Respiratory Arrest Management: Ventilation Devices and Airway Support
This guide provides a comprehensive overview of respiratory arrest management, focusing on the safe and effective use of various ventilation devices. Designed for ACLS providers, nurses, and medical professionals, this article will teach you how to recognize respiratory arrest, step through the initial management sequence, and select the appropriate airway device based on the patient’s clinical presentation.
ACLS Certification Association videos have been peer-reviewed for medical accuracy by the ACA medical review board.
Article at a Glance
- Immediate Action: For a patient with a pulse who is not breathing, immediately open the airway and begin rescue breathing (1 breath every 6 seconds).
- Device Progression: Start with basic barrier devices (mouth-to-mask) or bag-mask ventilation, and escalate to advanced supraglottic airways if basic methods fail.
- Mouth-to-Mouth Context: While direct mouth-to-mouth resuscitation is no longer encouraged in healthcare settings due to infection risks, it may be necessary as a last-resort, life-saving option in out-of-hospital emergencies.
- Avoid Over-Ventilation: Delivering breaths too rapidly or forcefully can cause severe complications, including gastric inflation and decreased cardiac output.
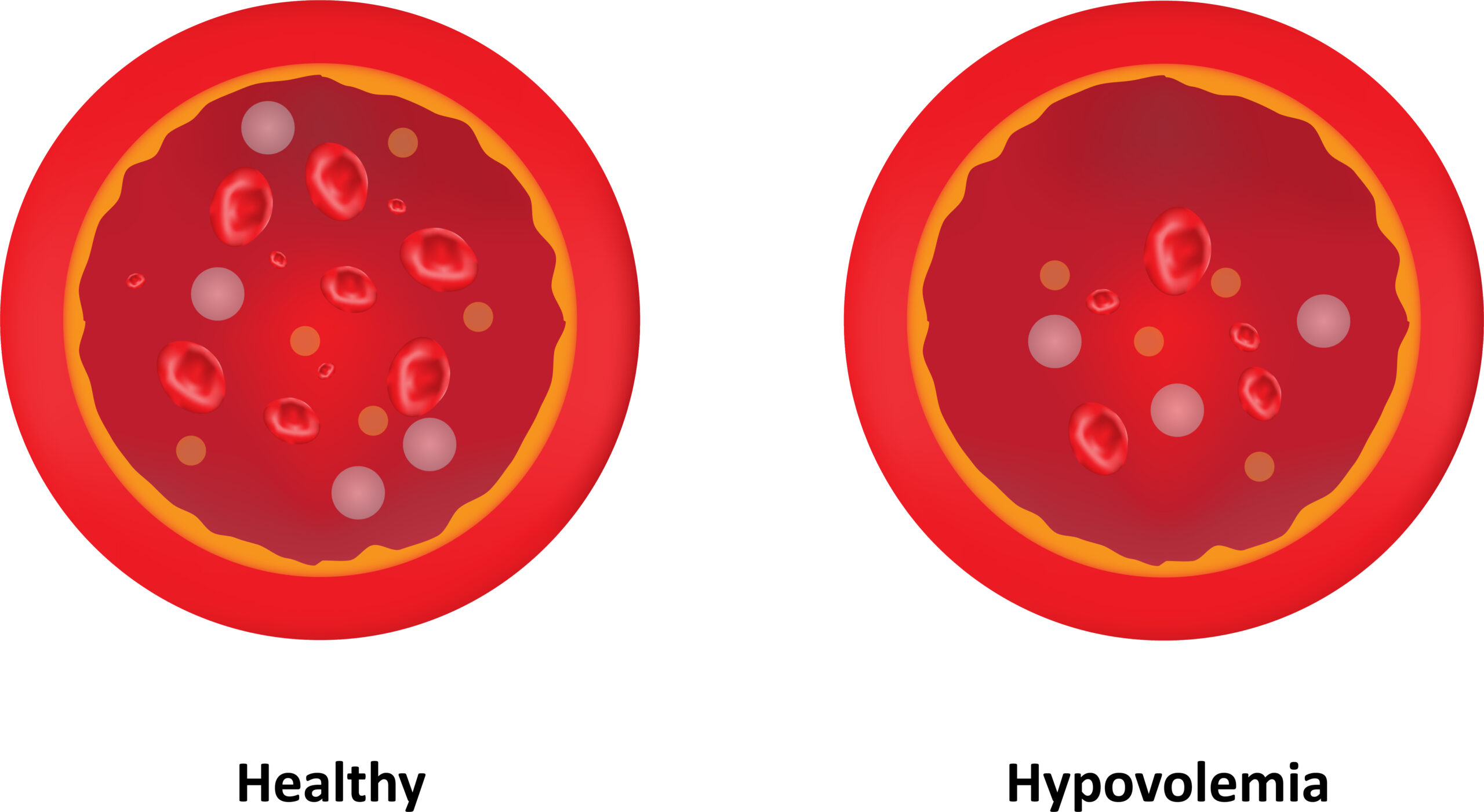
What is respiratory arrest?
