Neonatal Resuscitation Algorithm
The Neonatal Resuscitation Program (NRP) establishes the standard of care for newborns requiring assistance at birth. Guided by the latest 8th edition guidelines, this protocol emphasizes the critical importance of the "golden minute", the first 60 seconds of life where initial assessment and support must occur to ensure positive outcomes.
Algorithm at a Glance
- Pre-delivery: antenatal counseling, a team briefing, and an equipment check.
- Neonatal team is present at the time of birth.
- Rapid initial assessment.
- Routine care proceeds in the event of a normal birth.
- Stimulation of the infant as indicated by assessment.
- Evaluation of the baby for apnea and bradycardia.
- Airway management.
- Monitoring of oxygen saturation with pulse oximetry.
- Minimal routine suctioning.
- CPR first, then epinephrine and volume expansion if not responding.
- Heart rate is the most important indicator of response to resuscitation efforts.
- Post-resuscitation briefing.
Understanding the Neonatal Resuscitation Algorithm
The neonatal resuscitation algorithm provides a systematic approach to evaluating and managing a newborn. It begins with antenatal counseling and moves rapidly through assessment, airway management, and potential pharmaceutical interventions. Watch the video below for a visual walkthrough of these critical steps.
What is the “Golden Minute” in Neonatal Resuscitation?
The “Golden Minute” is the critical first 60 seconds after birth. During this timeframe, the team must complete the initial steps of newborn care: drying, stimulating, and assessing the infant. If the baby is not breathing or is gasping, positive pressure ventilation (PPV) must be initiated by the end of this minute. Successful execution of these steps often prevents the need for more advanced resuscitative measures.
Key Updates from the 8th Edition NRP Guidelines
The 8th edition introduces several pivotal changes to optimize newborn care. Key updates include:
- Umbilical Cord Management: Delayed cord clamping (30–60 seconds) is recommended for vigorous term and preterm infants.
- Epinephrine Administration: Optimized dosing and timing protocols have been established for varying gestational ages.
- Temperature Management: Increased emphasis on maintaining normothermia in non-asphyxiated newborns.
Goals for Management
- A well-trained team is important for exceptional resuscitation.
- Oxygenation and ventilation are the priorities for infants needing support after birth, and these skills are reinforced in our online NRP certification course.
- Increased heart rate is a primary goal.
- The umbilical vein is the preferred source of vascular access in the newly born.
- Prevention of hypothermia is critical.
- If the newly born does not respond within 20 minutes, the clinician and family should discuss other options.
- Post-resuscitation care includes consideration for therapeutic hypothermia.
Neonatal Resuscitation Algorithm Explained
This algorithm guides the clinician when delivering neonatal resuscitation.
Box 1: Antenatal Counseling, Team Briefing, and Equipment Check
Preparation is the foundation of survival. The team must review maternal risk factors (antenatal counseling), assign specific roles (team briefing), and perform a comprehensive equipment check. Ensuring the flow-inflating bag, laryngoscopes, and suction are functional before birth minimizes delays during the crisis.
Box 2: Birth
The entire team assembles or has members readily available at the time of birth.
Box 3: Rapid Assessment
Using the mother’s history of the pregnancy and a tool such as the Ballard scale, the team determines if the baby is at term, if the muscle tone is good, and if the baby is breathing.
If the answer to all three questions is “yes,” the team proceeds to Box 4.
If the answer to at least one of the questions is “no,” the team proceeds to Box 5.
Box 4: Routine Care
If the baby is at term with good tone and is breathing or crying, the team allows the baby to remain in skin-to-skin contact with the mother. The team provides warmth and stimulation and monitors for changes.
Box 5: Increased Stimulation
If the answer to any of the three rapid assessment questions is “no,” the team moves the baby to a radiant warmer for possible resuscitation interventions. Team members warm the baby. They also dry and stimulate the baby to encourage breathing or crying. They open the airway and also suction the airway to clear secretions if needed.
Once the baby is born, the team must act quickly. The following video demonstrates the initial steps of warming, clearing the airway, and stimulating the newborn.
Box 6: Apnea or Bradycardia?
The team evaluates the neonate for apnea or gasping and for a heart rate below 100 bpm.
If the heart rate remains low or the infant is not breathing effectively, rescue breathing is the next intervention. This video details the correct technique for delivering breaths to a neonate.
If none of these symptoms, the team proceeds to Box 14.
If one or more of the symptoms are noted, the team proceeds to Box 7.
Box 7: Initiate Positive Pressure Ventilation (PPV)
The team begins PPV. Since respiratory problems cause most neonatal issues at birth, early respiratory intervention can often revive the infant. A team member places the infant on a pulse oximeter and considers an ECG monitor if that will not delay PPV.
