Pathophysiology of Increased Intracranial Pressure (ICP)
This guide explores the underlying mechanisms, common causes, and clinical manifestations of increased Intracranial Pressure (ICP). Designed for ACLS providers, nurses, and medical students, this article will equip you to understand the pathophysiology of ICP, recognize early versus late warning signs, and understand the critical concept of the fixed cranial vault to optimize your patient assessments.
ACLS Certification Association videos have been peer-reviewed for medical accuracy by the ACA medical review board.
Article at a Glance
- The Fixed Vault Mechanism: The skull is a rigid container holding brain tissue, blood, and cerebrospinal fluid (CSF). An increase in one compartment requires a decrease in another to maintain normal pressure.
- Common Etiologies: ICP rises due to space-occupying lesions (tumors, hematomas), cerebral edema, or obstructions in CSF flow.
- Clinical Progression: Symptoms evolve predictably from early, subtle changes (such as altered mental status) to late, life-threatening indicators (Cushing Triad).
What is increased intracranial pressure (ICP)?
Intracranial pressure (ICP) measures the pressure exerted by fluids and tissues inside the skull on the brain. Because the adult skull is a rigid, fixed-volume bone vault, it cannot expand to accommodate extra volume. Increased ICP occurs when the pressure within this fixed cranial vault rises above normal physiological limits (typically 5 to 15 mmHg in resting adults). This elevation directly threatens cerebral perfusion and can lead to catastrophic brain shifting or herniation if left untreated.
What causes increased intracranial pressure?
Increased ICP arises from:
- An increase in cerebrospinal fluid (CSF).
- An increase in the amount of blood or cerebral blood flow.
- An increase in brain tissue, including cerebral swelling or cerebral edema.
- A combination of these etiologies.
What causes increased intracranial pressure?
Increased ICP arises from:
- An increase in cerebrospinal fluid (CSF).
- An increase in the amount of blood or cerebral blood flow.
- An increase in brain tissue, including cerebral swelling or cerebral edema.
