HHS vs. DKA: Understanding the Differences
ACLS Certification Association videos have been peer-reviewed for medical accuracy by the ACA medical review board.
Article at a Glance
- Hyperosmolar hyperglycemic syndrome is a complication of type 2 diabetes.
- The blood glucose for hyperosmolar hyperglycemic syndrome is typically much higher than diabetic ketoacidosis.
- Clinicians will learn how hyperosmolar hyperglycemic syndrome differs from diabetic ketoacidosis.
Hyperosmolar Hyperglycemic Syndrome
Hyperosmolar hyperglycemic syndrome (HHS) is similar to diabetic ketoacidosis (DKA), but there are several differences we will review in this article.
How common is HHS?
HHS is less common than DKA and is estimated to account for less than 1% of hospital admissions in patients with diabetes.
What Are the Risk Factors for Hyperosmolar Hyperglycemic State (HHS)?
Patients with type 2 diabetes are at risk of HHS. Physicians must remember:
- The emergency complication of type 2 diabetes is HHS.
- The emergency complication of type 1 diabetes is DKA.
HHS most often occurs in people with type 2 diabetes (including undiagnosed diabetes), especially when an illness or stressor causes severe dehydration and sustained hyperglycemia.
- Underlying diabetes factors: Type 2 diabetes, missed medications, limited access to water, or inability to self-manage (older age, cognitive impairment).
- Infections (very common triggers): Pneumonia, urinary tract infection, sepsis—often drive stress hormones that raise glucose and worsen dehydration.
- Acute medical events: Stroke, myocardial infarction, pancreatitis, trauma, surgery, burns.
- Medications that raise glucose or promote dehydration: Glucocorticoids, thiazide/loop diuretics, atypical antipsychotics, some sympathomimetics; anything that reduces fluid intake can worsen risk.
- Dehydration/limited intake: Vomiting/diarrhea, poor oral intake, heat exposure, inadequate caregiving support.
Quick clinical reminder: HHS is classically linked to type 2 diabetes, while DKA is classically linked to type 1 diabetes—however, either condition can occur outside these “classic” patterns depending on the trigger and insulin availability.
DKA vs. HHS: A Detailed Comparison
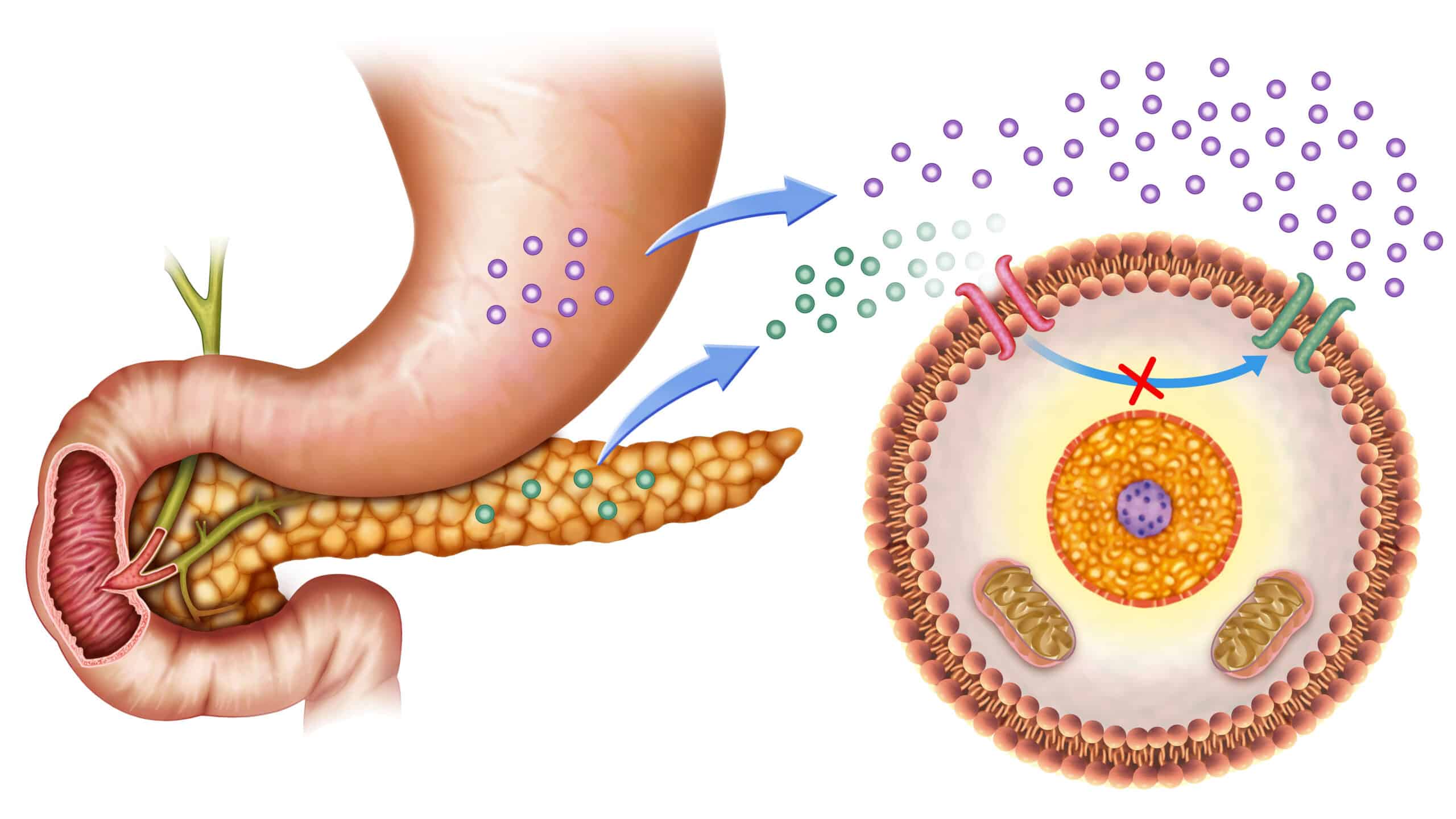
