Cardiac Tamponade
This comprehensive guide covers the critical emergency of cardiac tamponade. Designed for ACLS providers and emergency clinicians, this article explores the pathophysiology of pericardial fluid accumulation, how to recognize classic clinical signs like Beck’s Triad, and the life-saving interventions required to restore cardiac output.
ACLS Certification Association videos have been peer-reviewed for medical accuracy by the ACA medical review board.
Article at a Glance
- A Time-Sensitive Emergency: Cardiac tamponade is a critical, life-threatening condition requiring urgent decompression to prevent obstructive shock and cardiac arrest.
- Cardiac tamponade is pressure on the heart due to fluid build-up in the pericardium.
- Clinicians treat the signs and symptoms of cardiac tamponade until a pericardiocentesis is performed.
- Clinicians will learn the unique signs and symptoms and nursing care of cardiac tamponade.
What is cardiac tamponade?
Cardiac tamponade is a severe form of obstructive shock caused by the accumulation of fluid, blood, or pus in the pericardial space. As this fluid builds up, it places immense pressure on the heart. Because the ventricles are physically squeezed from the outside, they cannot fully expand or relax during diastole. This severely impaired filling directly leads to a drastic drop in stroke volume and decreased cardiac output, depriving the body’s vital organs of oxygenated blood.
To fully understand this, we must look at the anatomy of the pericardial sac. The pericardium is a double-walled, fibrous sac surrounding the heart, consisting of the visceral pericardium (touching the heart muscle) and the parietal pericardium (the tough outer layer). Normally, there is a very small amount of lubricating fluid (15-50 mL) between these layers. Because the outer parietal layer is highly fibrous and inelastic, any rapid accumulation of extra fluid quickly builds pressure inward against the heart rather than stretching outward.
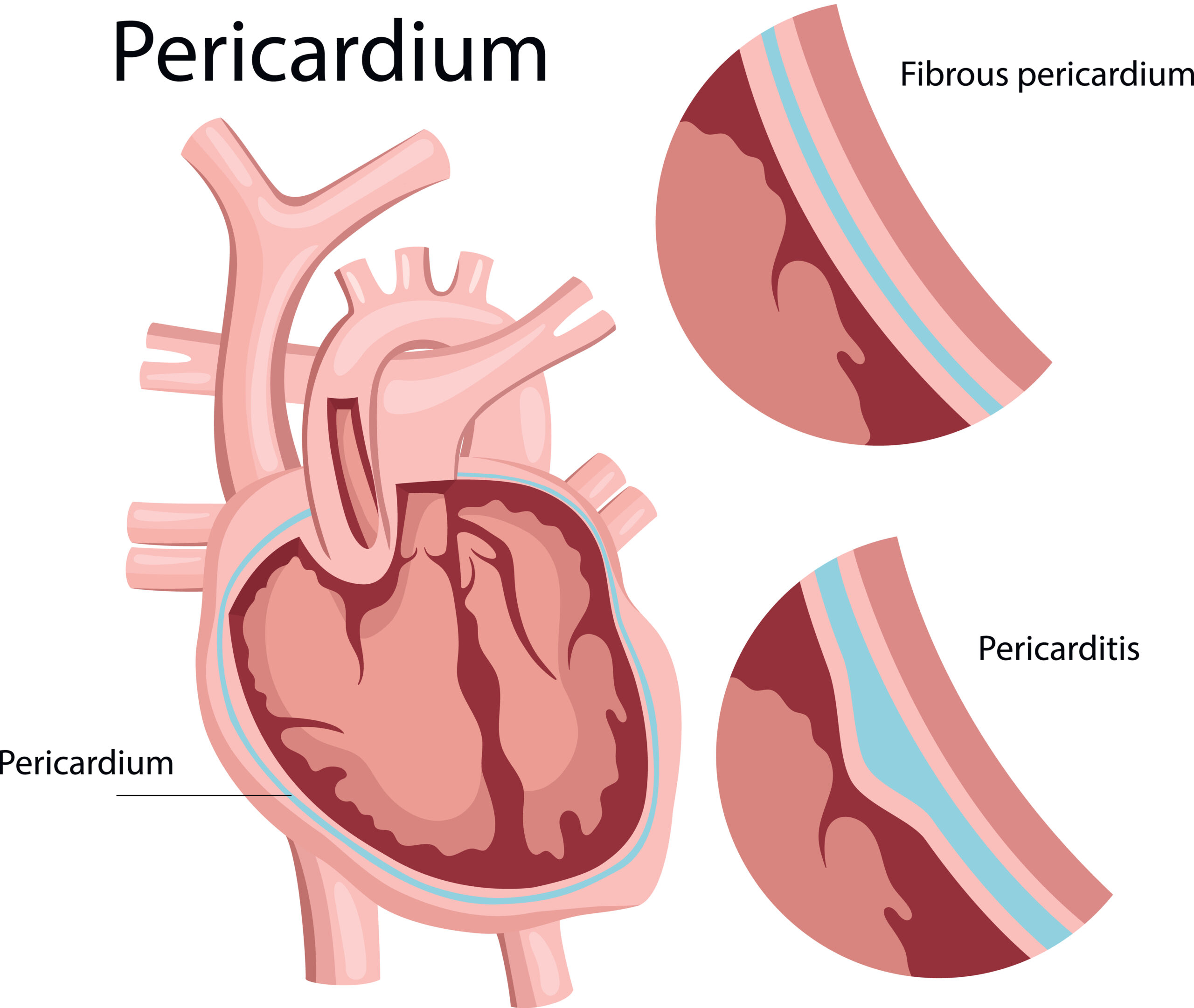
The pericardium is the sac surrounding the heart.
