Intravenous (IV) Fluids: Types, Uses, and Administration
Intravenous (IV) fluids are essential in clinical settings for maintaining hydration, correcting electrolyte imbalances, and administering medications. This guide covers the critical differences between crystalloids and colloids, detailed profiles of isotonic, hypertonic, and hypotonic fluids, and essential administration protocols.
ACLS Certification Association videos have been peer-reviewed for medical accuracy by the ACA medical review board.
Article at a Glance
- Isotonic Fluids (e.g., 0.9% NaCl, Lactated Ringer’s): Have a solute concentration equal to blood. They remain in the intravascular space to increase volume, making them ideal for treating hypovolemia, hemorrhage, and septic shock.
- Hypertonic Fluids (e.g., 3% NaCl): Have a higher concentration than blood. They pull fluid from cells into the intravascular space, commonly used for severe hyponatremia and reducing cerebral edema in head injuries.
- Hypotonic Fluids (e.g., 0.45% NaCl, D5W): Have a lower concentration than blood. They cause fluid to shift out of the vessels and into the cells, effective for treating diabetic ketoacidosis (DKA) and hypernatremia.
Different Uses of Intravenous Fluids
IV fluids are a cornerstone of patient care, essential for maintaining hemodynamic stability and correcting fluid and electrolyte disturbances. Whether treating a marathon runner with dehydration or a trauma patient with blood loss, selecting the correct fluid based on tonicity is vital.
Crystalloids vs. Colloids: An Overview
Before selecting a specific fluid, it is important to distinguish between the two main categories:
- Crystalloids: These solutions contain small molecules (like electrolytes and glucose) that can easily flow across semipermeable membranes from the bloodstream into the cells and tissues. Examples include Normal Saline and Lactated Ringers. They are the primary choice for fluid resuscitation and maintenance.
- Colloids: These solutions contain larger molecules (such as proteins or starch) that cannot easily pass through cell membranes. They remain in the intravascular space longer, drawing fluid into the vessels via oncotic pressure. They are often used for volume expansion in specific shock states.
