Addison Disease vs. Cushing Disease
Disorders of the adrenal cortex can lead to life-altering conditions. This guide explores the critical differences between Addison’s disease (adrenal insufficiency) and Cushing’s disease (hypercortisolism). We cover the distinct symptoms—from hypotension and hyperpigmentation in Addison’s to the “moon face” and hypertension in Cushing’s—along with their specific diagnostic tests and nursing interventions.
ACLS Certification Association videos have been peer-reviewed for medical accuracy by the ACA medical review board.
Article at a Glance
- Addison disease and Cushing disease are disorders of the adrenal cortex.
- A unique presentation in Addison disease is hyperpigmentation. Two unique presentations in Cushing disease are a moon face and a buffalo hump.
- Read on to learn more about the pathophysiology, signs and symptoms, and nursing care of Addison disease and Cushing disease.
Introduction to Addison Disease and Cushing Disease
The adrenal glands are small but powerful organs that regulate essential functions like blood pressure, metabolism, and the body’s response to stress. When these glands malfunction, the consequences are profound. This article addresses disorders of the adrenal cortex, specifically comparing the insufficiency of Addison’s disease against the excess hormone production of Cushing’s disease. Understanding these opposing conditions is vital for effective diagnosis and patient care. One way to remember the three hormones that the adrenal cortex produces is to use the mnemonic “three silly sisters,” which are “salt, sugar, and sex.” The adrenal cortex produces:
- “Salt,” which represents aldosterone.
- “Sugar,” which represents cortisol.
- “Sex” hormones, which represent the androgens.
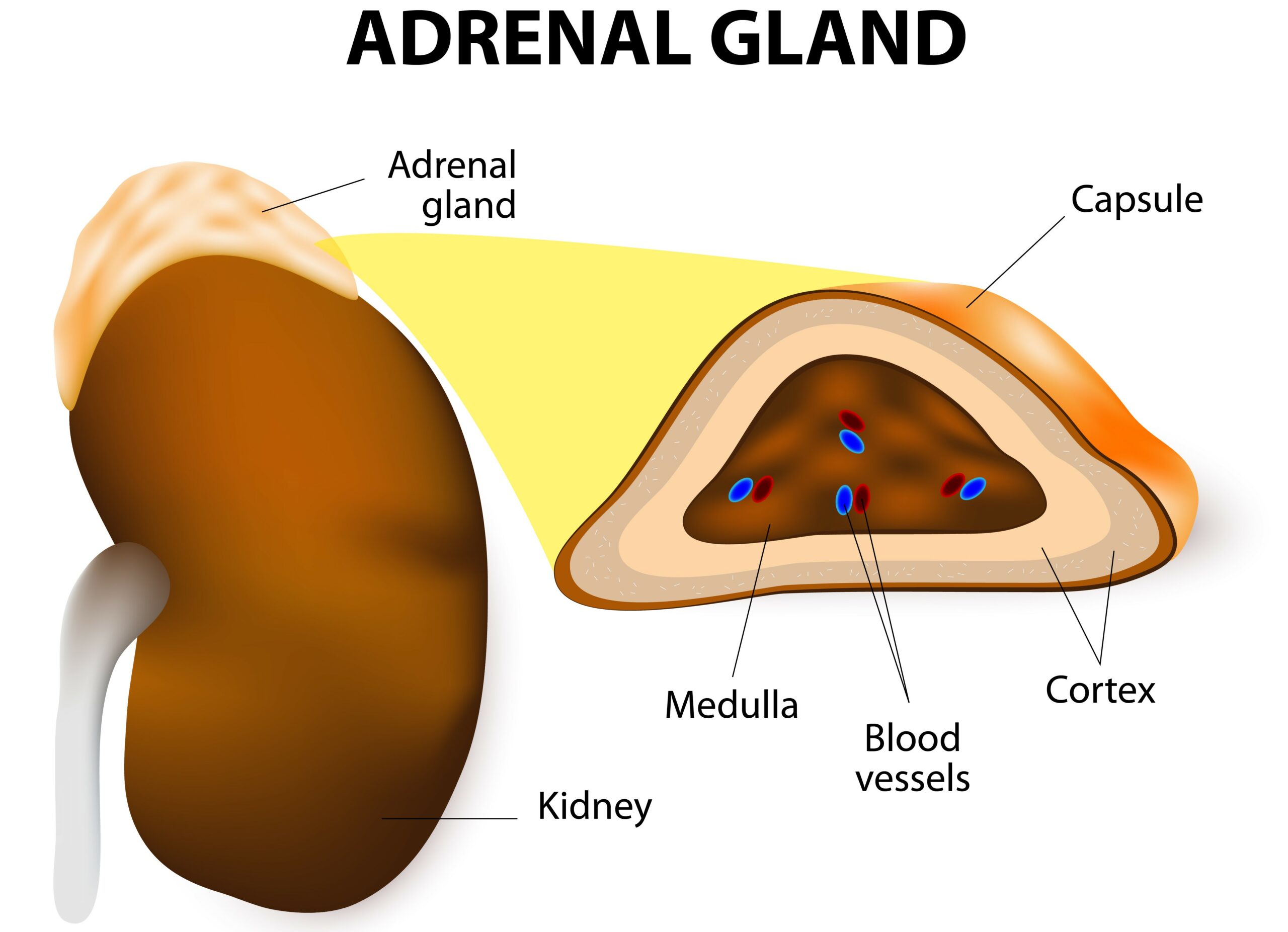
The adrenal glands are located on top of the kidneys.
Addison’s Disease
With Addison disease, the body is lacking hormones, or it is lacking the salt, sugar, and sex. That means the body is low on aldosterone, cortisol, and androgens, respectively.
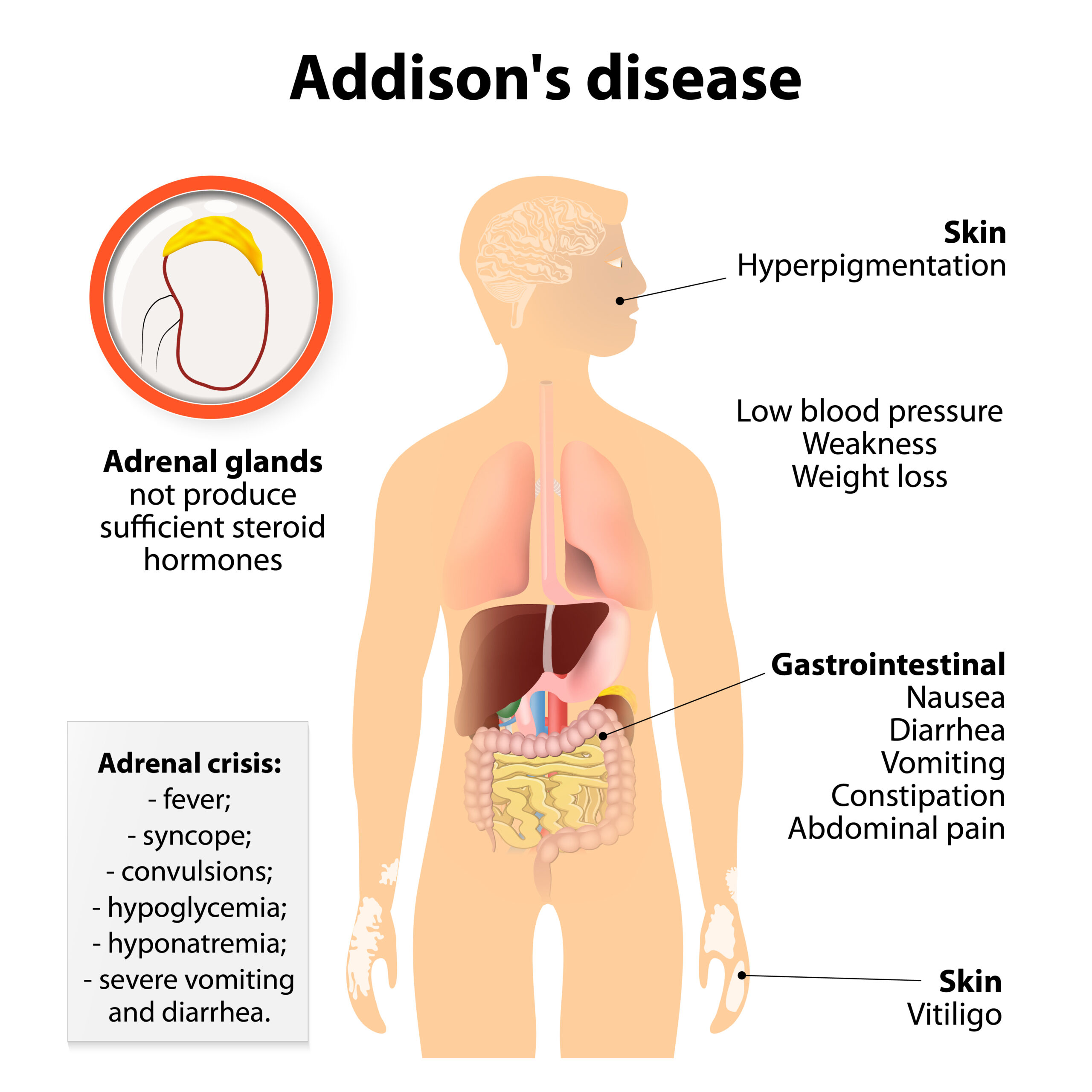
In Addison disease, the adrenal glands do not produce sufficient hormones.