To visualize how this fluid accumulation physically compresses the heart and leads to rapid hemodynamic collapse, watch our detailed lesson on Cardiac Tamponade.
Acute Cardiac Tamponade
Acute tamponade occurs rapidly, often over minutes to hours. Because the pericardial sac has no time to stretch, even small amounts of rapid fluid accumulation (e.g., 100-200 mL of blood from trauma) can trigger life-threatening tamponade physiology.
Subacute Pericardial Tamponade
Subacute tamponade develops more slowly, over days to weeks. Because the pericardium has time to gradually stretch and adapt, it can sometimes accumulate over 1,000 mL of fluid before the pressure overwhelms the heart and causes hemodynamic compromise.
What are the symptoms of cardiac tamponade?
Because cardiac tamponade causes a severe drop in cardiac output, patients will present with symptoms of systemic shock. Common symptoms include:
- Severe dyspnea (difficulty breathing) and tachypnea (rapid breathing)
- Tachycardia (fast heart rate as the body attempts to compensate)
- Chest pain (often sharp, radiating to the neck or back)
- Altered mental status, confusion, or overwhelming anxiety
- Cold, clammy extremities
What causes cardiac tamponade?
To understand what causes tamponade, it is important to first understand its relationship with a pericardial effusion. A pericardial effusion is simply the abnormal buildup of extra fluid in the pericardial space. An effusion is a condition, whereas cardiac tamponade is the catastrophic physiological event that occurs when that effusion grows large enough, or fast enough, to choke the heart.
Cardiac tamponade can result from a wide variety of medical and traumatic etiologies, including:
- Trauma: Blunt force trauma to the chest or penetrating injuries (stab/gunshot wounds) causing rapid bleeding into the sac.
- Iatrogenic (Post-Procedure): Accidental cardiac perforation during procedures like pacemaker placement, catheter ablation, or central line insertions.
- Malignancy: End-stage lung, breast, or other metastatic cancers can spread to the pericardium and cause rapid fluid shifts or directly compress the heart.
- Systemic Diseases: Conditions like severe kidney failure (uremia) or autoimmune diseases (lupus, rheumatoid arthritis).
- Aortic Dissection: A ruptured aortic aneurysm can rapidly bleed into the pericardial space.
Pericarditis
One of the most prominent medical causes of pericardial effusion, and subsequently cardiac tamponade, is pericarditis (an inflammation of the pericardium). Inflammation is typically caused by a viral, bacterial, or fungal infection, which prompts an immune response that produces excess fluid between the visceral and parietal layers. Other drivers of pericarditis include recent heart attacks (Dressler’s syndrome) and localized chest radiation.