The outline for this lesson includes:
- Isotonic fluids
- Hypertonic fluids
- Hypotonic fluids
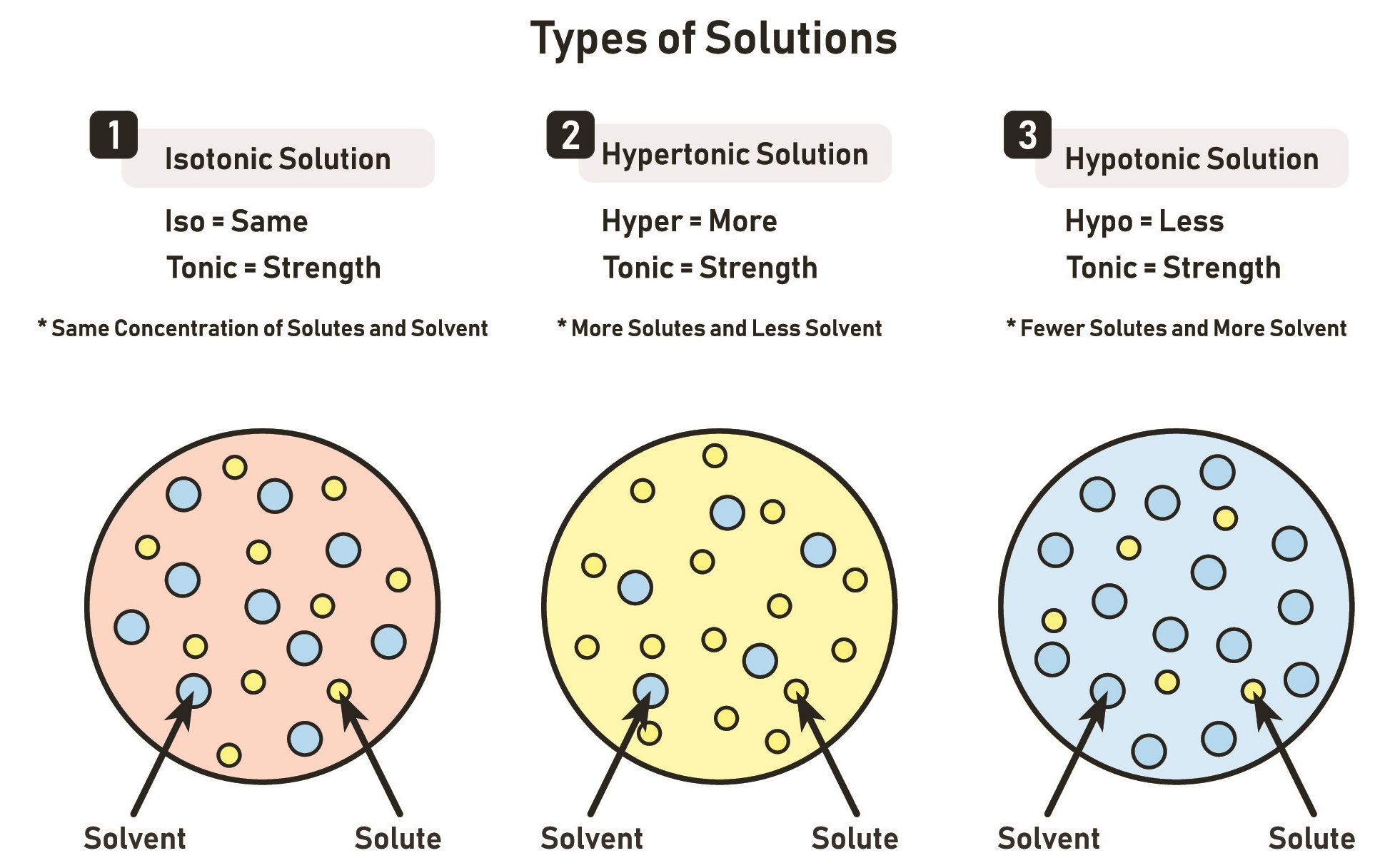
Different types of fluids have different effects on the body.
Isotonic Fluids
Isotonic fluids are the most common IV fluids used in hospitals and other settings.
Isotonic fluids are most often used in emergency situations requiring the rapid replacement of fluid losses. Clinical scenarios include:
- Hypovolemia: Used for dehydration caused by severe vomiting or diarrhea to restore intravascular volume without shifting fluid into or out of cells.
- Septic Shock: Large volumes of isotonic fluids are administered to maintain blood pressure and organ perfusion.
- Hemorrhage: 0.9% Saline or Lactated Ringers are used as first-line therapy for trauma patients losing blood volume.
Examples are:
- 0.9% sodium chloride
- Lactated Ringer solution

0.9% sodium chloride (normal saline) is an isotonic fluid.
The prefix “iso” means equal. The concentration of solutes in isotonic fluids is equivalent to that normally found in the serum.
The key concept is to think of 0.9% as the baseline concentration for solutes in IV fluids. Isotonic fluids have a solute percentage of 0.9%. Any concentration greater than 0.9% is considered hypertonic, and any below 0.9% is considered hypotonic. This 0.9% rule works for every IV fluid except for 5% dextrose (D5W). D5W will be discussed further in the hypotonic fluids section.
Isotonic fluid is used to replace intravascular losses because it stays within the intravascular space (space within the blood vessels).
Isotonic fluids are most often used in emergency situations requiring the rapid replacement of fluid losses. Examples of this would be:
- Hypovolemia
- Septic shock
- Hemorrhage
Lactated Ringer is a type of isotonic fluid used frequently in postoperative patients to replete blood that was lost during surgery. This IV fluid is formulated with electrolytes that are similar to those found in the blood.
