Junctional Rhythm (Escape): ECG Criteria and Diagnosis
This comprehensive guide is designed for healthcare professionals and ACLS providers. It covers the essential ECG criteria, underlying causes, and clinical management of junctional escape rhythms. By the end of this article, you will be able to confidently identify a junctional escape rhythm on an ECG strip, differentiate it from other arrhythmias, and determine the appropriate care strategy to improve the overall patient outcome.
ACLS Certification Association videos have been peer-reviewed for medical accuracy by the ACA medical review board.
Article at a Glance
- Junctional escape is characterized by:
- Regularity: Regular
- Rate: 40–60 bpm
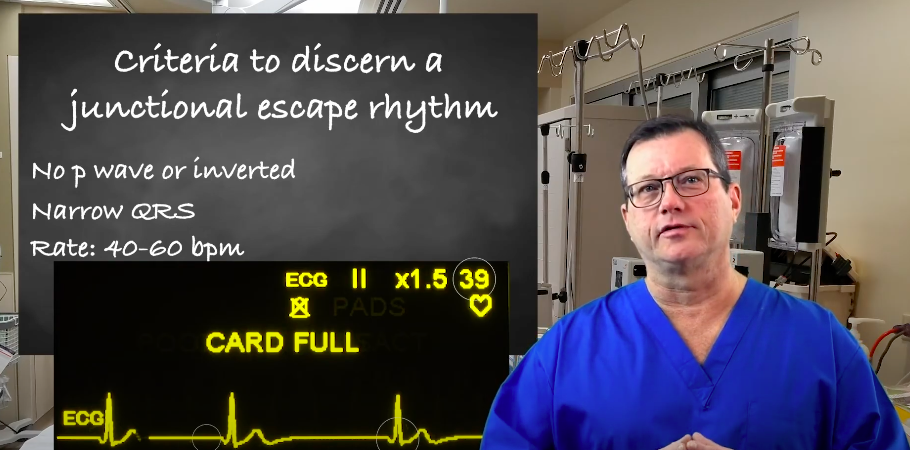
- P Wave: Inverted, if visible; may be before, after or within the QRS
- PR Interval: If before the QRS, PRI <0.20 second; otherwise, not measurable
- QRS Complex: < 0.12 second
- Terminology: A junctional escape rhythm acts as a protective backup pacemaker when the higher pacemakers (like the SA node) fail.
- ECG Recognition: Characterized by a narrow QRS complex and a rate of 40 to 60 beats per minute (bpm).
- Atrial Activity Relationship: P waves are often absent, inverted, or retrograde (appearing after the QRS) due to reverse electrical conduction.
- Clinical Management: Treatment focuses on addressing the underlying cause and assessing patient stability, rather than immediately trying to suppress this protective rhythm.
A junctional escape rhythm occurs when the sinus node slows down or fails, and the AV junction takes over as a backup pacemaker. On ECG, the key is recognizing that the rhythm originates near the AV node, which explains why the P wave may be absent or inverted, why the QRS is usually narrow, and why the rate falls into a predictable range. What does the P wave look like in a junctional escape rhythm? The P wave is often absent or inverted. This happens because atrial activation is moving backward toward the atria rather than forward from the sinus node. Depending on timing, the inverted P wave may appear: The QRS is usually narrow (normal duration) because ventricular conduction still travels through the normal His Purkinje pathway. A narrow QRS supports the idea that the impulse starts above the ventricles and then conducts normally through them. What is the normal heart rate for a junctional escape rhythm? Typically 40 to 60 beats per minute. This is the intrinsic firing rate of the AV junction. It is slower than the sinus node, but it is faster than a ventricular escape rhythm, which is why junctional escape often appears as a protective backup. Junctional escape is commonly regular or nearly regular because the AV junction fires at a steady intrinsic pace. Irregularity may appear if the underlying issue is intermittent sinus node activity or changing autonomic tone. If a P wave is visible before the QRS, the PR interval is usually short because the impulse starts near the AV node, so there is less distance and less delay before ventricular activation. If the P wave is inverted and appears after the QRS, there may be no measurable PR interval. Step-by-Step Rhythm Labeling Use the examples below to connect the criteria to what you see on an ECG strip. Focus on the P wave position or absence, the narrow QRS, and the typical junctional rate. This example highlights the most common pattern: a narrow QRS, a rate in the 40 to 60 bpm range, and an absent or inverted P wave due to retrograde atrial activation. Annotated ECG example showing key junctional escape rhythm criteria: P wave changes, narrow QRS, and typical junctional rate. In some junctional escape rhythms, the inverted P wave appears just before the QRS. When this happens, the PR interval is often short because the impulse begins near the AV junction. Sometimes the atria depolarize after the ventricles. In this pattern, the QRS occurs first, and a small inverted P wave may follow, which can be subtle and easy to miss. Visualizing these criteria in real-time is critical for accurate rhythm interpretation. In this video, we analyze an ECG Strip of a Junctional Escape rhythm, highlighting the missing P waves and the characteristic rate. Read: Rhythm-based Management in Cardiac Arrest One tip is to leave a little pressure on the Ambu bag with your thumb after administering a breath. Read: Rhythm-based Management in Cardiac ArrestCriteria for Junctional Escape Rhythm
P wave
QRS complex
Rate
Regularity
PR interval
ECG Examples of Junctional Escape Rhythm
Example 1: Classic junctional escape rhythm
Example 2: Inverted P wave before the QRS
Example 3: Retrograde P wave after the QRS
ECG Strip: Junctional Escape

Causes of Junctional Escape Rhythm
A junctional escape rhythm is usually a protective response when the sinus node slows down or conduction from the atria is suppressed. Causes often fall into a few common buckets.