There are little to no ketone bodies in the blood in HHS since patients with type 2 diabetes have insulin in their bodies to protect against lipolysis. Lipolysis, or the breakdown of fat, leads to the build-up of ketone bodies present in DKA. A hallmark DKA symptom is the presence of ketone bodies. A type 1 diabetic does not produce insulin to bring glucose into the cells. Therefore, the cells do not have glucose available as an energy source, so the body breaks down fats instead via lipolysis. The extracellular fluid (ECF) of the vascular space with an HHS patient is extremely hyperosmolar due to elevated blood glucose. Osmolality (or colloid osmotic pressure) is created by albumin, glucose, sodium, and other components in the vascular space. Due to the hyperosmolar ECF, the body tries to dilute the blood to rid itself of the extra glucose. When glucose is removed through the urine, water follows. Therefore, patients with HHS are at risk of extreme dehydration due to water loss.
Pathophysiology
Diabetic ketoacidosis (DKA) and hyperosmolar hyperglycemic syndrome (HHS) both result from insulin deficiency, but the degree and metabolic consequences differ significantly. In DKA, an absolute or near-absolute lack of insulin leads to unchecked lipolysis. Fat breakdown produces ketone bodies, resulting in metabolic acidosis. This process occurs rapidly and is most common in patients with type 1 diabetes.
In contrast, HHS occurs in the presence of relative insulin deficiency. There is enough insulin to suppress ketone formation but not enough to prevent severe hyperglycemia. Profound hyperosmolarity develops, causing osmotic diuresis, extreme dehydration, and altered mental status.
Treatment Protocols
Although both conditions are medical emergencies, treatment priorities differ slightly between DKA and HHS.
- Fluid resuscitation: The first and most critical intervention for both DKA and HHS. Patients with HHS often require larger fluid volumes due to more severe dehydration.
- Insulin therapy: Continuous intravenous insulin is essential in DKA to halt ketone production. In HHS, insulin is used cautiously after fluid replacement to gradually lower blood glucose.
- Electrolyte management: Potassium levels must be closely monitored in both conditions. Hypokalemia is particularly dangerous in DKA once insulin therapy begins.
- Treatment of underlying causes: Infections, myocardial infarction, stroke, or medication-related triggers must be identified and managed.
Diagnostic Criteria Overview
DKA is characterized by hyperglycemia, metabolic acidosis, and ketonemia, whereas HHS is defined by extreme hyperglycemia, high serum osmolality, and minimal or absent ketosis. While laboratory thresholds differ, clinical context and overall presentation guide diagnosis and management decisions.