It is important to understand what these hormones do in the body to know what signs and symptoms of Addison’s disease to look for in patients.
Diagnosis of Addison’s Disease
Diagnosing Addison’s involves confirming low hormone levels. Key tests include the acth stimulation test, where synthetic ACTH is injected to see if the adrenal glands respond to produce cortisol. If cortisol levels remain low, primary adrenal insufficiency is confirmed. Blood tests will also typically reveal hyponatremia (low sodium) and hyperkalemia (high potassium).
Risk Factors for Addison’s Disease
The primary risk factor is having an autoimmune disease, as the immune system may attack the adrenal cortex. Other risks include chronic infections (like tuberculosis or HIV), history of cancer with metastasis to the adrenals, or the use of blood-thinning medications that could lead to adrenal hemorrhage.
Aldosterone is known as the salt-water hormone. If the body is low on salt, which is aldosterone, then the patient will present with hyponatremia.
Hypotension will also present with hyponatremia, because without aldosterone, the body cannot retain salt and water.
Additionally, potassium and sodium have an inverse relationship. If the patient is hyponatremic, they will also be hyperkalemic. Therefore, it is necessary to monitor potassium levels in patients with Addison disease.
Finally, if the body is low on sugar, which represents cortisol, the body is hypoglycemic. Cortisol stimulates the production of glucose. Patients with Addison disease will have a low blood glucose level because there is less cortisol produced.
Another unique presentation of Addison disease is the hyperpigmentation of the skin. The pathophysiology behind this presentation is that adrenocorticotropic hormone (ACTH) is out of balance in Addison disease. ACTH stimulates the melanocytes to produce melanin, giving patients with Addison disease a tanned look.
Read: SIADH vs. Diabetes Insipidus
Nursing Role in Addison Disease
When someone has Addison disease, the main signs and symptoms to watch for are:
- Hypotension. The patient will have a low serum cortisol level and low serum sodium. The patient may develop tachycardia through a compensatory mechanism.
- Hyponatremia. The patient will likely be hyponatremic due to the lack of aldosterone.
- Hyperkalemia. The patient may be hyperkalemic due to hyponatremia.
- Dysrhythmias. Because potassium is affected, it is necessary to watch for dysrhythmias.
Patients with Addison disease need to wear a medical alert bracelet. If they go into an Addisonian crisis (also known as an adrenal crisis), they can become so hypotensive that they have severe mental status changes and possibly go into a coma.
The primary treatment for Addison’s disease consists of administering hydrocortisone and hormone replacement. Patients will need to receive replacement therapy for aldosterone, cortisol, and androgens, because without the replacement of these hormones, they will be perpetually hypoglycemic, hyponatremic, and hypotensive.
Cushing Disease
As stated above, Cushing disease is the opposite of Addison disease. Therefore, where Addison disease presents with low hormone levels, Cushing disease presents with too much “salt, sugar, and sex.” Someone with Cushing disease will have too much aldosterone, cortisol, and androgens, respectively.