- A combination of these etiologies.
The CSF, blood, and brain tissue are the three main elements that occupy the skull. If there is an increase in any of these elements without a compensatory decrease in another, the ICP will increase.
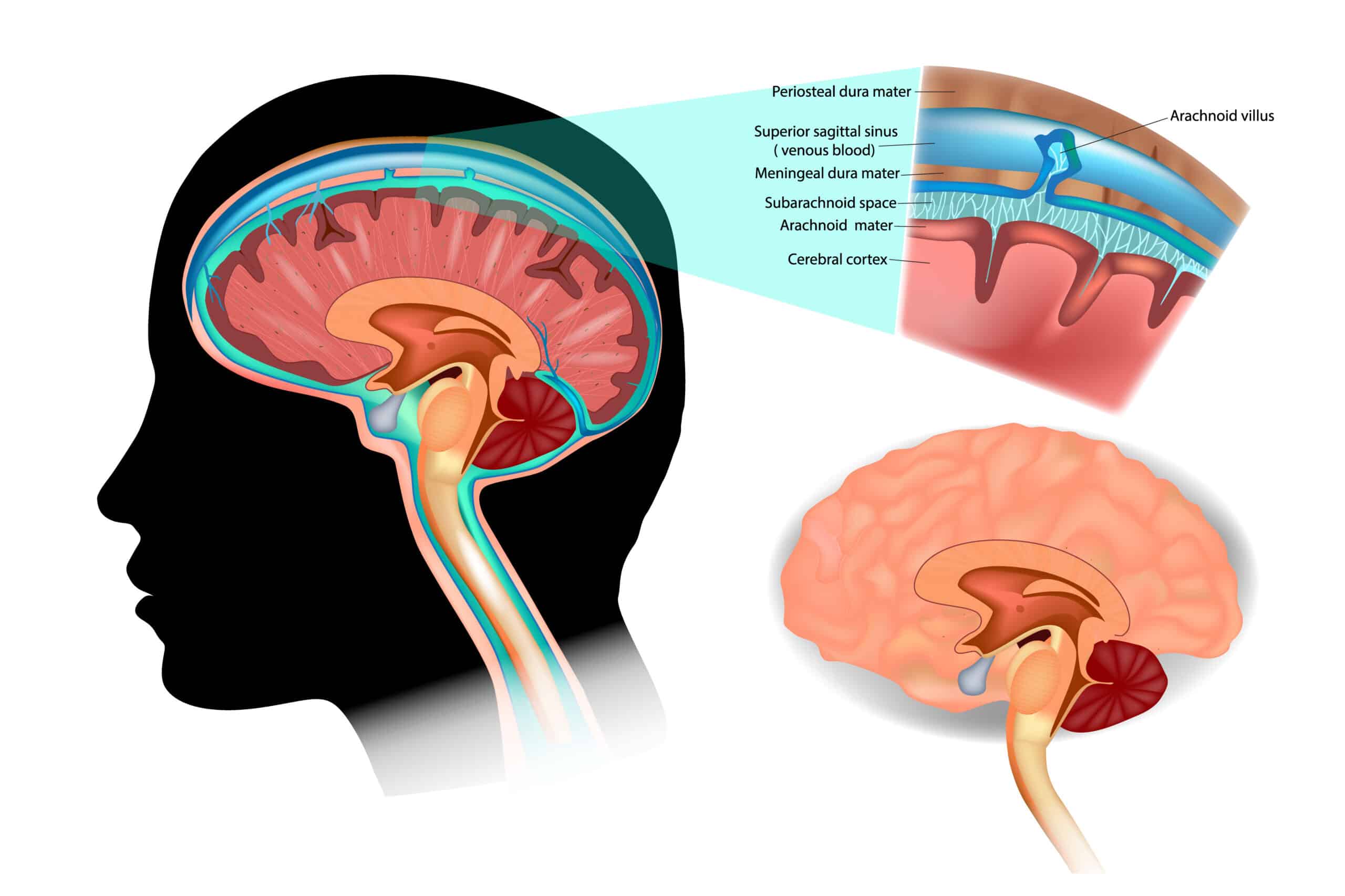
Respiratory acidosis can eventually lead to increased intracranial pressure.
Changes in these elements occur for different clinical reasons. For example, an increase in CSF is observed in hydrocephalus or infectious processes like meningitis. An increase in blood volume can result from hemorrhagic strokes, traumatic epidural/subdural hematomas, or profound vasodilation. Finally, an increase in brain tissue volume is strongly associated with ischemic stroke, brain tumors, or traumatic brain injuries that cause widespread cellular swelling and edema.
Because rising pressure directly impacts brain function, performing a prompt and accurate neurological assessment is vital for detecting these subtle early changes before permanent damage occurs.
A Case to Illustrate Increased ICP
To see how this three-compartment pathophysiology works in practice, let’s look closely at the blood compartment. A patient presents with respiratory acidosis. This presentation is fairly common in patients with emphysema and chronic obstructive pulmonary disease (COPD) and occurs when the amount of carbon dioxide (CO2) in the body increases.
Because CO2 is a potent vasodilator and readily crosses the blood-brain barrier, the patient may experience rapid neurological changes. When CO2 enters the brain, it causes significant cerebral vasodilation, which increases cerebral blood flow. This sudden increase in blood volume within the fixed cranial vault disrupts the delicate balance, directly leading to increased intracranial pressure.
Note: While the specific pathophysiological pathway to increased ICP differs based on the underlying etiology (e.g., tumor vs. bleeding vs. vasodilation), the resulting clinical patterns often overlap significantly as the brain experiences compression.

Respiratory acidosis can eventually lead to increased intracranial pressure.
Read: Peripheral Vascular Disease
What Are the Signs and Symptoms?
