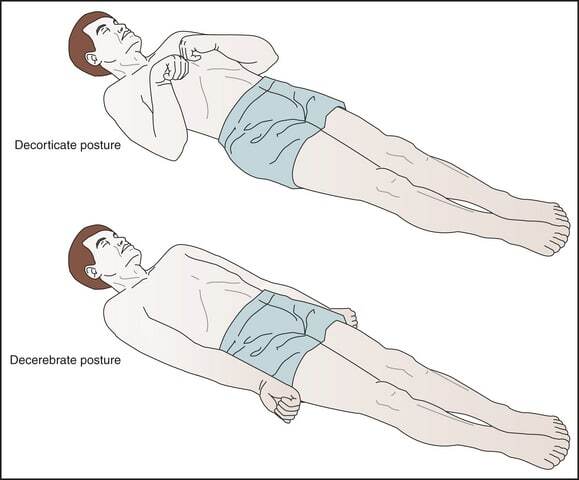
Decorticate and decerebrate posturing indicate severe neurological damage.
3. Pupils
Clinicians need to check the pupils during the physical assessment to evaluate cranial nerves II and III. Cranial nerve II (optic) controls visual acuity/afferent input, while Cranial nerve III (oculomotor) controls pupil constriction and dilation. The PERRLA test is used to examine the pupils:
- Pupils
- Equal
- Round
- Reactive to
- Light
- Accommodation
Normal vs. Abnormal Quick Check:
- Normal: Equal in size bilaterally (typically 2-3 mm) and briskly reactive (constricting) to light.
- Abnormal: Unequal (one dilated, one constricted), sluggish, or completely “fixed/blown” (nonreactive). Extremely pinpoint (1mm) or widely dilated pupils often indicate drug toxicity or severe pressure on CN III.
To test light reactivity, shine a penlight into the patient’s eyes from the side while they look straight ahead at your nose. You are looking for a brisk, bilateral constriction. Next, test accommodation by having the patient focus on a pen held close to their face, then shifting focus to a distant object like a clock. The pupils should dilate as their eyes accommodate to the distance.
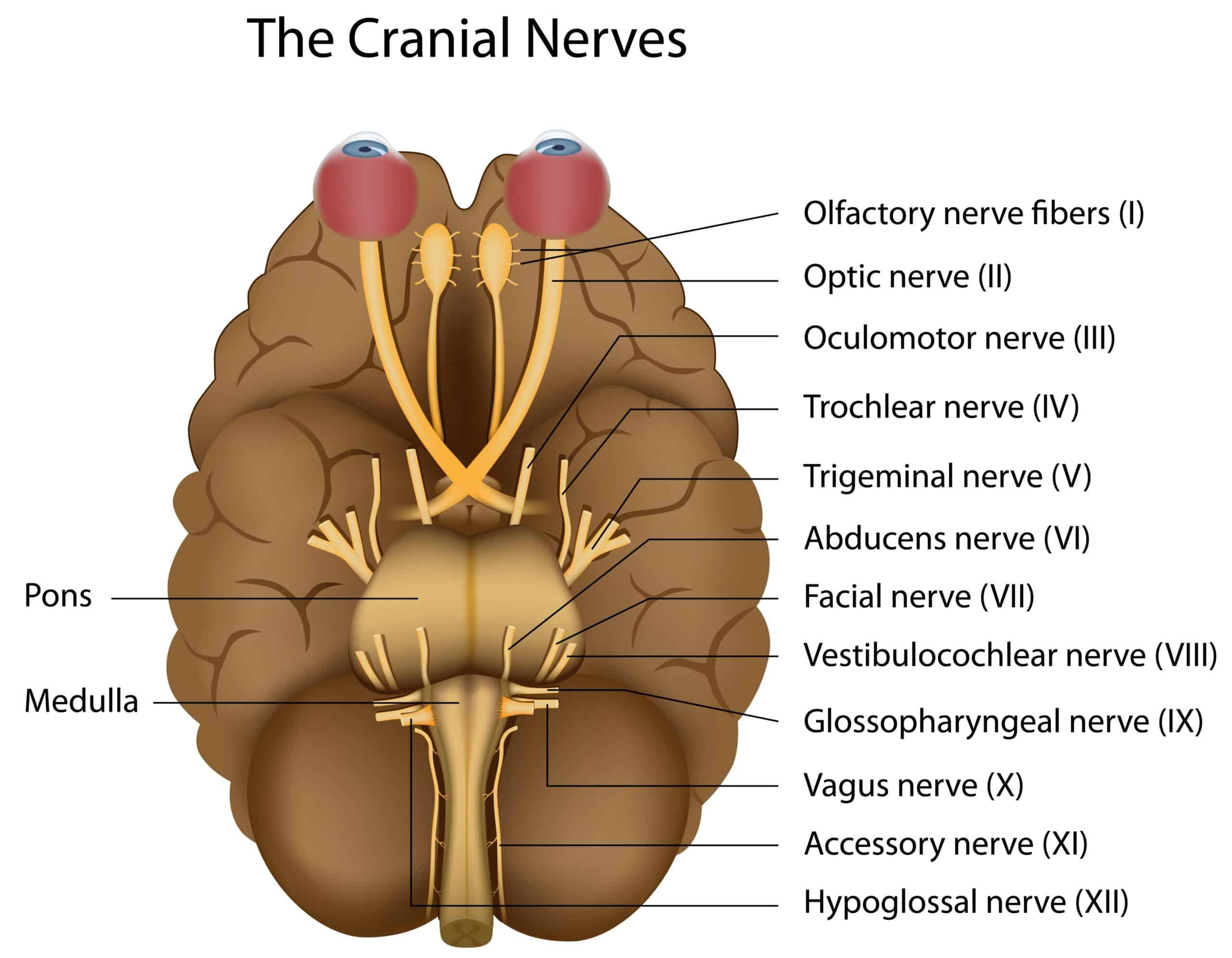
The cranial nerves connect the brain to the head, neck, and body.