Respiratory arrest is a life-threatening medical emergency where a patient completely stops breathing, although they may still have a palpable pulse. Without immediate intervention to restore oxygenation and ventilation, respiratory arrest will rapidly deteriorate into full cardiac arrest. For a deeper dive into the specific types and underlying pathophysiology, visit our complete guide on Respiratory Arrest and Airway Management.
How to Manage a Respiratory Arrest?
Managing a respiratory arrest requires a rapid, systematic approach to restore oxygenation while preventing cardiac arrest. If you assess a patient and find a pulse present but they are not breathing (or only gasping), follow this core sequence:
How is respiratory arrest treated?
The fundamental treatment principles follow a logical progression: open the airway, deliver ventilations, optimize oxygen, and identify the cause.
- Create or Clear the Airway: Immediately open the airway using the head tilt-chin lift or jaw thrust maneuver. If secretions or vomit are present, suction the airway clear before attempting to insert any advanced devices.
- Ventilate: Begin rescue breathing immediately using a bag-mask or barrier device. Deliver 1 breath every 6 seconds (10 breaths per minute), ensuring visible chest rise with each breath.
- Optimize Oxygen and Monitor: Attach supplemental oxygen as soon as available. Titrate the oxygen to achieve a target SpO2 of 94% or greater. If an advanced airway (like an endotracheal tube or supraglottic device) is placed, you must confirm proper placement using continuous waveform capnography (ETCO2) alongside observing bilateral chest rise.
- Determine and Treat the Underlying Cause: Once the airway is secured and the patient is oxygenating, investigate why they stopped breathing. This may involve ordering an Arterial Blood Gas (ABG), a Complete Blood Count (CBC), electrolyte panels, toxicology screens, and a portable chest X-ray to assess lung fields and confirm advanced airway depth.
Mouth-to-Mask Ventilation
Mouth-to-mask ventilation is administered using a barrier device with a one-way valve to prevent contact with blood, vomitus, or other secretions.1
Follow these steps for proper mouth-to-mask ventilation:
- Mask Sizing: Ensure the mask is the correct size. It should cover the nose and mouth without extending below the chin or encroaching on the eyes.
- Placement: For triangular masks, place the pointier edge over the bridge of the nose and the wider base over the mouth and upper chin.
- Head Tilt-Chin Lift: While holding the mask firmly, perform the head tilt-chin lift maneuver (tilting the head back and lifting the chin to pull the tongue away from the back of the throat). This is a fundamental part of early airway management (the process of ensuring an open path for air to reach the lungs).
- Breath Timing: Take a normal breath and deliver one breath over 1 second, delivering 1 breath every 6 seconds (10 breaths per minute).
- Reassessment: Watch for visible chest rise with each breath, and ensure the chest relaxes fully between breaths.