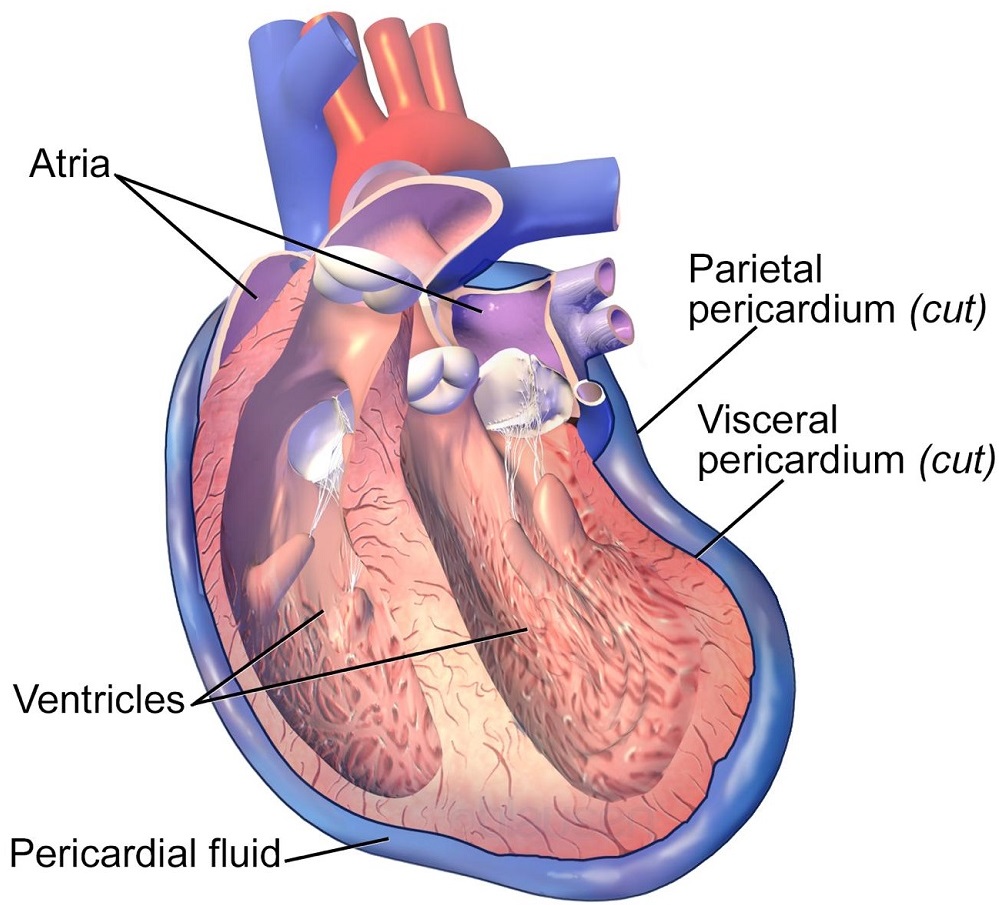
Pericarditis can cause excess fluid to build up between the visceral and parietal pericardium.
Read: Beta-Blockers vs. Beta-Agonists
Beck’s Triad and Pulsus Paradoxus
To accurately diagnose cardiac tamponade at the bedside, clinicians look for key exam signs. However, it is critical to note that these classic findings are not always present simultaneously, especially in rapidly developing acute trauma, and their absence should not be the sole basis for ruling out clinical suspicion.
Beck’s Triad
Beck’s triad describes three classic clinical signs/findings heavily associated with severe cardiac tamponade:
- Hypotension: Dropping blood pressure due to drastically reduced stroke volume.
- Muffled heart sounds: The thick layer of pericardial fluid dampens the acoustic sound of the heartbeat when listening with a stethoscope.
- Jugular vein distention (JVD): Because the right side of the heart is compressed and cannot accept incoming venous blood, the pressure backs up, causing the veins in the neck to bulge visibly.
The jugular veins visibly bulge at the neck due to blood backing up from the compressed heart.
Pulsus Paradoxus
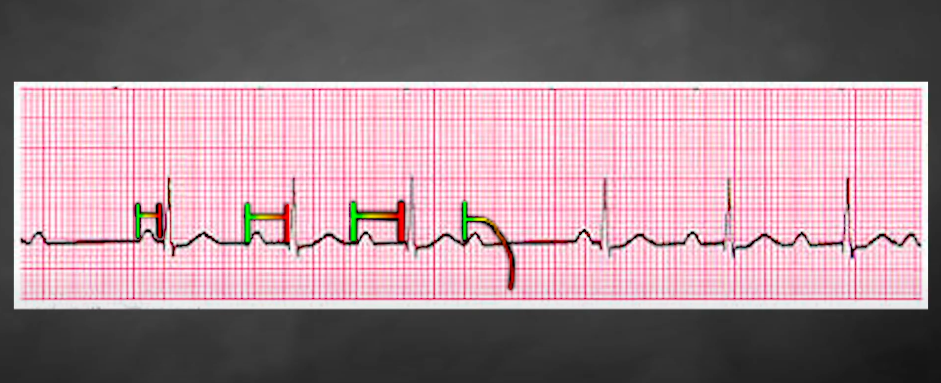
Pulsus paradoxus is an abnormally large decrease in systolic blood pressure (greater than 10 mm Hg) during inspiration. Clinicians can observe this by slowly deflating a manual blood pressure cuff and noting the pressure difference between when sounds are heard only during expiration versus when they are heard continuously.