4. Extraocular Movements (EOMs)
Extraocular movements (EOMs) evaluate cranial nerves III, IV, and VI, and are assessed using the six cardinal fields of gaze.
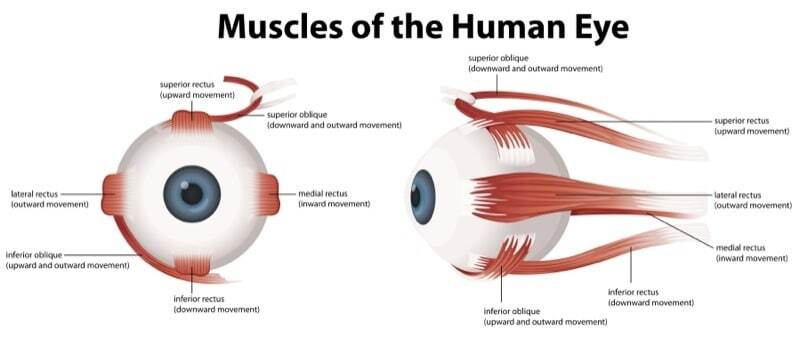
The six cardinal fields of gaze confirm extraocular movement.
Have the patient keep their head still and follow your pen with only their eyes through these six patterns:
- Superior rectus (upward movement)
- Superior oblique (downward and outward movement)
- Lateral rectus (outward movement)
- Medial rectus (inward movement)
- Inferior oblique (upward and outward movement)
- Inferior rectus (downward movement)
If the patient can follow the pen smoothly in all directions without nystagmus (involuntary eye shaking), the clinician will chart that “EOMs are intact.”
However, if the patient’s eyes jump or wiggle, nystagmus is present and must be documented. Furthermore, if the patient physically cannot move their eye into one of the quadrants (indicating a nerve palsy or entrapment), you must document exactly which gaze field failed.
5. Grips and Strength
Finally, the clinician checks peripheral motor function by testing grips and extremity strength. To test upper extremities, have the patient squeeze two of your fingers simultaneously in both hands. The exact baseline strength (e.g., a strong young adult vs. a frail elderly patient) matters less than bilateral equality. It’s vital that the grips are equal in both hands.
Testing leg strength is similar. Have the patient push down against your hands with their feet (like pressing a gas pedal) and pull their toes up against resistance. Again, assess for equality. If the patient is generally weak in all extremities, it may be a systemic or muscular issue. However, acute unilateral weakness (where one arm or leg is noticeably weaker than the other) is a hallmark indicator of a focal neurological emergency, such as a stroke.
Caution on Trending: The true value of a focused neurological assessment lies in repeating it. You must trend the patient’s strength against their baseline. A patient who initially had 5/5 equal grips but drops to 3/5 in the right hand an hour later is experiencing an active, evolving neurological event.
Conclusion
This has been a quick overview of the neurological assessment. The clinician will utilize this information every time they assess a patient. During a focused assessment, such as after a stroke or other neurological incident, clinicians may perform the neurological assessment more often.
More Free Resources to Keep You at Your Best
Editorial Note
ACLS Certification Association (ACA) uses only high-quality medical resources and peer-reviewed studies to support the facts within our articles. Explore our editorial process to learn how our content reflects clinical accuracy and the latest best practices in medicine. As an ACA Authorized Training Center, all content is reviewed for medical accuracy by the ACA Medical Review Board.