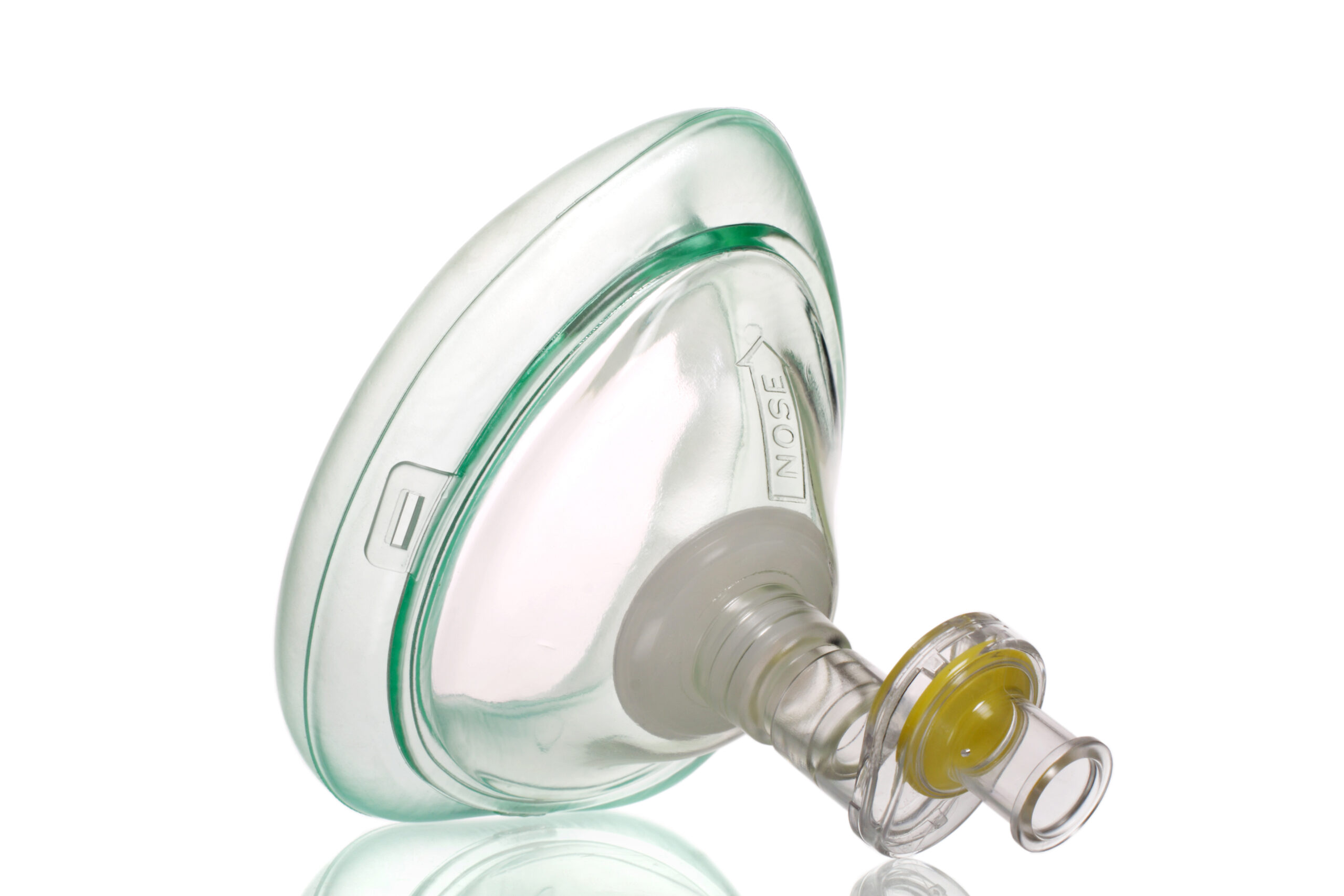
One-way valve masks need to fit properly on the patient’s face.
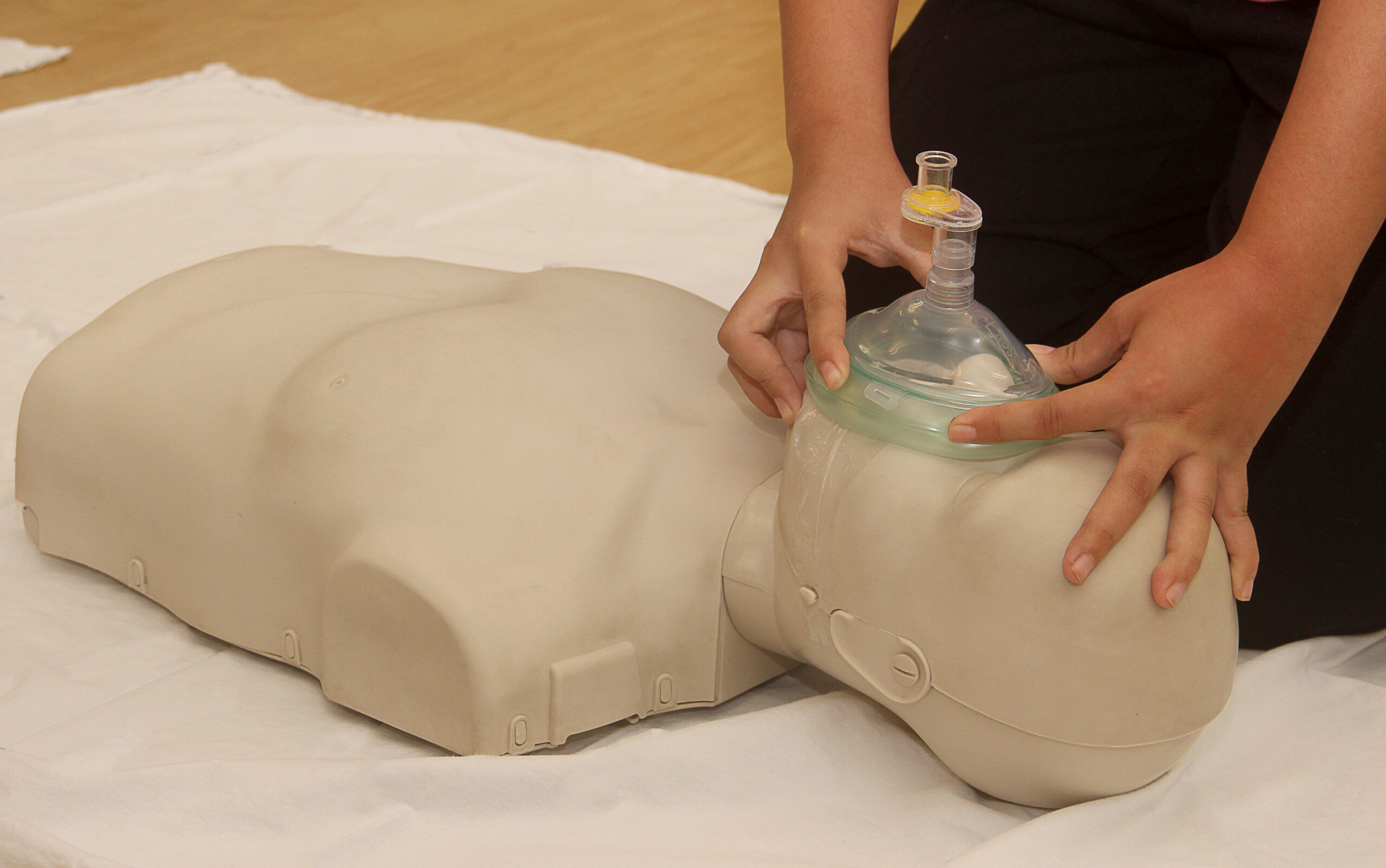
Many health professionals carry their own masks to have on hand in case of emergency.
While providing direct mouth-to-mouth ventilation used to be common, this practice is no longer recommended in clinical settings due to the risk of contracting or spreading infectious illnesses. However, in certain out-of-hospital situations where no barrier devices are available, providing direct mouth-to-mouth ventilations may be the only life-saving recourse.
Providing mouth-to-mouth ventilations involves performing the head tilt-chin lift maneuver, holding the airway open with the palm of one hand on the forehead, and simultaneously pinching the nostrils closed. With the other hand, grasp the chin and pull it gently upward. Deliver a normal breath over 1 second to achieve adequate chest rise (1 breath every 6 seconds).
Room air is about 21% oxygen. When a person takes a normal breath and breathes out, 80% of the oxygen inhaled is still available. Therefore, ventilating patients with air from your lungs provides enough oxygen for survival.2 In clinical practice, however, providers rely on different types of oxygen delivery devices to ensure optimal oxygenation.

Mouth-to-mouth ventilation is no longer recommended in clinical settings but may be indicated in severe out-of-hospital emergencies.
Rescue Breathing for Adults
To see these barrier device techniques applied in a clinical scenario, watch this demonstration on Rescue Breathing for Adults, which covers the proper head tilt-chin lift and pacing of breaths.
Rescue Breathing for Children
The anatomy and ventilation rates for pediatric patients differ from adults. This video explains how to adjust your technique and breath timing when performing Rescue Breathing for Children.
Understanding Infant Rescue Breathing
Infants require extremely precise air volumes to prevent lung injury. Review the differences in mask placement and volume delivery in this guide to Understanding Infant Rescue Breathing.
Read: Respiratory Arrest and Airway Management: Maintaining Airway Patency
Bag-Mask Devices
As mentioned in our earlier How to Manage a Respiratory Arrest sequence, ventilating the patient is a top priority. When available, a Bag-Valve-Mask (BVM) device is a more effective tool to provide positive-pressure ventilation to patients who are not breathing or who are breathing ineffectively.3 Bag-mask ventilation allows oxygen-enriched air to be pushed into the patient’s lungs, and then from the lungs into the bloodstream to support vital organs. Proper use should be guided by findings from a respiratory assessment.