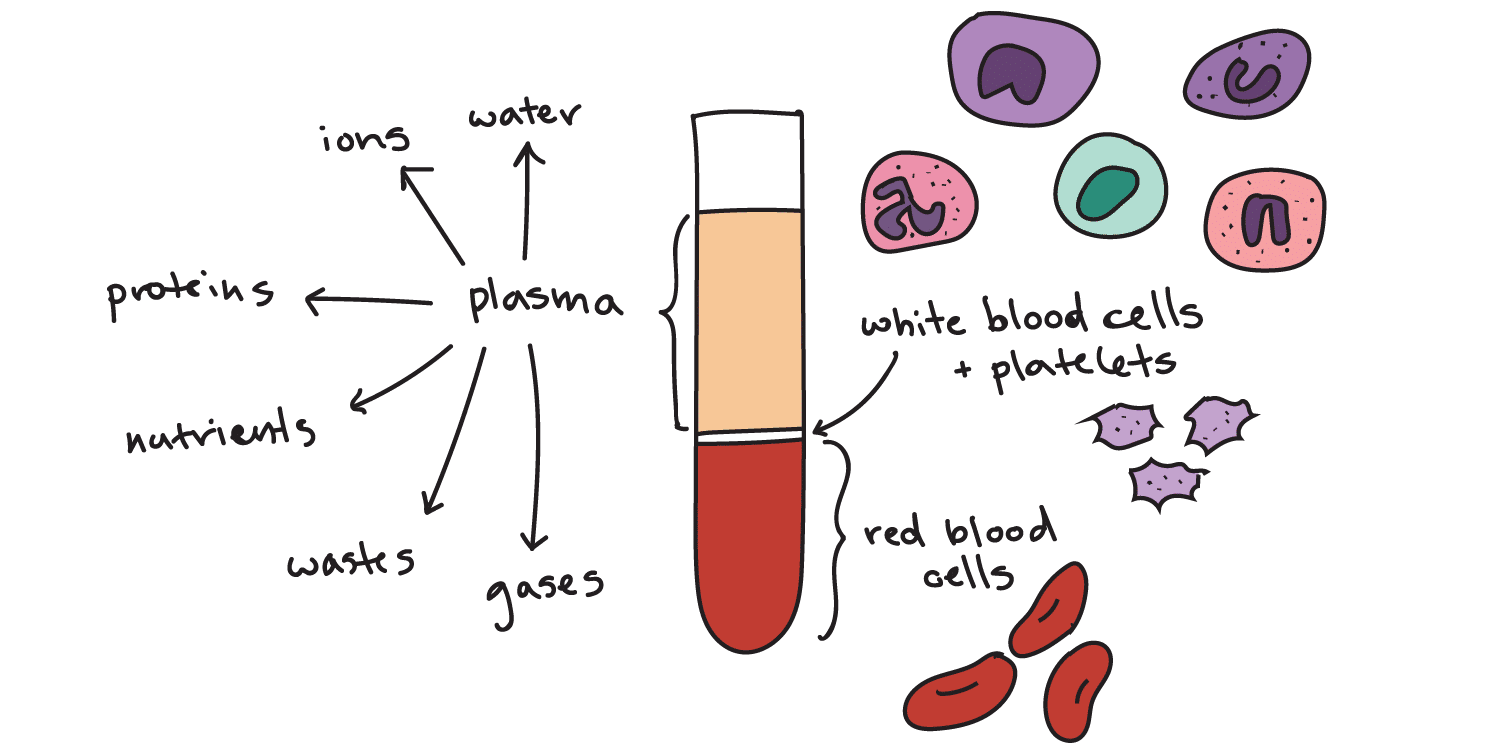
Blood contains components such as albumin (protein), glucose, and sodium that contribute to the osmotic pressure of the blood.