There are both early and late-stage signs and symptoms of increased ICP. The very first sign of increased intracranial pressure is almost always a change in the patient’s level of consciousness or altered mental status.
It is vital for the provider to recognize these early indicators to correct the underlying etiology before irreversible damage occurs. If the underlying cause is not addressed, it can lead to severe brain compression. Once late-stage signs and symptoms present, it serves as a critical warning that brainstem herniation may be rapidly approaching.
The early signs and symptoms of ICP are:
- Restlessness
- Agitation
- Confusion
- Headache
- Nausea or vomiting
In these early stages, the patient may seem inexplicably “off” after previously being calm, alert, and oriented. They will increasingly become restless and agitated, and may report a headache (from pressure stretching the meninges) or sudden projectile vomiting (from direct pressure on the medulla—the vomiting center of the brain).
Cushing Triad: A Unique Set of Symptoms
The Cushing Triad is a late, distinct presentation of symptoms caused by significantly elevated ICP. The triad includes an increase in the systolic blood pressure (widening pulse pressure), a decrease in the heart rate (bradycardia), and a decrease or irregularity in the respiratory rate.
It is important to understand the pathophysiology of why these symptoms occur:
- Increase in Systolic Blood Pressure. An increase in ICP physically compresses cerebral blood vessels, which directly decreases Cerebral Perfusion Pressure (CPP). CPP is the net pressure driving oxygen to the brain. When the body senses that CPP is dropping and the brain is starving for oxygen, the sympathetic nervous system triggers a massive release of norepinephrine. This aggressively drives up systemic systolic blood pressure in a desperate attempt to force blood past the high intracranial resistance.
However, as the systolic blood pressure increases, a similar increase will not be seen in the diastolic pressure. Instead, what will result is a widened pulse pressure.
- Decrease in the Heart Rate. The severe increase in systolic blood pressure triggers stretch receptors (baroreceptors) in the carotid arteries and aorta that sense extreme pressure changes. The baroreceptors then stimulate the vagus nerve, prompting the parasympathetic nervous system to drastically slow the heart rate. The body decreases the heart rate in a reflex attempt to lower the soaring systemic blood pressure.
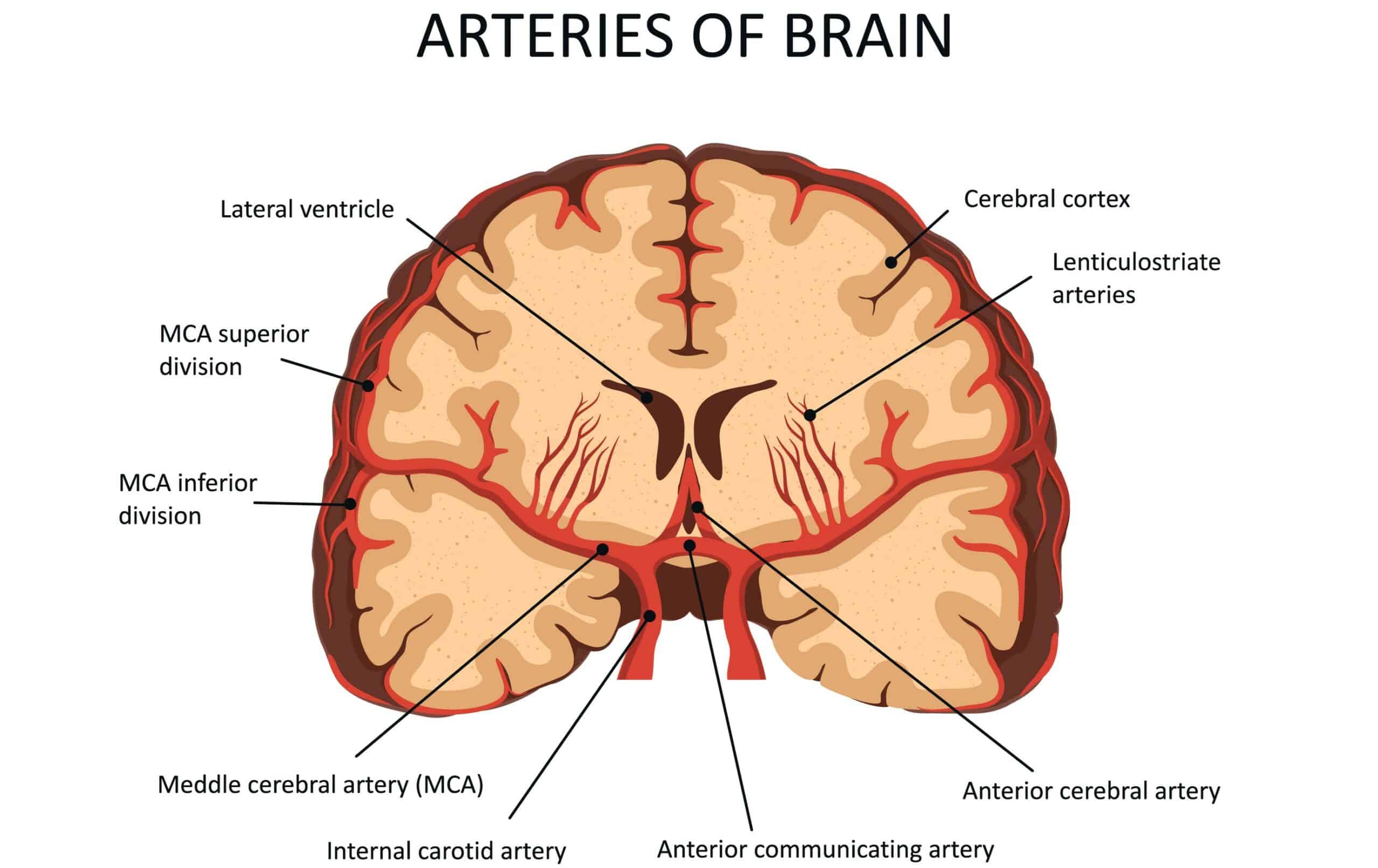
The baroreceptors in the carotid artery sense changes in blood pressure.
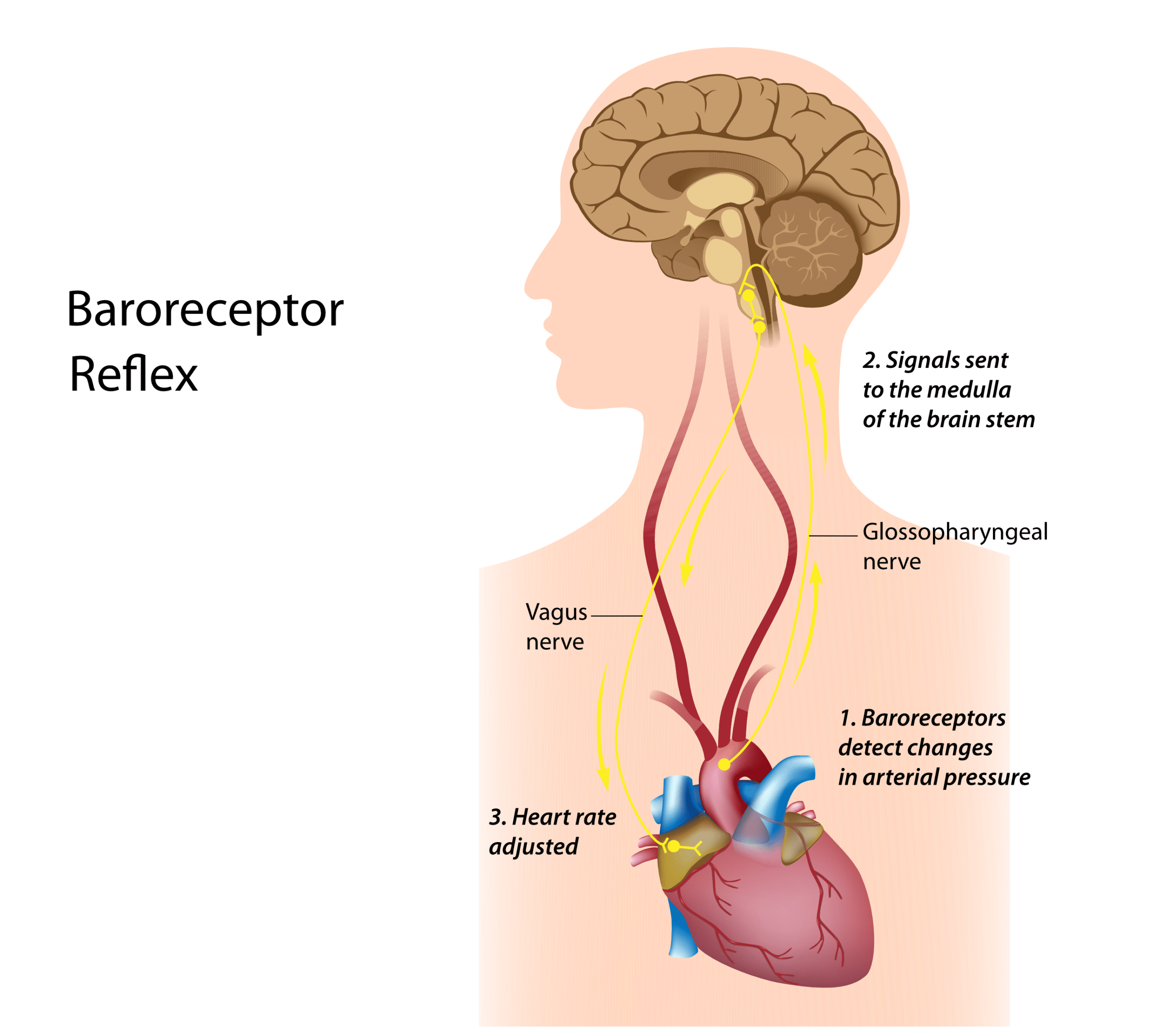
When the baroreceptors sense increased blood pressure, the body’s reflex response is to slow the heart rate.
- Decreased Respiratory Rate. Finally, the expanding physical pressure shifts brain tissue downward, putting direct mechanical pressure on the brainstem. Because the brainstem controls involuntary breathing, this physical compression causes decreased, highly irregular breathing patterns (such as Cheyne-Stokes respirations).