What that means is that the signs and symptoms of cushing disease will present as the opposite of Addison’s; for example, excess cortisol often leads to rapid weight gain.
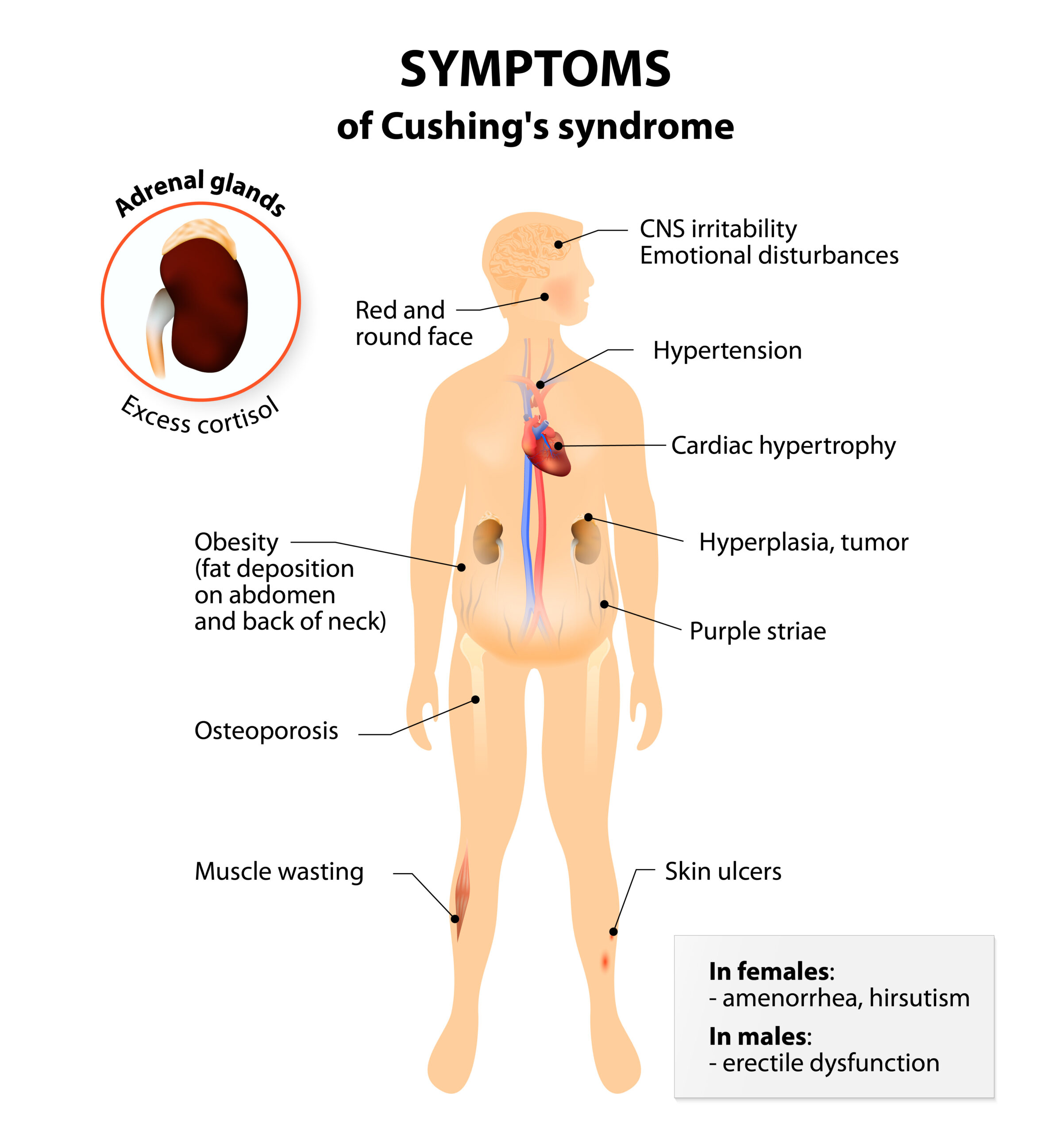
Cushing syndrome and Cushing disease are characterized by an excess of hormones.