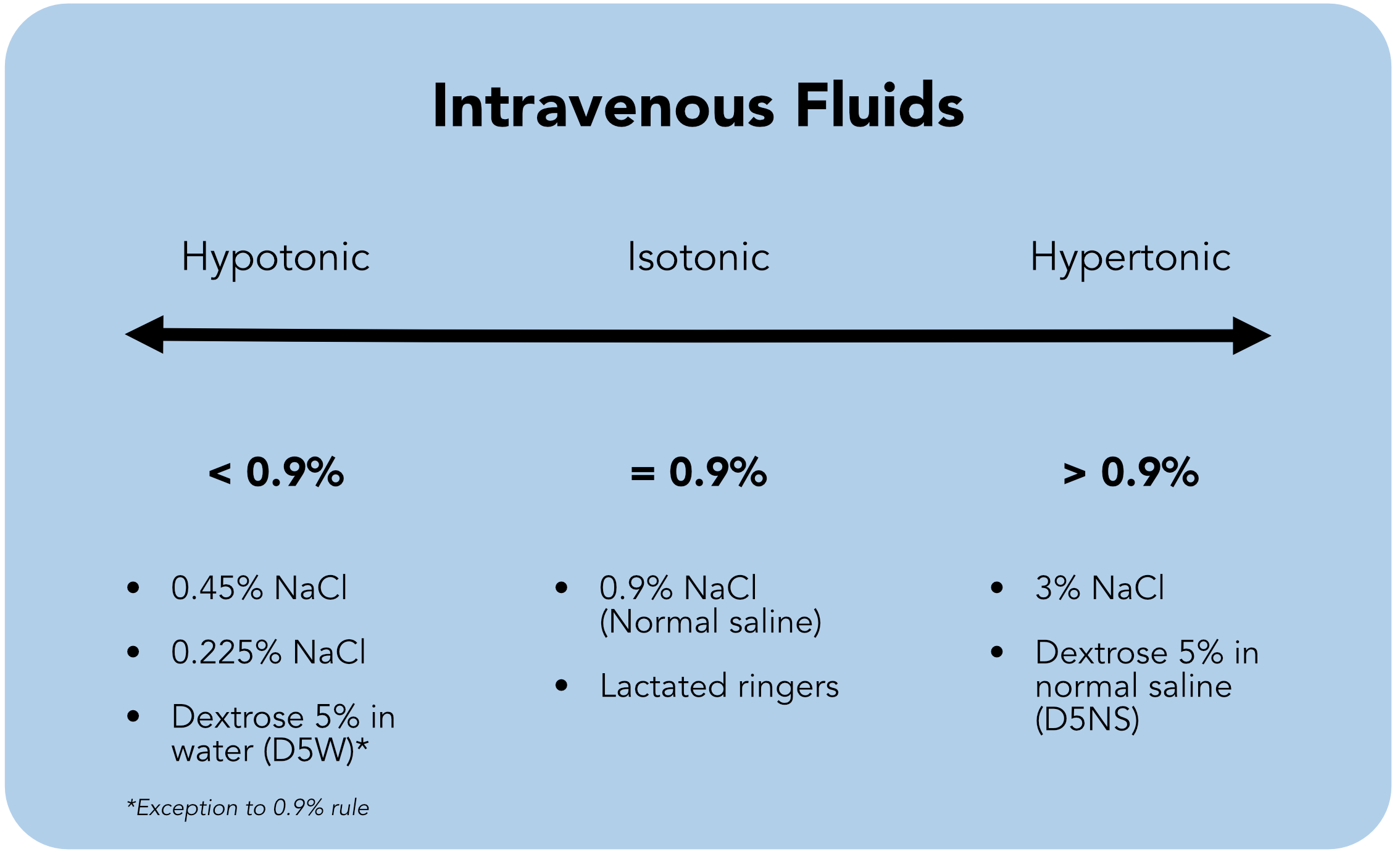
Intravenous fluids are isotonic, hypotonic, or hypertonic.
Read: Diabetic Ketoacidosis: Fact and Fiction
Hypertonic Fluids
Hypertonic fluids have a solute percentage greater than that found in the serum, or more than 0.9%.
Examples are
- 3% sodium chloride (NaCl)
- Dextrose 5% with normal saline (D5NS)
When hypertonic fluid is administered to a patient, it makes their serum more concentrated and increases the osmolality. And where does the fluid go? The fluid will travel from places of lower concentration to places of higher concentration. This means that fluid from the cells will travel into the intravascular space. Basically, hypertonic fluid gives the serum a “pulling power.”
Hypertonic fluids are used for:
- Head injury. When patients have a head injury, the main concern is cerebral edema, which is swollen brain cells. Giving hypertonic fluids will help pull fluid out of the brain cells and reduce swelling caused by the injury.
- Hyponatremia. Hypertonic fluids are used to correct severe hyponatremia. 3% sodium chloride is commonly used.
- Hypoglycemia. Hypertonic fluids such as dextrose 50% (D50W) are given to correct severe hypoglycemia or low blood glucose.
When a patient receives a hypertonic fluid, they are at risk for intravascular fluid volume overload and may develop complications. The nurse will be measuring daily weights, recording inputs and outputs, and listening to the lungs. The nurse will also be checking the blood pressure and assessing for edema. Typically, edema will not be visible until the patient has gained an excess of 3 liters of fluid.
Critical Contraindications: Hypotonic fluids should never be given to patients with increased intracranial pressure (ICP), head trauma, or stroke. Because these fluids cause fluid to shift into cells, they exacerbate cerebral edema (brain swelling), which can be fatal. Additionally, rapid administration can cause cardiovascular collapse as fluid leaves the blood vessels, leading to hypotension.