[Image demonstrating pulsus paradoxus on an arterial pressure waveform]
This occurs because the fluid accumulated inside the pericardial space tightly restricts the entire heart. During a normal breath in (inspiration), negative pressure draws more blood into the right ventricle. Because the restrictive fluid prevents the outer heart wall from expanding, the right ventricle’s expanding wall bows inward, squashing the left ventricle. This decreases left ventricular filling, severely dropping stroke volume and systolic pressure with every breath. Like Beck’s Triad, pulsus paradoxus may not be present in every scenario (such as if the patient is severely hypotensive) and should be interpreted alongside the full clinical picture.
Pathophysiology: Decreased Cardiac Output and Right-sided Heart Failure
Cardiac tamponade creates a severe mechanical obstruction to the heart’s natural pumping cycle. While some systemic diseases might cause both right-sided heart failure and pericardial effusions, the classic presentation of right-sided heart failure in tamponade is a direct consequence of the heart being squeezed, not the primary cause of the fluid itself.
Because the right side of the heart operates at lower pressures than the left, the thin-walled right atrium and right ventricle are the first to collapse inward under the weight of pericardial fluid. The compressed right ventricle isn’t able to accept the incoming venous return. Because this blood cannot enter the heart, it backs up into the peripheral systemic circulation, resulting in profound right-sided failure signs, such as jugular vein distension (JVD).
Ultimately, this impaired diastolic filling drastically decreases stroke volume (the amount of blood pumped out per beat). With less blood leaving the heart, systemic perfusion drops, causing profound hypotension. This mechanical failure can be understood through the core hemodynamic equations:
Cardiac output = heart rate × stroke volume
Blood pressure = cardiac output × systemic vascular resistance
Because the stroke volume has plummeted due to compression, the cardiac output falls, taking the blood pressure down with it. The body attempts to compensate by increasing the heart rate (tachycardia) and clamping down blood vessels (increasing systemic vascular resistance), but these are temporary, failing measures until the physical fluid pressure is relieved.
How is cardiac tamponade treated?
Cardiac tamponade is a mechanical problem requiring a mechanical solution. The only definitive treatment is urgent drainage of the pericardial sac. While preparing for drainage, clinical care is directed toward temporizing supportive interventions to manage the severely decreased cardiac output and prevent impending cardiac arrest.
Temporizing and Supportive Management Checklist:
- Airway and Breathing: Monitor the airway closely. If cardiac output is so diminished that the brain is not being perfused, the patient may become lethargic, somnolent, or confused, and may lose the ability to protect their own airway. Deliver supplemental oxygen as necessary.
- Positioning: Position the patient upright to facilitate maximum lung expansion, as the lungs are not being fully perfused.
- Hemodynamic Monitoring: Monitor heart rate, blood pressure, and continuous ECG frequently during the acute phase. These patients can rapidly crash into profound shock, and lethal dysrhythmias can result.
- IV Fluids & Inotropes: Administering IV fluid boluses can help push volume back into the right side of the compressed heart, temporarily buying time and supporting blood pressure. Occasionally, physicians may order dobutamine or other positive inotropic drugs to help the heart contract more efficiently.
- Lab and Output Checks: Perform hourly measurements of fluid intake and output. If the kidneys aren’t perfused, they won’t produce urine. A rapid drop in urine output indicates worsening cardiac failure. Monitor arterial blood gases (ABGs) to ensure the acid-base balance is not rapidly deteriorating.