While different traumatic or medical etiologies initiate the rise in ICP, the physiological response of the brain being compressed inside a fixed vault yields a highly recognizable clinical pattern. Recognizing these subtle early shifts before they progress to the ominous Cushing Triad is the cornerstone of preserving neurological function.
Summary
The pathophysiology of increased intracranial pressure is rooted in the confines of a fixed cranial vault. When any of the three main compartments, brain tissue, blood, or cerebrospinal fluid, increases in volume without a compensatory decrease in another, intracranial pressure rises. This pressure compresses vital tissues and drops cerebral perfusion, leading to a predictable clinical progression. Subtle, early signs like altered mental status and headache can rapidly devolve into the Cushing Triad (hypertension, bradycardia, and irregular respirations) as brainstem herniation approaches.
Would you like me to guide you through how to properly perform the neurological assessments needed to catch these early warning signs? Reviewing standard pupillary responses and the Glasgow Coma Scale (GCS) is a great next step for any clinical provider.
More Free Resources to Keep You at Your Best
Editorial Note
ACLS Certification Association (ACA) uses only high-quality medical resources and peer-reviewed studies to support the facts within our articles. Explore our editorial process to learn how our content reflects clinical accuracy and the latest best practices in medicine. As an ACA Authorized Training Center, all content is reviewed for medical accuracy by the ACA Medical Review Board.