Risks and Monitoring for Hypertonic Fluids
Hypertonic fluids are high-risk medications. Because they pull fluid from the intracellular space into the vascular space, they can cause cells to shrink (cellular dehydration).
- Fluid Overload: Rapid expansion of blood volume can lead to pulmonary edema and heart failure. Monitor lung sounds and effort of breathing closely.
- Vessel Irritation: These fluids can be irritating to veins (phlebitis) and are often best administered through a central line.
Related Video – One Quick Question: How Do You Calculate IV Drip Rates?
Hypotonic Fluids
The solute concentration of hypotonic fluids is less than that found in the serum, or less than 0.9%. Administration of hypotonic fluids makes the intravascular space more dilute.
Where does the fluid travel? Fluid will travel from places of low concentration to areas of high concentration. Therefore, the fluid is going to travel out of the intravascular space into the cells.
Examples of hypotonic fluids are:
- 0.45% sodium chloride (also called half-normal saline)
- 0.225% sodium chloride
- Dextrose 5% in water
Dextrose 5% in water (D5W) is an exception to the 0.9% rule. Although 5% is greater than 0.9% and may seem hypertonic, D5W is actually hypotonic. D5W is dextrose 5% that is diluted in water. It is initially isotonic in the bag, but the dextrose is metabolized when administered, leaving water that then dilutes out into the serum and expands the extracellular space. Therefore, D5W is considered a hypotonic fluid.
Hypotonic fluids are used in cases of:
- Extreme hypernatremia. Hypotonic fluids help dilute the sodium level but must be given slowly so as not to bring the serum sodium down too rapidly and cause adverse effects.
- Diabetic ketoacidosis (DKA). Initially, a patient with DKA will receive normal saline to replace volume losses. Then, they will receive half-normal saline. After that, they will receive D5W to prevent a sudden drop in glucose levels when their numbers start coming down.
- Heart failure. Hypertonic fluids should not be given to patients with heart failure because that can put them at risk for intravascular volume overload.
A very important note about hypotonic fluids is that they should never be given to patients with potential or actual head injuries. This includes stroke patients because a common symptom is cerebral edema. Giving these patients hypotonic fluids could make the cerebral edema worse.
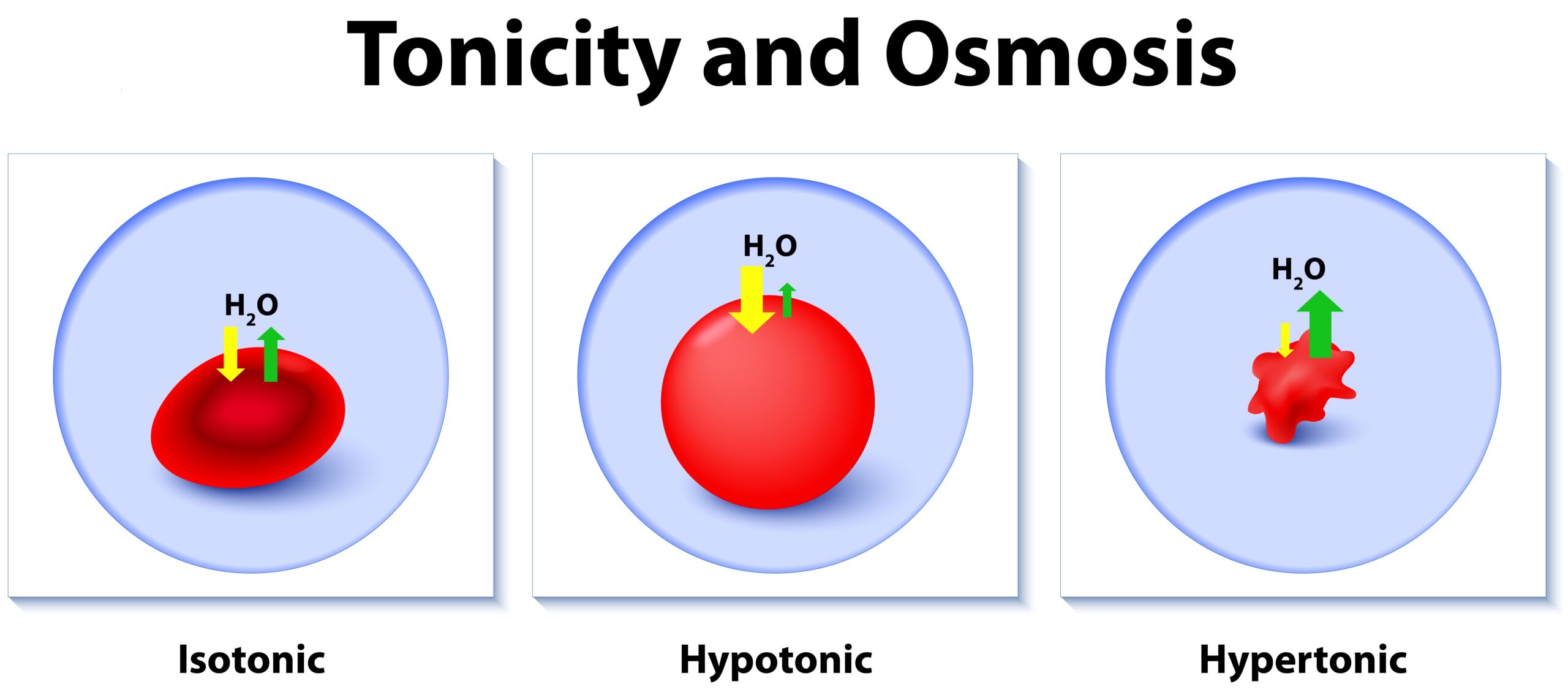
Hypotonic fluids cause cells to swell, while hypertonic fluids pull fluid out from the cells.