People with Cushing disease will be hypernatremic because of the excess aldosterone telling the body to retain sodium and fluid. They will be hypertensive and will present with edema. A way to remember Cushing disease is the phrase “Cushy Carl.”
One characteristic of Cushing disease is hyperglycemia because of the excess cortisol. Patients will be hypokalemic due to hypernatremia and the inverse relationship between sodium and potassium. They need to be monitored for dysrhythmias due to hypokalemia.
Patients with Cushing disease also have physical changes. The unique physical characteristics of Cushing disease are:
- Moon face
- Buffalo hump
The excess cortisol in the body causes the deposits of adipose tissue in various places around the body. However, the face and area between the shoulders on the backside are two notable locations where fat deposits develop.
Other physical changes in Cushing disease are due to the overproduction of sex hormones. Females with Cushing disease may grow facial hair, while males develop gynecomastia. The hormone imbalance causes physical changes where females take on male characteristics and males take on female characteristics.
Patients with Cushing disease tend to be fatigued, possibly depressed, and mentally cloudy. They may feel lethargic. They may not want to get out of bed and do anything. An excess of cortisol has that effect on the body.
Diagnosis of Cushing Disease
Diagnosis focuses on confirming hypercortisolism. The 24-hour urinary free cortisol test is a primary screening tool. Another method is the dexamethasone suppression test, where a patient takes a steroid pill at night, and cortisol is measured the next morning; in Cushing’s, cortisol levels will remain high despite the suppression attempt.
Risk Factors for Cushing Disease
The most significant risk factor is the long-term use of oral corticosteroid medications (e.g., prednisone) for conditions like asthma or arthritis. Other risks include having pituitary or adrenal tumors (adenomas) that secrete excess ACTH or cortisol.
Nursing Role in Cushing Disease
What is the cure for Cushing disease? If the adrenals are the source, they may need to be removed. Radiation is another option, and some medications help control excessive cortisol.
The role of the nurse is to treat the symptoms. Insulin is administered to lower glucose, antihypertensives are administered to reduce blood pressure, and diuretics are given to control fluid overload. However, the disease is not cured until the source is identified and addressed.
Differential Diagnosis: How Doctors Distinguish Between Addison’s and Cushing’s