Bag-mask devices have three main parts: the mask portion, the bag part that is attached to oxygen, and the reservoir bag (which should be fully inflated when the device is attached to 15 L/minute of oxygen). Even without a compressed gas source, self-inflating bags can still deliver 21% room-air oxygen.
To maximize efficiency, an oropharyngeal airway (a rigid plastic curve inserted into the mouth to keep the tongue from blocking the throat) is often used in conjunction with a bag-mask device.
Mastering the bag-mask device requires practice. Follow these steps:
- Positioning: Use the correctly sized face mask to form a tight seal over the patient’s nose and mouth.
- The “E-C Clamp” Technique (One-Person): Form a “C” with your thumb and index finger to press the mask firmly against the face. Use your middle, ring, and pinky fingers (forming an “E”) to hook under the mandible (lower jaw) and lift it upward into the mask. Avoid putting pressure on the soft tissues of the neck, and do not just push the mask down, as this can occlude the airway.
- The Two-Person Technique: Because bagging can be difficult for people with small hands or patients with complex facial structures, the two-person technique is highly preferred. One rescuer uses both hands to perform a double E-C clamp to maintain a perfect seal, while the second rescuer squeezes the bag.
- Squeeze: Squeeze the bag just hard enough to cause the chest to rise, delivering one breath over 1 second (1 breath every 6 seconds). The rise of the patient’s chest should appear as though they are taking a natural breath.
The Dangers of Over-Ventilation: A common and dangerous mistake during respiratory arrest management is squeezing the bag too hard or too fast. Excessive ventilation can cause:
- Stomach Insufflation: Forcing air down the esophagus instead of the trachea.
- Aspiration: Stomach inflation drastically increases the risk of vomiting and inhaling gastric contents into the lungs.
- Decreased Cardiac Output: High pressure in the chest cavity prevents blood from returning to the heart, plummeting blood pressure and organ perfusion.
Understanding Bag Valve Mask Usage During CPR
To properly visualize the E-C clamp technique and see the proper volume to squeeze during an emergency, review this demonstration on Understanding Bag Valve Mask Usage During CPR.
Supraglottic Devices
When basic bag-mask ventilation is failing to oxygenate the patient, providers must escalate the airway. Supraglottic (meaning “above the vocal cords”) devices are an excellent middle ground before full endotracheal intubation.
Consider LMA or LTs when basic BVM ventilation is ineffective, when you need to free up a provider’s hands during a code, or when the patient has difficult facial anatomy that prevents a tight BVM seal.
There are two main supraglottic devices. Both have advantages and disadvantages.
The laryngeal mask airway (LMA) is composed of a ventilation tube attached to a small inflatable mask. It is inserted into the mouth to sit in the hypopharynx (the lower part of the throat) and cover the glottic opening, allowing air to pass directly into the trachea.4
Laryngeal tubes (LTs) are airway devices primarily designed to blindly intubate the esophagus, which is far easier than intubating the trachea. These tubes come with two cuffs: one that inflates to block the esophagus and one to block the upper pharynx, forcing air to exit through holes directly into the trachea.
Advantages:
- The LMA and LT can be inserted quickly and blindly, without the use of a laryngoscope.
- They are highly effective for patients with “difficult airways” that are hard to intubate.
- Once placed, they free up the rescuers’ hands for other critical ACLS tasks.
Disadvantages:
- Aspiration Risk: Because the tube does not pass through the vocal cords, the airway is not as well protected from stomach contents as it is with a definitive endotracheal tube.
- Auscultation Difficulty: It can be much harder to auscultate (listen with a stethoscope) for clear breath sounds when these devices are used. Therefore, continuous capnography (monitoring exhaled CO2) is critically important to confirm and monitor placement.