Monitoring, Evaluation, and Complications of IV Fluid Therapy
Continuous reassessment is required to ensure the therapy is effective without causing harm.
Fluid Balance Monitoring and Diagnostic Evaluation Methods
Nurses and providers must monitor for signs of efficacy (improved pulse, blood pressure, and urine output) versus signs of complications.
- Physical Assessment: Check for jugular venous distention (JVD), bounding pulses, crackles in the lungs, and peripheral edema, which indicate fluid overload.
- Lab Studies: Monitor electrolytes (Na+, K+), BUN/Creatinine, and Hematocrit. Hemodilution (low hematocrit) may indicate over-hydration.
- Imaging: Chest X-rays can reveal pulmonary congestion, while bedside ultrasound can assess Inferior Vena Cava (IVC) diameter to estimate fluid status.
IV Fluid Management Strategies and Clinical Considerations
Modern fluid management often employs a “Restrictive vs. Liberal” approach depending on the clinical context. For example, in ARDS (Acute Respiratory Distress Syndrome), a conservative fluid strategy is often preferred to prevent lung edema. Conversely, in early sepsis, aggressive fluid resuscitation (e.g., 30mL/kg) is the standard of care. Always tailor the fluid choice and rate to the individual patient’s comorbidities, such as heart failure or renal insufficiency.
Summary Table
Below is a summary table of IV fluids and uses.
| Type of fluid | Examples | Uses |
|---|---|---|
| Isotonic fluid |
|
|
| Hypotonic fluid |
|
|
| Hypertonic fluid |
|
|
What are Intravenous (IV) Fluids?
Intravenous (IV) fluids are specially formulated liquids injected directly into a vein to prevent or treat dehydration. They are used in patients of all ages who are sick, injured, dehydrated from exercise or heat, or undergoing surgery. IV therapy restores fluid balance, replenishes electrolytes, and delivers medications effectively throughout the body.
Comprehensive IV Fluid Administration
Administering IV fluids requires precise calculation and the correct choice of equipment. Safety checks include verifying the fluid type, expiration date, and clarity of the solution.
How Do You Calculate IV Drip Rates?
Ensuring the correct flow rate is vital to prevent fluid overload. In this video, we review the formula for calculating IV drip rates (gtts/min) using the volume to be infused and the drop factor of the tubing.
Different Routes of Parenteral Fluid Therapy
While “IV” implies a vein, the specific route depends on the patient’s condition and the type of fluid:
- Peripheral IV: A short catheter inserted into small veins (hand/arm). Suitable for short-term isotonic or hypotonic fluids.
- Central Venous Catheter (CVC): Placed in large veins (internal jugular/subclavian). Required for hypertonic fluids or vesicants to prevent vein damage.
- Intraosseous (IO): Used in emergencies when IV access fails; fluids are delivered directly into the bone marrow.
More Free Resources to Keep You at Your Best
Editorial Note
ACLS Certification Association (ACA) uses only high-quality medical resources and peer-reviewed studies to support the facts within our articles. Explore our editorial process to learn how our content reflects clinical accuracy and the latest best practices in medicine. As an ACA Authorized Training Center, all content is reviewed for medical accuracy by the ACA Medical Review Board.