The initial assessment relies on identifying the opposing symptomatic profiles: the “wasting” phenotype of Addison’s versus the “excess” phenotype of Cushing’s.
Diagnostic Pathways:
- Electrolyte Panels: Addison’s is characterized by low sodium and high potassium, whereas Cushing’s often presents with high sodium and low potassium.
- Confounding Factors: Obesity and metabolic syndrome can mimic Cushing’s (pseudo-Cushing’s). Doctors must rule these out by testing cortisol rhythms, which are disrupted in true Cushing’s disease but often preserved in simple obesity.
To understand the differences between Cushing disease and Cushing syndrome, it is important to understand their source. The hypothalamus secretes a hormone that stimulates the anterior pituitary gland. The anterior pituitary gland secretes an adrenocorticotropic hormone or ACTH. ACTH speaks directly to the adrenal cortex. Addison disease tends to be an autoimmune disorder in the adrenal cortex. However, Cushing has different etiologies, which are defined as Cushing disease and Cushing syndrome. These are two similar but different disorders: For example, a patient with chronic obstructive pulmonary disease may develop Cushing syndrome after taking long-term corticosteroids. They present with the same signs and symptoms but may not have a primary disorder of the adrenal cortex. Addison disease and Cushing disease are both disorders of the adrenal cortex. Where Addison disease presents with low levels of aldosterone, cortisol, and androgens, Cushing disease presents with high levels. As these disorders are opposites of one another, the provider needs to understand how to identify which disease the patient has and know how to treat or cure it.Cushing Disease versus Cushing Syndrome
Addison’s Disease vs Cushing’s Disease: A Quick Summary
Addison’s disease and Cushing’s disease represent opposite ends of the adrenal spectrum. While Addison’s is a life-threatening deficiency requiring lifelong hormone replacement, Cushing’s is a condition of excess often requiring surgical intervention. The table below summarizes these key differences:
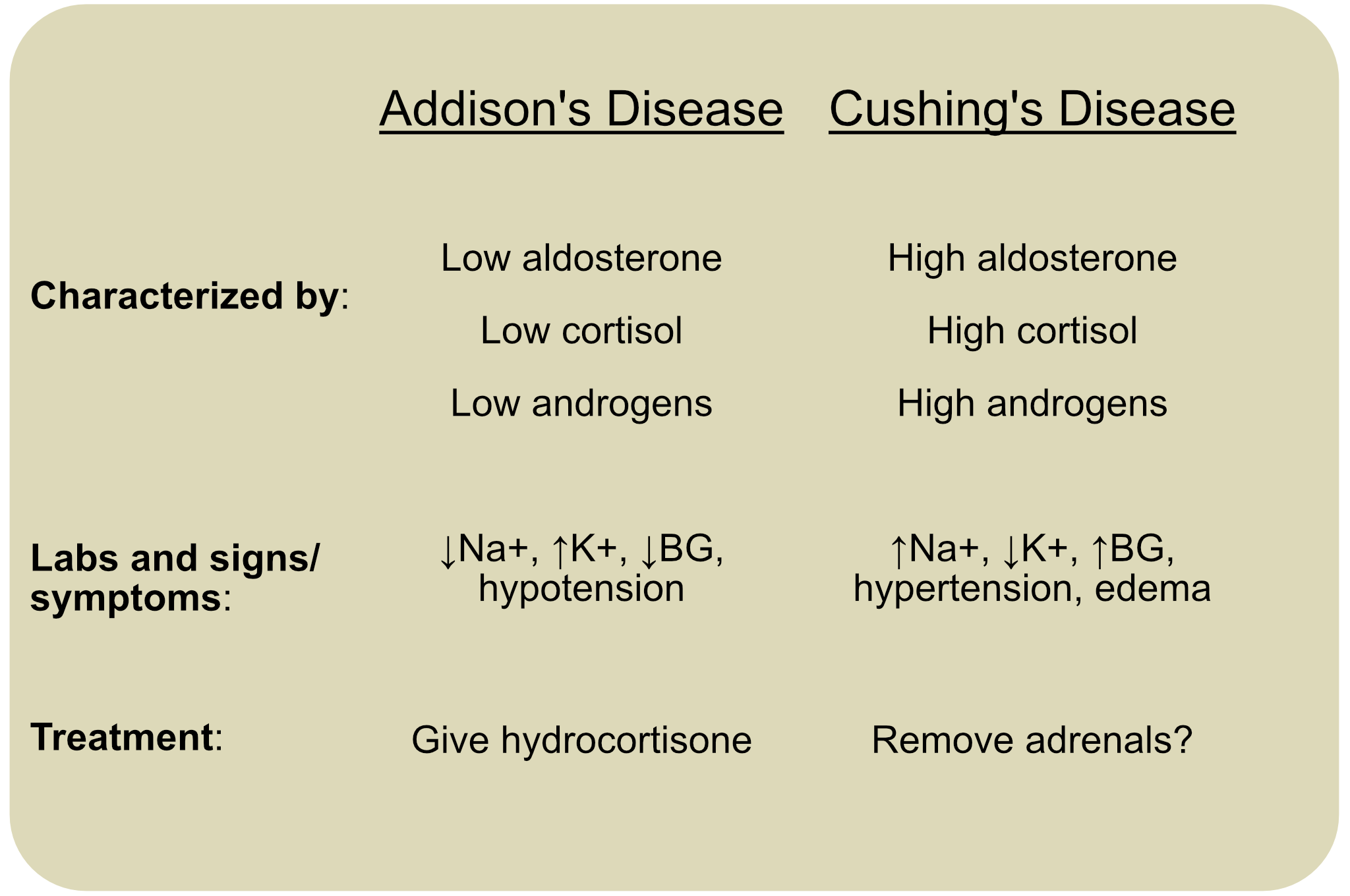
Addison disease and Cushing disease summary table
More Free Resources to Keep You at Your Best
Editorial Note
ACLS Certification Association (ACA) uses only high-quality medical resources and peer-reviewed studies to support the facts within our articles. Explore our editorial process to learn how our content reflects clinical accuracy and the latest best practices in medicine. As an ACA Authorized Training Center, all content is reviewed for medical accuracy by the ACA Medical Review Board.