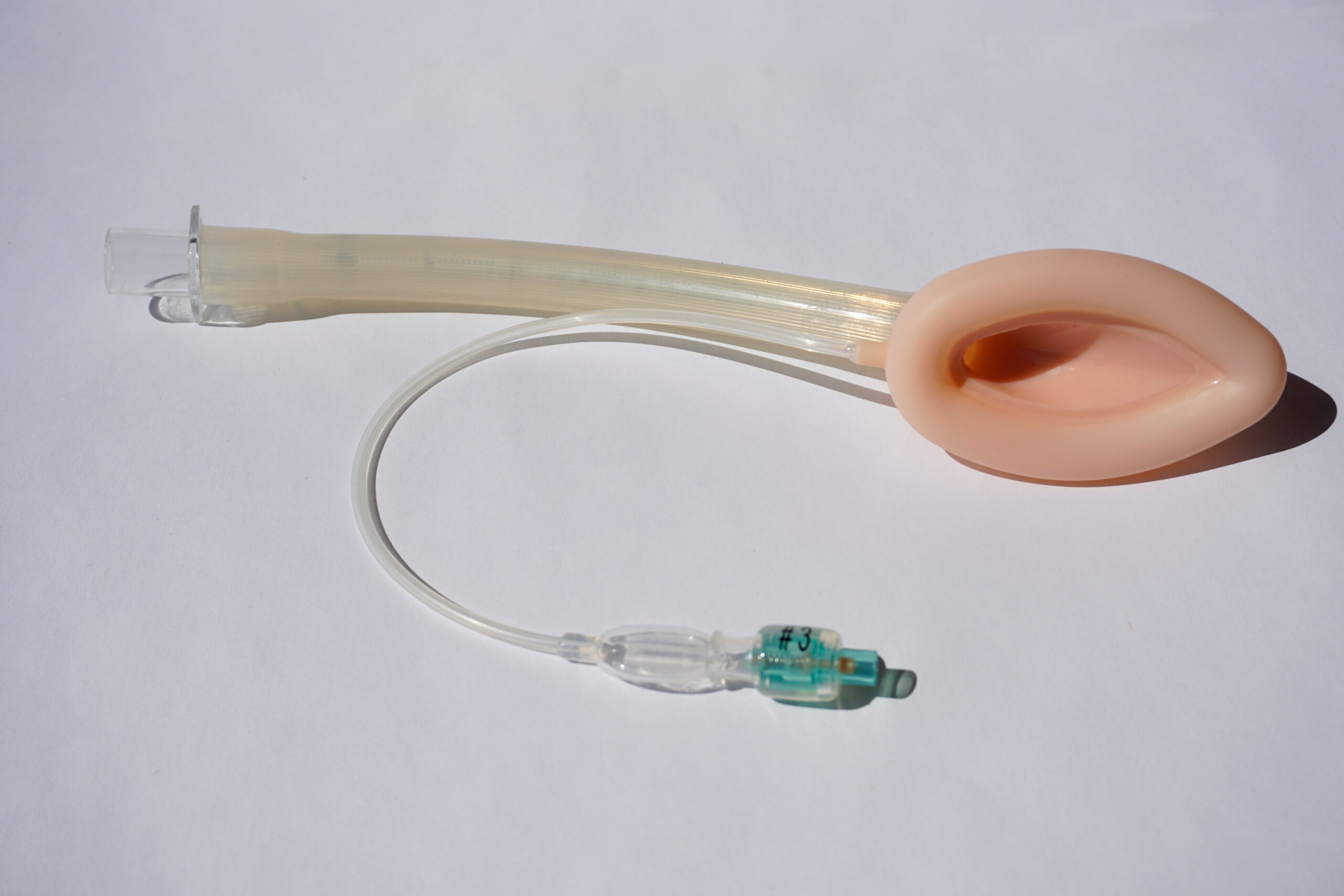
Laryngeal Mask Device (LMA)
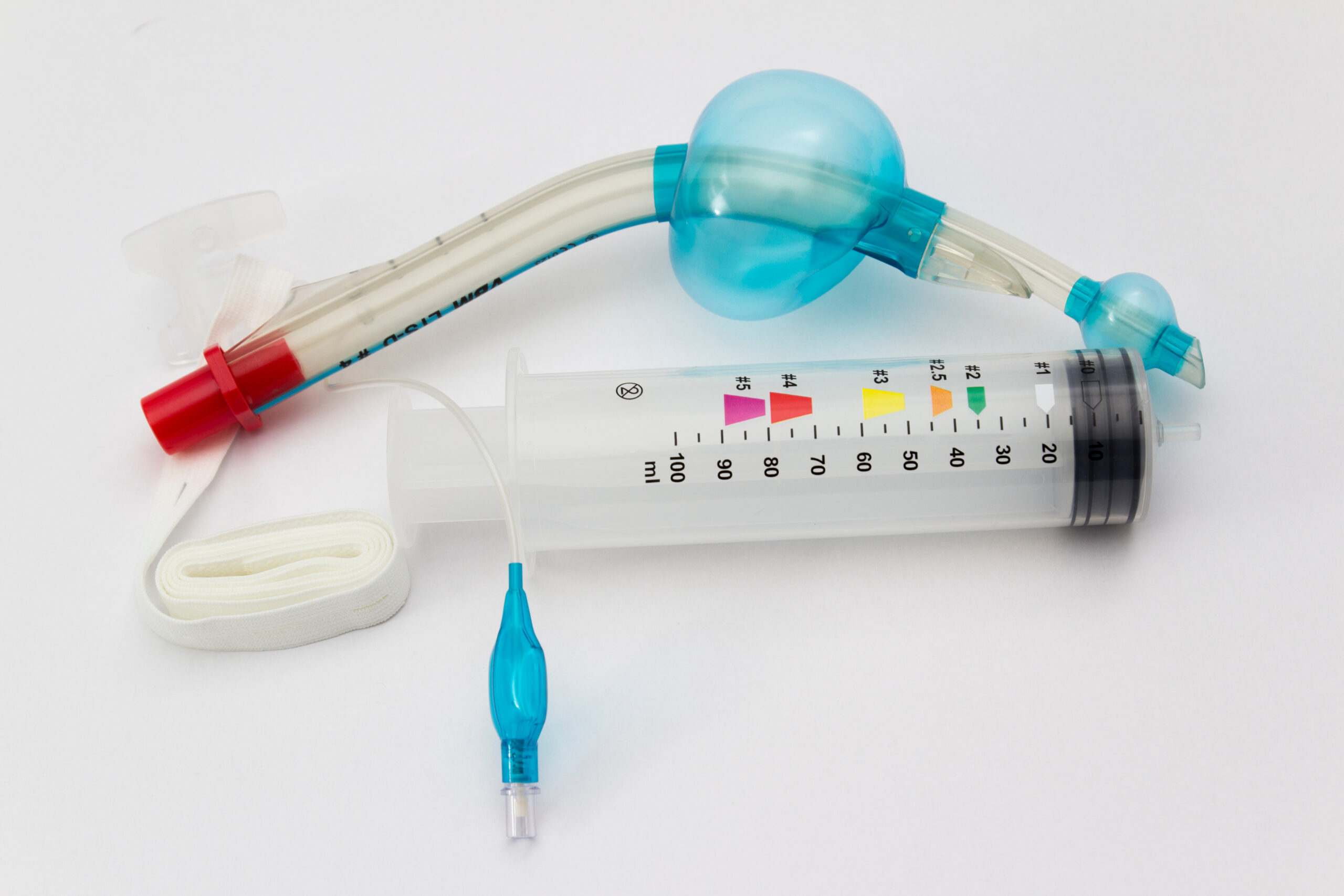
Laryngeal Tube (LT)
Summary
Proper respiratory arrest management relies on quick recognition and the stepwise escalation of airway devices. Providers should immediately open the airway and initiate ventilations at a rate of 1 breath every 6 seconds using a pocket mask or Bag-Valve-Mask (BVM). To prevent dangerous complications like gastric insufflation and reduced cardiac output, avoid squeezing the bag too hard or too fast. If basic BVM ventilation is insufficient, blindly inserted supraglottic devices (like the LMA or LT) provide a rapid, hands-free bridge to definitive airway control, provided placement is verified with continuous capnography.
More Free Resources to Keep You at Your Best
Editorial Sources
ACLS Certification Association (ACA) uses only high-quality medical resources and peer-reviewed studies to support the facts within our articles. Explore our editorial process to learn how our content reflects clinical accuracy and the latest best practices in medicine. As an ACA Authorized Training Center, all content is reviewed for medical accuracy by the ACA Medical Review Board.
1. American Heart Association. Adult Basic Life Support. 2000.
2. Stallinger A, Wenzel V, Oroszy S, et al. The effects of different mouth-to-mouth ventilation tidal volumes on gas exchange during simulated rescue breathing. Anesth Analg. 2001.
3. Joshua T. Bucher; Rishik Vashisht; Megan Ladd; Jeffrey S. Cooper. Bag Mask Ventilation. National Library of Medicine. 2022.
4. Leslie V. Simon; Klaus D. Torp. Laryngeal Mask Airway. National Library of Medicine. 2022.