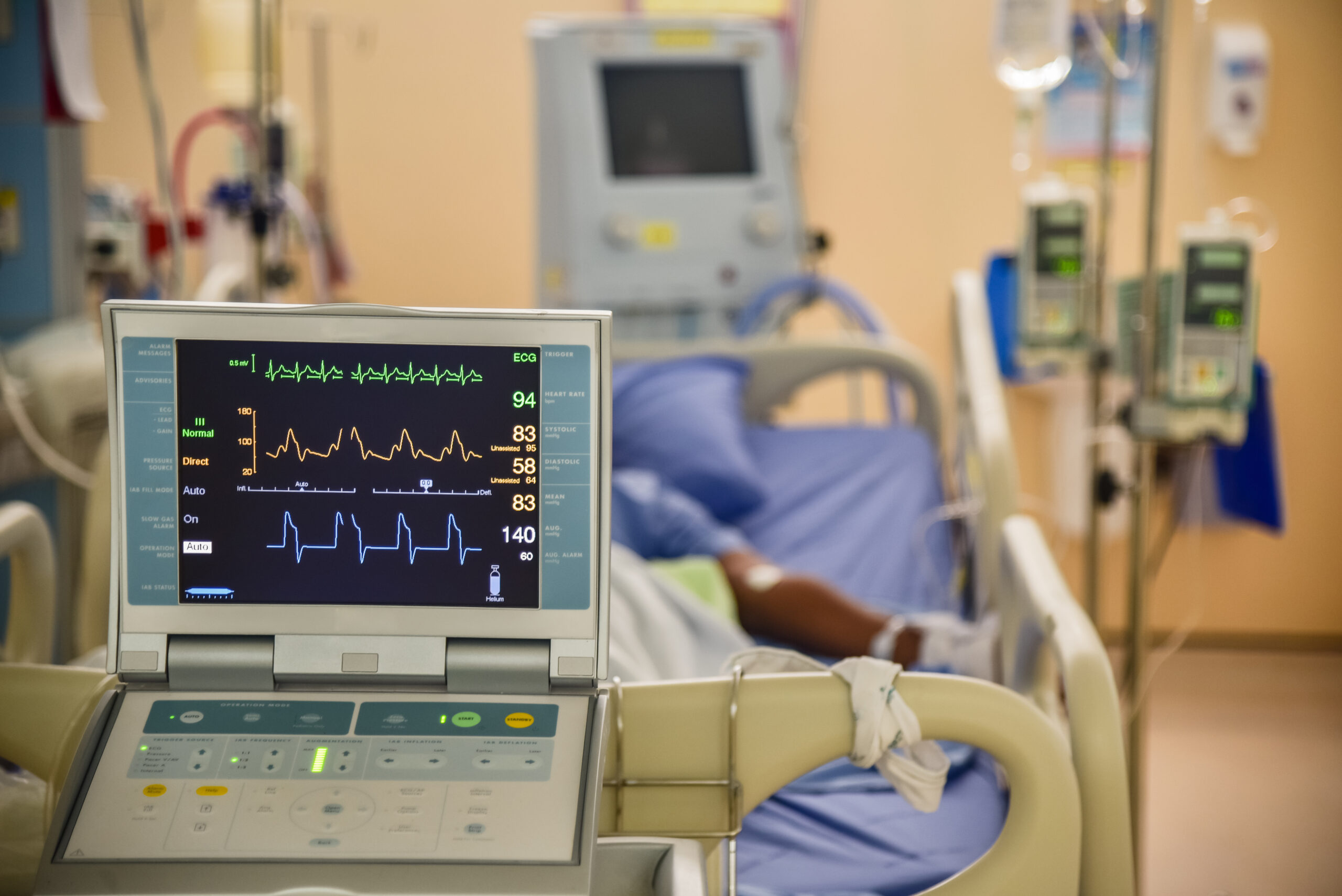
Monitor the patient’s vitals and symptoms aggressively until the patient can receive definitive drainage.
Definitive Escallation: Fluid Drainage
If the patient is highly unstable, a pericardiocentesis is a critical, life-saving intervention. Using ultrasound guidance, a clinician inserts a long needle into the pericardial space to physically drain the fluid, allowing the heart to instantly expand and resume pumping. In cases of traumatic tamponade (such as a stab wound) or recurring effusions, surgical drainage (such as a pericardial window or thoracotomy) in the operating room may be required to evacuate clotting blood and repair the heart wall.
Complications of Tamponade
Patients with cardiac tamponade require constant monitoring because decompensation happens rapidly. If the pressure is not relieved, major complications include:
- Cardiogenic and obstructive shock
- Pulmonary edema
- Pulseless Electrical Activity (PEA) Cardiac Arrest
- Death
Summary
Cardiac tamponade is a life-threatening emergency caused by the rapid buildup of fluid inside the pericardial sac. This pressure physically crushes the heart, drastically reducing stroke volume and cardiac output. Clinicians must rapidly identify key diagnostic indicators like Beck’s Triad (hypotension, JVD, muffled heart sounds) and pulsus paradoxus. Because conservative care with IV fluids is only temporary, definitive treatment requires urgent mechanical drainage via a pericardiocentesis or surgery.
While preventing cardiac tamponade itself is often not possible, especially in cases of sudden trauma, early detection and treatment of underlying pericardial effusions, systemic diseases, and inflammatory conditions can significantly reduce a patient’s risk of progressing into catastrophic hemodynamic collapse.
More Free Resources to Keep You at Your Best
Editorial Note
ACLS Certification Association (ACA) uses only high-quality medical resources and peer-reviewed studies to support the facts within our articles. Explore our editorial process to learn how our content reflects clinical accuracy and the latest best practices in medicine. As an ACA Authorized Training Center, all content is reviewed for medical accuracy by the ACA Medical Review Board.