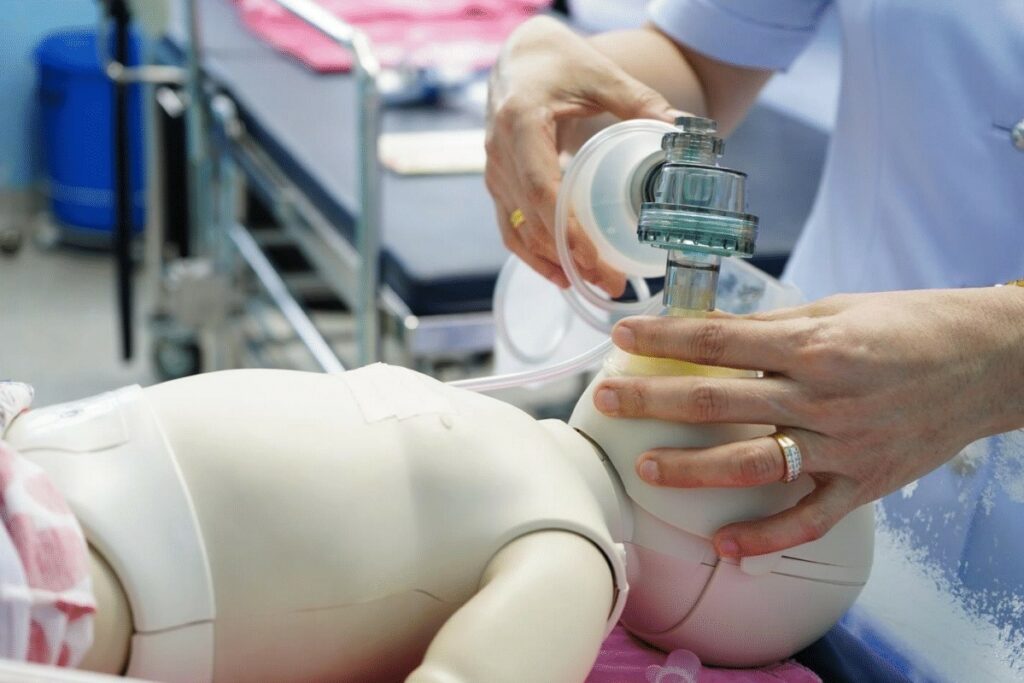
Positive pressure ventilation provides respiratory support if the baby is gasping or apneic.
Effective ventilation is skill-dependent. The video below guides you through proper Bag Valve Mask (BVM) usage during CPR to ensure adequate chest rise.
A common question in neonatal care involves equipment sizing. Here, we discuss whether infants can be safely fitted with an adult Ambu mask in emergency scenarios.
Box 8: Heart Rate < 100 bpm?
If PPV results in a heart rate > 100 bpm, the team proceeds to Box 16 for post-resuscitation care. If PPV does not result in a heart rate > 100 bpm, the team proceeds to Box 9.
Box 9: Ventilation Corrective Steps
The team evaluates ventilation technique and chest movement to determine if simple adjustments are needed to improve breath delivery. The clinician may consider the use of a laryngeal mask or endotracheal intubation. A team member places a cardiac monitor.
Box 10: Heart Rate < 60 bpm?
If the heart rate is 60 bpm or above, the team proceeds to Box 8.
If the heart rate is BELOW 60 bpm, the team proceeds to Box 11.
Box 11: Initiate High-Quality CPR
The team begins chest compressions at a rate of 100–120 per minute. The most qualified team member intubates the child, and the team provides synchronized compressions and PPV with a ratio of 3:1. The he procedures are reviewed in online NRP recertification courses.
Box 12: Heart Rate < 60 bpm?
If the heartrate remains < 60 bpm, the team proceeds to Box 13.
If the heart rate is > 60 bpm, the team proceeds to Box 8.
Box 13: Administer Epinephrine
If the heart rate falls below 60 bpm despite adequate ventilation, the team administers epinephrine every 3 to 5 minutes. If the heart rate is persistently < 60 bpm, the team considers possible causes, including hypovolemia and pneumothorax. If the clinician can determine the cause, immediate treatment is implemented.
Box 14: Labored Breathing or Persistent Cyanosis?
Team members evaluate the neonate for labored breathing and persistent central cyanosis.
Cyanosis is a bluish skin discoloration due to inadequate oxygenation.
Box 15: Provide Airway Management
The team positions the infant to provide an open airway and suctions any mucous from the mouth and airway. Routine suctioning is not recommended. The team attaches a pulse oximeter to the infant’s righthand and provides supplemental oxygen to increase the preductal oxygen saturation according to the target saturation for the time after birth:
- 1 minute = 60–65%
- 2 minutes = 65–70%
- 3 minutes = 70–75%
- 4 minutes = 75–80%
- 5 minutes = 80–85%
- 10 minutes= 85–95%
If the team cannot achieve these saturations, they consider applying CPAP.
If the infant’s heart rate goes below 100 bpm, the team proceeds to Box 9.
Box 16: Post Resuscitation and Team Briefing
When the neonate is stable, the team begins post-resuscitation care and conducts a team debriefing, concepts reinforced in online PALS recertification courses. This phase focuses on preventing secondary injury by maintaining normothermia, monitoring blood glucose, and ensuring stable oxygenation/ventilation while preparing for transfer to the NICU or nursery.
Debriefing Protocols:
Immediately following the event, the team should conduct a structured debriefing. This is a short, non-punitive discussion designed to improve future performance. Key questions to address include:
- What went well? (e.g., “Clear leadership,” “Timely intubation”)
- What could be improved? (e.g., “Delay in getting epinephrine,” “Equipment malfunction”)
- System Issues: Were supplies missing or hard to find?
Communication Strategies:
Effective post-resuscitation communication relies on closed-loop communication and accurate handoffs. When transferring care, utilize standardized tools like SBAR (Situation, Background, Assessment, Recommendation) to ensure critical details—such as medications administered and response to intubation—are not lost. Finally, the team must update the family with clear, honest information regarding the infant’s status and the interventions performed.
Editorial Note
ACLS Certification Association (ACA) uses only high-quality medical resources and peer-reviewed studies to support the facts within our articles. Explore our editorial process to learn how our content reflects clinical accuracy and the latest best practices in medicine. As an ACA Authorized Training Center, all content is reviewed for medical accuracy by the ACA Medical Review Board.