Read: Coronary Artery Disease vs. Peripheral Artery Disease
Fatal Complications of HHS
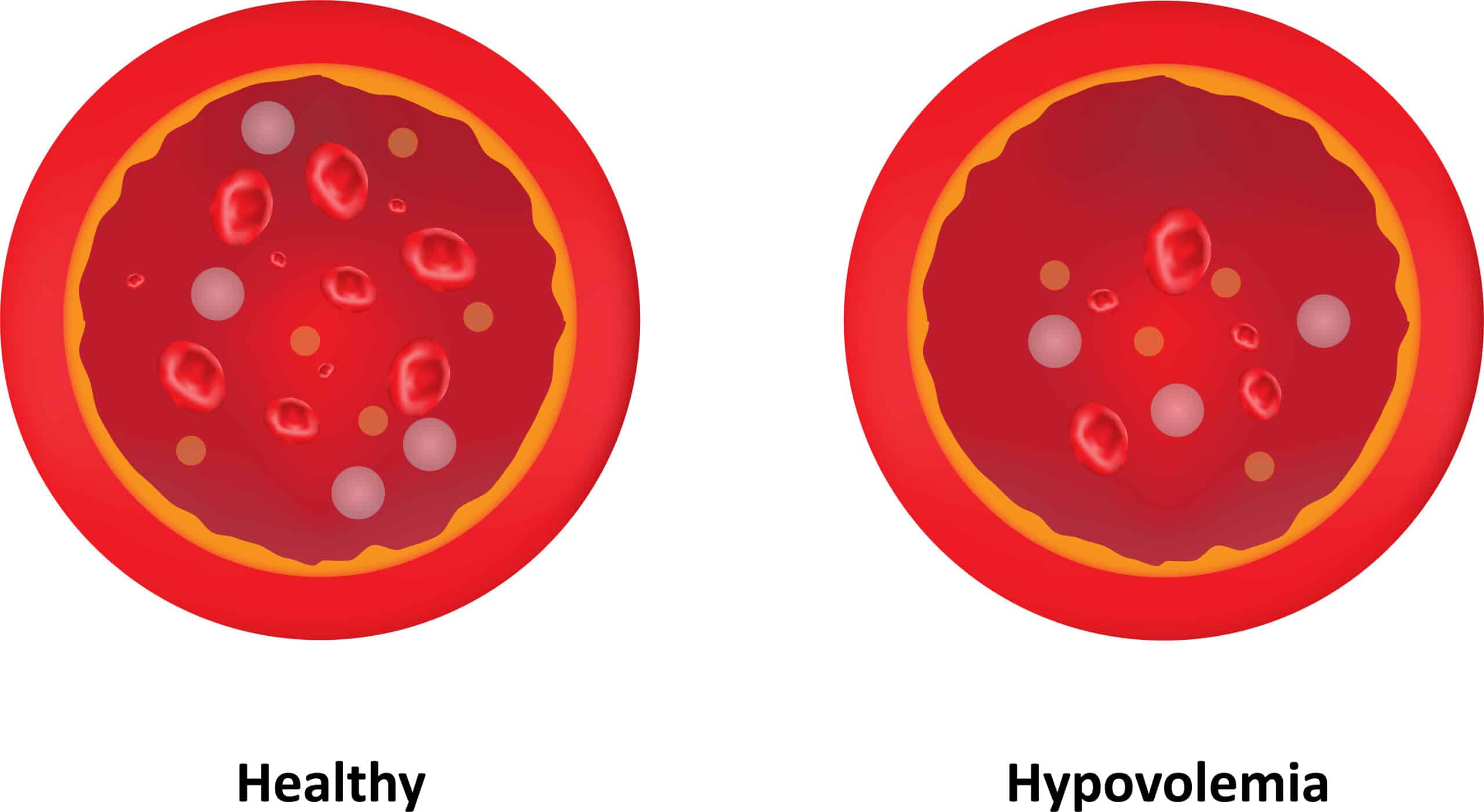
The main concern with HHS is hypovolemia. Fluid replacement is crucial because osmotic diuresis is very severe in these patients. The polyuria from hyperglycemia causes osmotic diuresis. To compare HHS and DKA:
- Hypovolemia is the main concern with HHS.
- Hypokalemia is the main concern with DKA.
Both diabetic ketoacidosis (DKA) and hyperosmolar hyperglycemic syndrome (HHS) are associated with serious complications if not treated promptly. While mortality is higher in HHS, both conditions can result in life-threatening outcomes.
- Severe dehydration and hypovolemic shock, especially in HHS due to prolonged osmotic diuresis
- Electrolyte abnormalities, including hypokalemia, hyperkalemia, and sodium disturbances
- Cerebral edema, more commonly associated with DKA, particularly in younger patients
- Acute kidney injury resulting from prolonged hypovolemia
- Cardiac arrhythmias secondary to electrolyte shifts
- Thromboembolic events, which occur more frequently in HHS due to increased blood viscosity
Early recognition and aggressive management significantly reduce the risk of these complications.

Patients with HHS are constantly urinating and thirsty. They may become dehydrated.