Sinus Node Dysfunction
If the sinus node fails to fire reliably, the AV junction may take over to prevent profound bradycardia or asystole. This can be transient or related to underlying cardiac disease.
AV Conduction Abnormalities
When impulses from the atria do not reach the ventricles effectively, the conduction system may default to a junctional escape pacemaker. This is more likely when higher pacemakers are suppressed or blocked.
Medication Effects
Medications that slow sinus node automaticity or AV conduction can contribute, especially beta blockers, calcium channel blockers, digoxin, and some antiarrhythmics. In medication related cases, reviewing dosing, timing, and recent changes is essential.
Other Contributing Conditions
Myocardial ischemia, inferior MI, increased vagal tone, electrolyte abnormalities, hypoxia, and structural heart disease can all reduce sinus node output or alter conduction and trigger a junctional escape rhythm.
Symptoms of Junctional Escape Rhythm
Symptoms depend on how slow the rhythm is and whether cardiac output is reduced. Some patients are asymptomatic, especially if the rate remains near 60 bpm and perfusion is adequate.
- Fatigue or weakness
- Dizziness or lightheadedness
- Near syncope or syncope
- Chest discomfort
- Shortness of breath, especially with exertion
Treatment and Management of Junctional Escape Rhythm
Treatment depends on the clinical picture. A stable junctional escape rhythm can be an appropriate backup rhythm and may not require immediate intervention. Management focuses on identifying the cause and treating symptoms if perfusion is compromised.
- If asymptomatic and stable monitor, obtain a 12 lead ECG, and evaluate for reversible causes such as medication effects or ischemia.
- If symptomatic bradycardia follow bradycardia management principles, support airway and oxygenation, establish IV access, and treat based on hemodynamic status.
- Correct underlying causes adjust offending medications when appropriate, address hypoxia, correct electrolytes, and evaluate for acute coronary syndromes if suspected.
- Escalation if persistent symptomatic bradycardia or high risk conduction disease is present, pacing and specialist consultation may be required.
If you are learning junctional rhythms as a group, this page also connects well with the broader topic of junctional rhythms.
Differentiating Junctional Escape Rhythm
Junctional escape rhythm is often confused with other junctional rhythms and with ventricular escape rhythms. Use rate, QRS width, and rhythm context to differentiate them quickly. Pay close attention to the atrial activity relationship; if P waves are hidden or retrograde, combined with a narrow QRS and slow rate, it strongly points to a junctional rather than a ventricular origin.
| Rhythm | Typical Rate | QRS | P wave appearance | Key takeaway |
|---|---|---|---|---|
| Junctional escape rhythm | 40 to 60 bpm | Narrow | Absent or inverted, may be before, during, or after QRS | Protective backup when sinus node is suppressed |
| Accelerated junctional rhythm | 60 to 100 bpm | Usually narrow | Often absent or inverted | Same origin as junctional escape but faster |
| Junctional tachycardia | Over 100 bpm | Usually narrow | Often absent or inverted | Rapid junctional focus, may be symptomatic |
| Ventricular escape rhythm | 20 to 40 bpm | Wide | No consistent P wave relationship | Lower backup pacemaker with wider QRS |
Summary
A junctional escape rhythm acts as a vital physiological safety net when the sinus node fails due to heart disease, medication effects, or conduction abnormalities. Diagnosis relies on identifying a regular heart rate between 40 and 60 bpm, a narrow QRS complex, and absent or inverted P waves. Because it is a protective response, treatment focuses primarily on correcting the underlying cause and managing patient symptoms if cardiac output is compromised.
What are Junctional Rhythms?
To solidify your understanding of how the AV junction functions as a backup pacemaker, watch this comprehensive breakdown of What are Junctional Rhythms and how they fit into the broader category of cardiac arrhythmias.
More Free Resources to Keep You at Your Best
Editorial Note
ACLS Certification Association (ACA) uses only high-quality medical resources and peer-reviewed studies to support the facts within our articles. Explore our editorial process to learn how our content reflects clinical accuracy and the latest best practices in medicine. As an ACA Authorized Training Center, all content is reviewed for medical accuracy by the ACA Medical Review Board.

